1 in 100 Tri-Citians test COVID positive in last two weeks. New pandemic record
The new case rate for COVID-19 in the Tri-Cities area has reached a record high for the pandemic, and four more people have died of complications of the disease.
The youngest was a Franklin County man in his 30s, said health officials.
The Benton Franklin Health District reported new record high case rates for both Benton and Franklin counties Thursday and again Friday as the highly contagious omicron variant of the coronavirus spreads.
And as a result, hospitals are delaying some non-urgent procedures to make sure beds and staff were available for patients who needed them most.
In Benton County, 1,142 new cases per 100,000 people were reported over two weeks as of Friday, and in Franklin County 1,306 new cases per 100,000 people were reported over two weeks.
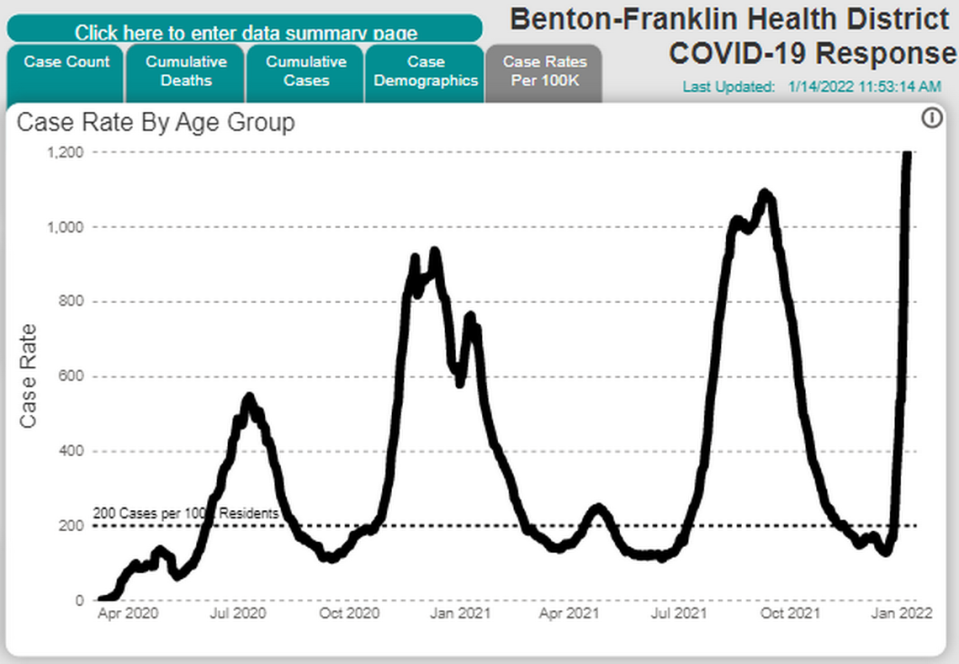
The combined case rate for the two counties is 1,195, or more than 1 in every 100 people with a positive COVID test result over the last two weeks.
The previous peak was about 1,185, as reported at the end of the summer as the delta variant of the virus surged.
The current new case rate may be an under count, said Dr. Amy Person, health officer for Benton and Franklin counties during a news briefing on Thursday.
More people are using rapid home test kits and many of their positive results may not be reported to public health officials.
The Benton Franklin Health District reported 952 new confirmed cases of COVID-19 on Friday, bringing the total for the week, starting with the weekend to 2,832.
That’s an average of 405 cases per day, up from 345 per day the previous week.
Tri-Cities COVID deaths
Four people died of COVID complications this week, according to the Tri-Cities based health district.
The youngest was a Franklin County man in his 30s. Also, a Benton County man in his 50s, Franklin County man in his 60s and Benton County woman in her 80s also died.
They bring Tri-Cities area COVID-19 deaths reported so far in January to five, with recent deaths reported once a week by the health district.
In December, 22 deaths of Benton and Franklin residents were announced. In November, 17 COVID deaths were reported, down from 80 reported in October.
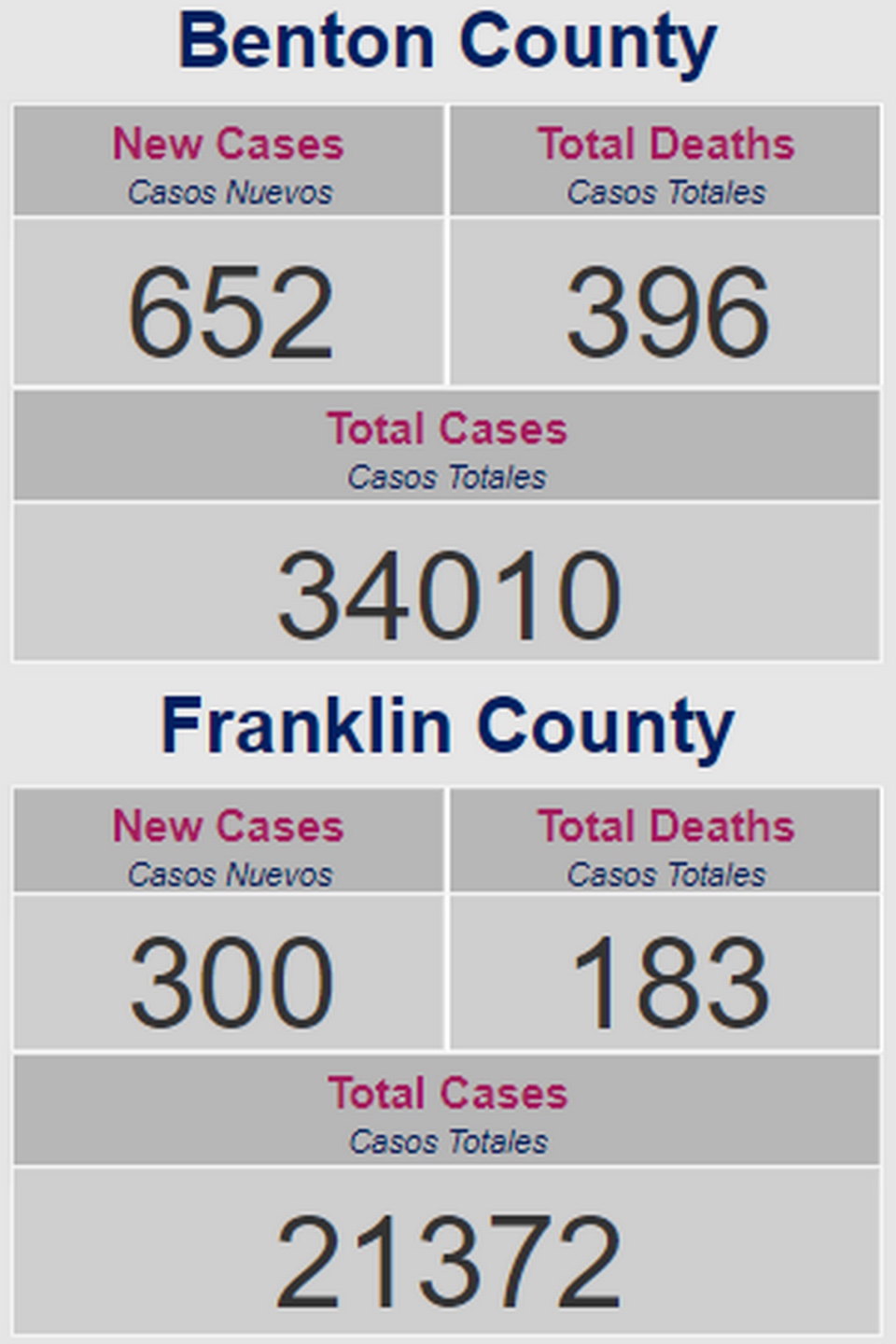
A total of 583 deaths of Tri-Cities area residents has been attributed to complications of COVID since the pandemic began, including 398 residents of Benton County and 185 residents of Franklin County.
Local public health officials verify that deaths are due to COVID complications by checking for a positive test result and that a coronavirus infection was named as a primary cause of death on the death certificate.
It can take several weeks for the district to receive and reconcile death information due to the reporting processes of medical facilities and coroner offices and the process of issuing and releasing death certificates.
COVID outbreaks
The Benton Franklin Health District reported five business outbreaks with 13 additional investigations in progress, in its last report issued early this week.
Schools had two outbreaks, although public health officials say that outbreaks are usually caused by after school activities and nonschool social activities, rather than through classroom spread.
Long-term care facilities, such as nursing homes had three outbreaks with 11 on watch, and investigations were being done in four healthcare facilities.
Tri-Cities hospitals
Reza Kaleel, the chief executive at Kadlec Regional Medical Center in Richland, said hospitals in the area appear to be dealing with the start of the surge of cases due to the omicron variant.
The omicron surge started earlier in Western Washington.
“We are buckling down for a pretty challenging few weeks, but with great hope that we will see this kind of move through and on to better days,” Kaleel said in a news briefing Thursday with the Washington State Hospital Association.
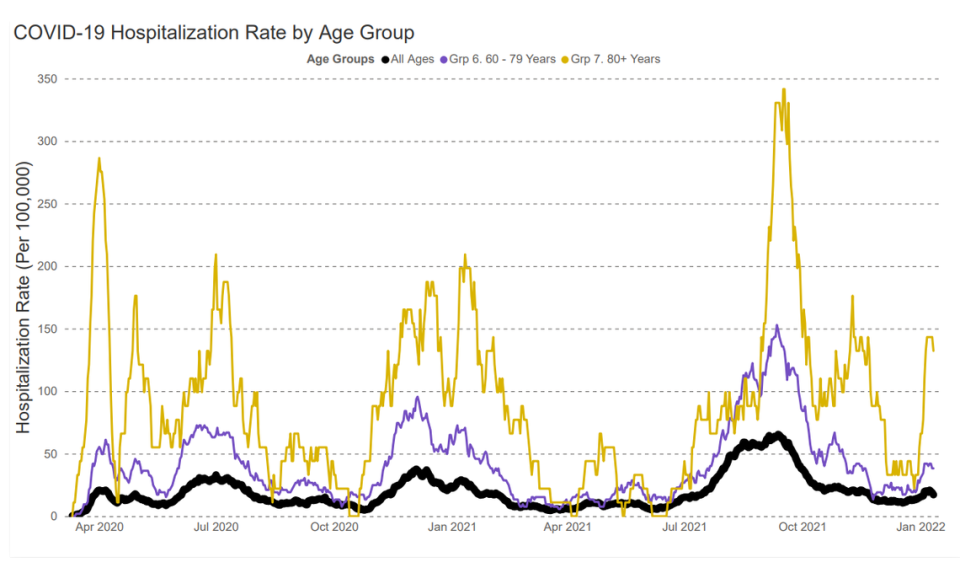
Although many cases due to the omicron variant are more mild than those due to the delta variant, some people — particularly those who are not vaccinated and the elderly — are still becoming ill enough to require hospitalization. In addition, some people may still be infected with the delta variant, which tends to cause more severe illness.
The Richland hospital, like others in the state, faces a greater challenge to have adequate staff working than in previous surges, as more staff are infected by the omicron variant in the community, he said.
The omicron variant is more contagious than both the original strain seen in the United States and also the delta variant that caused the previous spike in cases.
A total of 55 people were reported hospitalized in Benton and Franklin counties on Wednesday for treatment of COVID-19, with no reliable data available for later in the week.
The 55 patients were up from a recent low of 15 patients in mid December, but far below a high of 127 patients in mid September.
About 14% of the patients in the Richland, Kennewick, Pasco and Prosser hospitals Wednesday were there for treatment of COVID-19, according to the Benton Franklin Health District.
Additional patients were admitted for other treatment and also tested positive for COVID.
Statewide hospitals had a 65% increase in patients being treated for COVID over the past week compared to the previous week, with a 16% increase in patients needing ventilators.
A sizable majority of the hospitalized patients were not vaccinated against COVID or had only one shot, and very few had received a booster shot, said Taya Briley, executive vice president of the Washington State Hospital Association.
Hospitals delay care
As of Wednesday, Kadlec, the largest hospital in Benton and Franklin counties, was delaying some nonurgent procedures to make sure beds and staff were available for patients who needed them most.
Then on Thursday Washington Gov. Jay Inslee required hospitals in Washington state to halt nonurgent procedures and surgeries for four weeks to make sure there is enough staff and capacity for ill and injured patients.
Kadlec said in a statement after the announcement that the statewide order does not “apply to emergency treatment for life-threatening injuries or conditions such as strokes, heart attacks or anything else that warrants immediate care.”
The standard set in the state order requires delays in procedures if that is not anticipated to cause harm to patients within 90 days.
Potential harm could include expected advancement of disease, severe pain, deterioration of overall health or leaving a patient more vulnerable to COVID-19.

