3 doctors who received the Pfizer vaccine discuss their side effects and why they chose to get vaccinated
Last week, the Food and Drug Administration authorized emergency use of the two-dose Pfizer vaccine to battle the COVID-19 pandemic.
Frontline healthcare workers have been first in line to receive the vaccine, including three doctors who spoke with Business Insider about what it was like to receive the first dose.
Dr. Michael Bernstein from Connecticut said he had muscle soreness for about 24 hours after the shot, as did Dr. Katie Passaretti from North Carolina.
Here's what their experiences were like, as told to writer Nikhita Mahtani.
Just days after the Food and Drug Administration cleared the Pfizer-BioNTech COVID-19 vaccine for emergency use, Pfizer began shipping the vaccine to hospitals and healthcare centers across the US for distribution to frontline workers.
These three doctors were in the early rounds of vaccinations at their hospitals. Here's what they say the experience is like.
Dr. Michael Bernstein, 43, is an ICU doctor in Stamford, Connecticut.
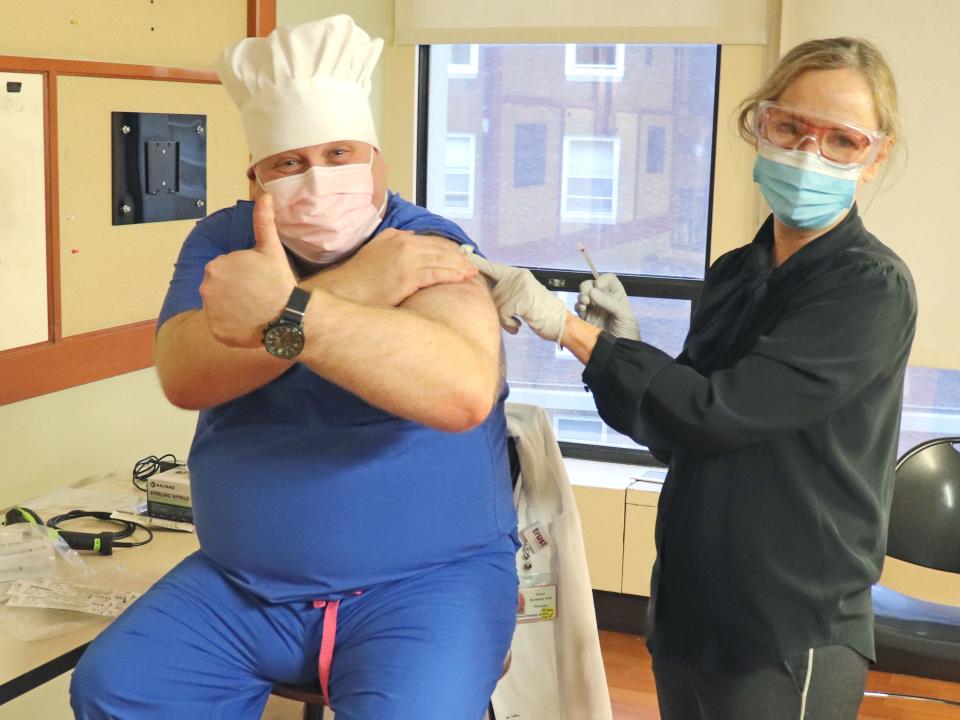
I received the Pfizer vaccine on December 16 at my hospital, Stamford Health. I think our hospital management wanted to first vaccinate some key clinicians who felt very comfortable with it - I personally wanted it as soon as possible since I see patients with COVID-19 every day.
Twelve hours before I received the vaccine, I took an information survey and signed the consent form.
At my appointment, I was asked to confirm that I was feeling OK, was given the injection, and then waited about 15 minutes to make sure I didn't experience any side effects.
I had a little muscle soreness, sort of like a punch to the arm, for about 24 hours.
Other than a little muscle soreness that felt similar to a punch, I felt perfectly fine. The hospital administrator said they'd be in touch to schedule the second dose, which will be within a 96-hour window about three weeks later.
I believe the science behind this type of vaccine - the messenger RNA platform - is strong. Understanding the basic science of it, I have very few concerns about the efficacy of the vaccine or the long-term complications. As a mechanism, there is no live COVID-19 virus in the vaccine: It's just giving you the code for spike protein so that your immune system will be able to make antibodies. To me, it's an even safer platform than many previous types of vaccines.
Many infectious diseases are managed through vaccines.
Infectious diseases that we don't think of as being a big issue anymore, like polio, even chickenpox, have been all but wiped out in the US thanks to vaccines that most people now get as babies.
One or two people are not going to stop the COVID-19 pandemic. It's really when we get a good majority of the population fully vaccinated that we'll start to see a major effect.
Until then, I plan to still wear my face mask, practice social distancing, and observe safety and sanitary precautions.
Dr. Nick Kessener, 35, is a fourth-year resident in internal medicine and pediatrics in Peoria, Illinois.

I deal with COVID-19 patients every day while working at OSF Medical Group both in the intensive-care unit and on the outpatient floor (where sick people come but aren't required to stay overnight). As one of the biggest hospital systems in central Illinois, we have significant COVID-19 numbers in our area, so many of our healthcare workers were scheduled to be vaccinated in the early rounds.
We were informed by the hospital administration in late November that we'd receive the vaccine shipments early and told basically to opt in or opt out. If you opt in, you can always opt out later saying, "Hey, I don't want it." It's not required, but it was certainly encouraged to get vaccinated.
My hospital prioritized the order based on who was working with COVID-19 patients for at least 50% of their patient-interaction time. I received it the morning of December 15, the first day we began doses.
For me, the choice to get vaccinated is a risk versus benefit decision.
I'm at fairly high risk of contracting the virus because I work around COVID-19 patients extensively. I've seen the effects of this disease, from short-term complications like respiratory distress to the long-term complications like pulmonary issues with pneumonia and even lung diseases. I had a patient in her 30s who had a stroke because of COVID-19, and it made me realize this is a scary disease, especially for causing young, healthy people to be having significant complications very early on.
Before I got the vaccine, I was given a form explaining the potential side effects, how it was emergency approved by the FDA, and what's in it, so I had all of the information and could opt out whenever.
After I got the shot, I had just a little muscle soreness.
Personally, it makes me feel better that I'm a lot more protected because I did feel like it's not a matter of if I get it, it's when. It's somewhat of a miracle that I somehow haven't caught it yet, so I am really reassured from that sense. But at the same time, I could still spread it if I'm around someone, since the data isn't out on whether it prevents spreading to other people yet, even if I don't get the disease myself.
I still plan to, of course, wear a mask and wash my hands well. I was happy to get it and am thankful that though it's still very early, it feels like the beginning of the end of the wild era that is COVID-19.
Dr. Katie Passaretti, 44, is an infectious-disease attending doctor in Charlotte, North Carolina.
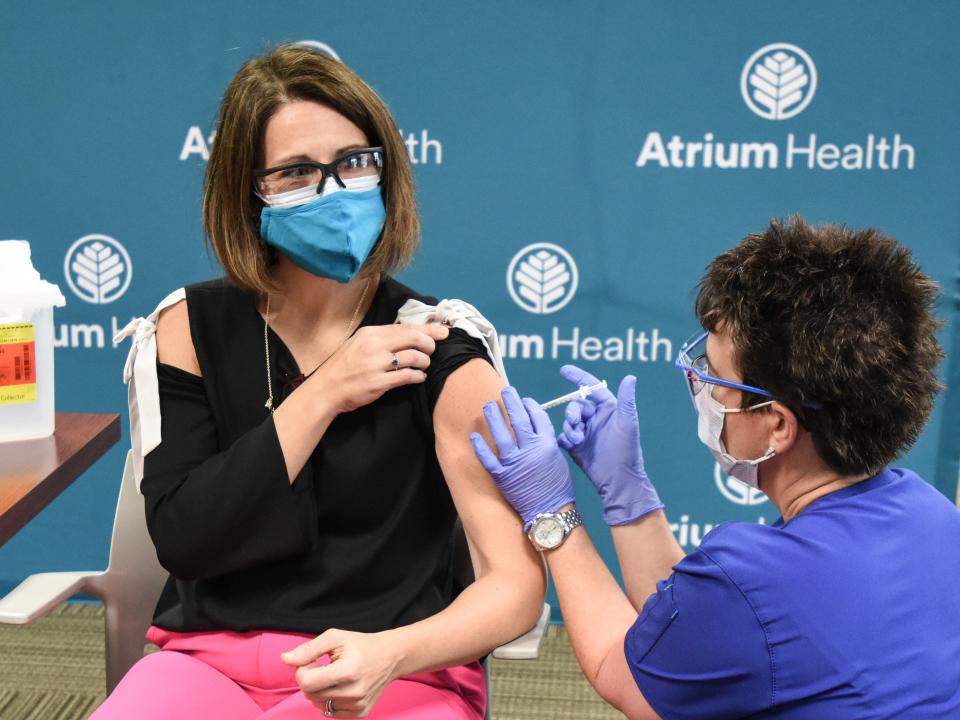
On December 14, I was the first person to get the COVID-19 vaccine in North Carolina, where I work as the infectious-disease attending MD at Atrium Health. I wear a couple of hats in my job - often I'm actively seeing and treating patients admitted to the hospitals with infectious-disease issues, so the risk of me getting the virus is quite high.
You don't go into infectious diseases without acknowledging that some infections can be spread from patients to you while you are trying to heal them, but I feel a responsibility to treat patients with COVID-19 the same as I do for other infectious diseases.
This year has been tremendously challenging seeing the vast number of people infected with COVID-19 and how the virus has affected patients, families, and healthcare workers.
I've watched entire families be devastated when COVID-19 spreads at a funeral. I've seen couples pass away together and healthcare workers hospitalized after contracting COVID-19 while trying to take care of patients. It's been exhausting and emotional to say the least. The vaccine to me is a ray of a hope at a time that's been clouded by darkness with rising cases and hospitalizations. It's a beacon of light just when we need it.
For that reason, I had no hesitation in getting the COVID-19 vaccine: I feel strongly that getting the vaccine affords us an opportunity to influence the very dangerous trajectory we are on. I've thoroughly reviewed the data on the Pfizer vaccine and believe it to be effective and safe.
To me, the vaccine is far less risky than continuing to let COVID-19 spread unchecked.
My side effects were minimal - muscle soreness for 24 hours, that's about it. I absolutely felt safe, well-informed, and in good hands getting the vaccine. It felt physically very similar to any other vaccine I've received in the past.
But my emotional reaction to receiving the vaccine, and more importantly watching my other healthcare workers get vaccinated, was very different and honestly moved me to tears. It felt like the right thing to do to protect my community, set an example for my peers, and do my part to protect others in my community and workplace. I am grateful for the scientific experts that worked so hard to make this vaccine possible as quickly and as safely as they have, and I look forward to encouraging others to get vaccinated with me.
I definitely feel safer, but I am still masking up, maintaining social distance, and staying home. I do believe getting vaccinated is an important part of protecting those around me, including my patients, but until the pandemic is more under control, I have no plans to change my behavior.
As an infectious-disease doctor, I wouldn't recommend anyone else change behavior quite yet either, especially before most of the country is vaccinated.
Read the original article on Business Insider

