What Can Cause a Rash Around the Eyes?
Medically reviewed by Johnstone M. Kim, MD
A skin rash around your eyes, or eyelid dermatitis, can signify various conditions. Allergies, irritation, skin conditions like psoriasis and atopic dermatitis (eczema), infections, and autoimmune diseases are among the causes of patches of red, irritated skin that can impact your self-image and quality of life. It may also be a sign of a more severe condition.
Getting rid of a rash around the eyes often means treating the underlying cause, with healthcare providers tailoring treatments to individual cases. This article discusses why you may have a rash around your eyes, treatment options, and signs you should call a healthcare provider.
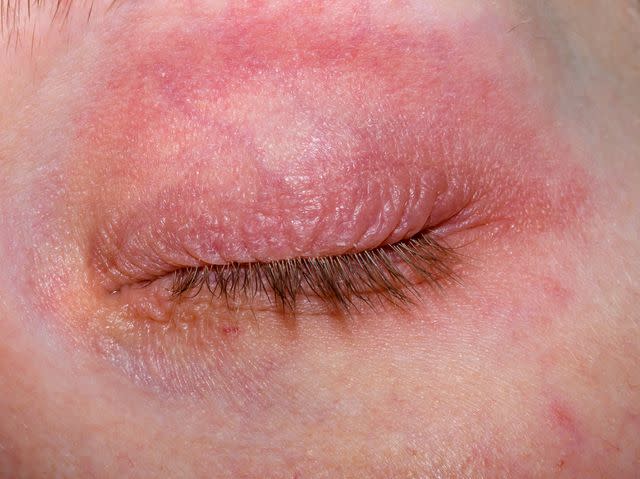
Pawel Kacperek / Getty Images
Atopic Dermatitis
Atopic dermatitis (eczema) is a common inflammatory disease that causes rashes and affects the skin’s ability to retain moisture. People with eczema have persistent symptoms, which go through active and dormant periods. Common signs include:
Itchiness (pruritis)
Dry, discolored patches of skin that appear
Rashes that produce clear fluid and bleed easily
Hyperkeratosis, hardened and thickened skin
Though more common in infants and children, eczema affects people of all ages. Your age can also influence the appearance and location of atopic dermatitis and its associated symptoms.
In Babies
In newborns and infants up to 2 years old, eczema causes the redness, rashes, or patches of discolored, dry skin. The face, scalp, or soft areas of skin around their joints (such as the elbows and knees) are most commonly affected.
In Children
In childhood and early adolescence, the rash is red and often thickened, bleeding easily or oozing clear fluid when scratched. It most often appears on the elbows, inside of the knee, neck, or ankles.
In Adults
Eczema rashes in older teenagers and adults are darker-colored brown or red. If scratched, they may start bleeding, scabbing, or crusting. In addition to the neck, knees, elbows, and ankles, rashes often spread to the hands and feet. Eyelid dermatitis due to eczema is most common among adults, and the skin below the eye may develop an extra fold (a Dennie-Morgan fold) or grow darker.
Treatment
Treatment for atopic dermatitis focuses on reducing the severity and frequency of symptoms and includes the following:
Using moisturizers, especially after bathing
Taking diluted bleach baths twice a week, adding 2 to 4 ounces of regular bleach to 40 gallons of water
Wet wrap therapy, laying wet gauze over affected areas for prolonged periods
Topical corticosteroids like Deltasone (prednisone) and Sernivo (betamethasone)
Topical calcineurin inhibitors, such as Protopic (tacrolimus)
Phototherapy, using a special light to expose skin to ultraviolet B (UVB) rays
Contact Dermatitis
Contact dermatitis is a rash that occurs due to something in the environment. The symptoms appear as an allergic reaction, known as allergic contact dermatitis, or a response to skin irritation, called irritant contact dermatitis. Rashes due to contact dermatitis, which can cause eyelid dermatitis, have the following characteristics:
Red bumps that may form into blisters
Warm or hot to the touch, tender or sore
Leaking or draining fluid, crusting, or scabbing
Sensitivity or rawness, scaly skin
Irritant Contact Dermatitis
Irritant contact dermatitis rashes occur when skin comes into contact with an irritating substance or friction from skin rubbing against skin or material.
This type may also cause burning or pain in affected areas. In some cases, streaky, red rashes develop where the irritating substance touches the skin, typically appearing one to two days after contact. Irritant contact dermatitis can also cause chronic swelling and cracking of the skin.
Common triggers include:
Hair dye
Pesticides, weed killers, specific gardening or farming products
Rubber gloves
Certain shampoos or cleaning products
Cleaning products
Industrial or household chemicals, such as solvents, acids, or alkali
Cement
Allergic Contact Dermatitis
Allergic contact dermatitis arises when exposed to an allergen that sets off an allergic reaction—itchy, swollen, and red patches form, which can become blisters and ooze. The symptoms develop on areas of directly exposed skin within 24 and 48 hours. Sometimes, airborne allergens can also lead to rashes.
You can be allergic to many different substances that are both naturally occurring and manufactured. Examples include the following:
Certain metals (commonly nickel)
Fragrances found in shampoos, soaps, or beauty products
Poison ivy, poison oak, or poison sumac
Certain fabrics
Certain types of sunscreen
Treatment
Depending on the underlying cause, treatments for contact dermatitis include:
Thoroughly cleaning and washing affected areas with soap and water
Using moisturizers and emollients on the skin to prevent dryness and spur repair
Medications, including topical corticosteroids and calcineurin inhibitors
Applying anti-itch lotions to ease symptoms
Seborrheic Blepharitis
Seborrheic blepharitis is an inflammatory skin condition that affects the lids and skin around the eyes. It occurs due to overactive sebaceous glands—organs found in hair follicles that produce sebum, which preserves skin moisture. Elevated sebum levels allow bacteria to form, which cause the following symptoms:
Greasy flakes or dandruff-like crusts around the eyelids
Feeling like something is stuck in your eyes
Itchiness, discomfort
Skin redness
Complications like vision blurring, missing eyelashes, and inflammation that spreads to the other eye
Treatment
Seborrheic blepharitis can't be cured with treatment, but there are options to manage the symptoms. A healthcare provider will first identify the bacteria causing your symptoms, evaluate their severity, and recommend treatment based on those two factors. Standard treatment approaches include:
Hygiene practices to keep the affected area clean
Temporarily switching from contacts to glasses or stopping the use of eye makeup to limit recurrence
Ointments or artificial tear solutions to treat the affected area
Oral antibiotics to treat an underlying infection
Psoriasis
Psoriasis is a chronic autoimmune disorder that causes the overproduction of skin cells. Researchers don’t know the exact causes of psoriasis, but they believe it involves a combination of environmental and genetic factors.
These excess cells lead to patches of inflamed, itchy, and scaly skin and plaques: areas of raised, red, or discolored skin. People with psoriasis go through periods of flare-ups and remission (with no symptoms). While most cases affect the elbows, knees, and scalp, the rash can also affect the eyelids.
Treatment
Managing psoriasis often involves a combination of at-home methods and therapies, including:
Topical therapies, using creams, lotions, oils, or other products, especially those with vitamin D, retinoids (vitamin A), coal tar, and other additives
Keeping skin moisturized; taking daily, 10-minute lukewarm baths
Topical corticosteroids, phosphodiesterase 4 (PDE4) inhibitors, aryl hydrocarbon receptor (AhR) agonists
Oral medications that suppress immune function, including Rhuematrex (methotrexate), Gengraf (cyclosporine), or tyrosine kinase 2 (TYK2) inhibitors
Monoclonal antibody drugs, such as injections of Cimzia (certolizumab), among others
Phototherapy, exposing affected skin to UVB rays
Avoiding potential triggers, such as infections, injury, or cold temperatures
Periorbital and Orbital Cellulitis
Periorbital cellulitis occurs when the skin around the eye and eyelid becomes infected, and orbital cellulitis occurs when the infection spreads to the eye. The bacteria Staphylococcus aureus (staph) and Streptococcus (strep) are common causes.
These infections typically affect children and are caused by scratches or insect bites. Some cases of orbital cellulitis are also linked to sinus, ear, and gum or tooth infections.
The typical signs of periorbital cellulitis include redness, pain, and swelling in one eye. With periorbital cellulitis, eye movements don’t cause pain, and you see normally. But with orbital cellulitis, moving the eye hurts, vision becomes blurry or doubled, and the eye may bulge (proptosis). This condition can cause lasting damage to the eye if allowed to progress.
Treatment
Healthcare providers treat periorbital and orbital cellulitis with oral or intravenous (IV) antibiotics, which kill bacteria. Alongside antibiotics, topical corticosteroids may also help relieve symptoms.
You may need eye surgery if you have a severe case of orbital cellulitis that doesn't respond to other therapies.
Lupus
Lupus is an autoimmune disorder that affects the skin, joints, kidneys, brain, or other organs. It commonly is diagnosed in people assigned female at birth between the ages of 15 and 44. Researchers believe it derives from genetic, environmental, and hormonal factors and certain medications.
Nearly half of systemic lupus erythematosus (SLE)—the most common type of lupus—causes a distinctive, butterfly-shaped rash on the cheeks and over the nose, which can also impact the eyelids.
Treatment
As with some other autoimmune disorders, lupus has no singular cure. Healthcare providers recommend treatment to manage symptoms. For rashes associated with lupus and mild cases, options include topical corticosteroids.
When to Contact a Healthcare Provider
While rashes around the eyes are not typically serious, they can be. They can also significantly impact your quality of life. Medical treatments can make a big difference, so it’s important to know when to get help.
Call a healthcare provider if you experience the following:
Severe or worsening symptoms that don’t go away
Persistent symptoms, despite home remedies or over-the-counter medications
Signs of infection, including fever and swelling, tenderness, or warmth in the affected area
Symptoms that are disrupting your daily life
Summary
Many acute or chronic conditions can cause a rash around the eyes or on the eyelids. Treatments ranging from home remedies to medications or other procedures help manage flares or take on underlying causes.
A rash around the eyes can be a sign of something more serious, and symptoms can also significantly impact your self-image and quality of life. If you’re struggling with symptoms, it’s important to seek medical care. Don’t wait; the sooner you get help, the better you’ll feel.
Read the original article on Verywell Health.

