After declining for months, U.S. coronavirus cases are rising again. Has the 'fall wave' begun?
Summer just ended. The weather is cooling. School is back in session — or trying to be. People are spending more time indoors.
And now, after nearly two months of slow but steady decline, new daily U.S. coronavirus cases are rising again, with the seven-day average increasing by 21 percent — from 34,588 to 41,868 — since Sept. 12.
Is this the start of the pandemic’s dreaded “fall wave”?
The short answer is… it’s complicated. Much of the current uptick in coronavirus cases is tied to geography. In some previously hard-hit places — California, for instance — it’s almost certainly a by-product of increased testing. In others, such as Texas, college outbreaks are a driving force. Meanwhile, a state like Wisconsin — where the average positive testing rate has soared from about 6 percent in early August to more than 17 percent today — seems to have a more widespread problem.
And so even though it’s too soon to say whether a fall wave has begun, it’s not too soon to see the recent rise in U.S. cases for what it is: a warning.
Regardless of whether President Trump thinks we’re “rounding the final turn” of the pandemic, the truth is, we’re barreling into the riskiest months of the year averaging more than 40,000 new cases per day (and possibly rising). That level of spread in turn sets the stage for precisely the sort of fall wave that experts are worried about — and that they’re already starting to see in foreign countries where the virus appeared to be, until recently, under far better control than it has ever been in the U.S.
“The concern I’ve had and continue to have [is] this baseline of cases that we have every day,” Dr. Anthony Fauci, the nation’s top infectious disease expert, told CNN earlier this week. “We’re looking straight at the fall coming upon us. We’re looking at the winter coming upon us. If we don’t get that baseline down sharply to a very low level … when you have a lot of cases floating around, it’s much more difficult to contain.”
Wisconsin might be the most worrisome state in America right now. Last week, it cleared 2,000 daily cases for the first time — then hovered above that mark for three straight days. Health officials are currently detecting a “high level” of coronavirus activity in 71 of the state’s 72 counties. And while much of that spread appears to have originated with returning college students — the University of Wisconsin system has campuses in six of the eight cities with the fastest rise in cases — it has since blanketed the state.
According to a report Wednesday from Wisconsin Public Radio, K-12 school districts statewide have been forced to revert to remote learning amid growing community outbreaks. Wisconsin’s COVID-19 hospitalizations hit an all-time high on Tuesday, rising nearly 40 percent over the last week to surpass the previous record set on April 9. In response, Gov. Tony Evers just declared a new public health emergency.

“We continue to learn more about this virus, but what we do know is that we are facing a new and dangerous phase of the COVID-19 pandemic here in Wisconsin,” Evers said. “We are seeing an alarming increase in cases across our state.”
Wisconsin’s worsening situation reflects a broader trend across the Midwest, which, unlike the Northeast, South and West, never experienced much of a peak — but which now, belatedly, is setting new daily records with more cases per capita than any other region. Over the last week, the 11 states with the most cases per capita were, in order, North Dakota, South Dakota, Wisconsin, Oklahoma, Iowa, Utah, Arkansas, Missouri, Texas, Nebraska and Kansas.
But surges in states that haven’t suffered yet are one thing. A resurgence in a state that was already pummeled by the pandemic is what would, in theory, distinguish the tail end of the first wave from the start of the second — which is why Texas’s inclusion on that list is troublesome.
As the New York Times recently reported, “inconsistencies and problems with COVID-19 data collection in Texas have clouded the picture of the pandemic’s trajectory in the state.” In fact, Texas suddenly reported 22,276 cases on Tuesday — 7,000 more than it had ever reported before. The vast majority of them weren’t new; instead, they were backlogged or overlooked infections from some previous date.
Yet the Times database, which adjusts for such anomalies, still shows the average number of new daily cases in Texas rising 16 percent over the last two weeks. The South as a whole is still registering nearly as many new cases per capita as the surging Midwest — another disturbing sign.
To be sure, Texas’s current seven-day average (about 4,200 cases) is less than half its July peak (about 10,400). But it’s still moving in the wrong direction. As in Wisconsin, much of the spread seems to be starting on college campuses. According to the Texas Tribune, cases have grown 34 percent since Aug. 19 in counties where four-year college students make up at least one-tenth of the population; that’s compared with 23 percent in counties with a smaller proportion of students.
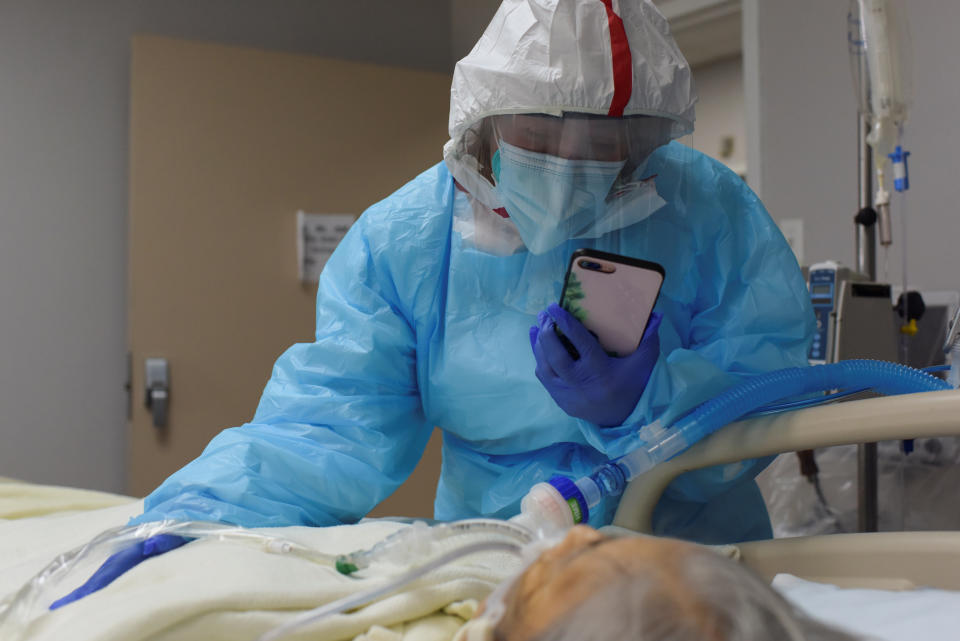
The problem, as Harvard infectious-disease researcher Stephen Kissler told the Texas Tribune, is that “diseases don’t stay isolated in the populations where they start.”
That trend is already clear in Lubbock, which houses Texas Tech and other colleges. Local health authority Dr. Ron Cook told the Texas Tribune that a “mild uptick” in rates of hospitalizations and intensive care unit admissions there has accompanied rapid growth in cases since students returned to campus.
If that pattern replicates itself statewide, it will test whether the virus infected much of Texas’s vulnerable population during the first wave or whether there’s still enough susceptibility left for an even bigger second wave — a frightening possibility with fall and winter ahead.
For now, California seems to be in better shape than either Texas or Wisconsin. As recently as Aug. 15, the state was averaging 9,400 new cases per day; now it’s averaging 3,600. Even a slight recent rise in new daily cases — the seven-day average appears to have bottomed out at 3,300 on Sept. 13 before inching upward again — may be misleading. Over the same period of time, the average number of daily tests conducted increased from 92,000 to more than 125,000, and the state’s positive testing rate actually fell from 3.54 percent to 2.79 percent, a new low. In other words, increased testing more than accounts for California’s recent rise in cases.
Yet California could also be the state to watch to see how complacency factors into the fall equation. With the positivity rate now below 3 percent for the first time and hospitalizations down to their lowest level since April, California’s reopening took a significant leap forward on Tuesday as officials granted five more counties — Riverside, San Luis Obispo, San Mateo, Alameda and Solano — the freedom to resume indoor dining, moviegoing and other activities. Even nail salons were given the go-ahead to reopen statewide, pending county approval. In-person schooling could resume within weeks.

The state’s four-tier reopening plan is relatively conservative, with benchmarks for the percentage of positive tests and new cases per capita that each of its 58 counties must meet for two consecutive weeks before advancing.
But Europe offers a sobering preview of what might lie ahead for states such as California if they simply assume the worst is behind them. After lockdowns this spring helped to smother the pandemic there — positive testing rates were lower than 2 percent — the virus once again is tearing across the continent as people proceed with their lives. Driven by soaring case counts in France, Spain and the U.K., Europe as a whole is now averaging 52,000 cases per day — nearly 20,000 more than it was detecting during its spring peak.
At the same time, Israel, which has seen its average daily case count more than double since the start of September, imposed a second countrywide lockdown last week — which it furthered tightened Thursday, ordering all nonessential businesses to close and requiring residents to stay within 1,000 meters of their homes.
None of this is to say that America’s fall wave is already underway. For now, new infections are skewing young. Deaths are trending downward. Therapeutics are improving. The U.S. can still avoid the worst if it collectively continues to take the kind of precautions that eventually stalled California’s summer spike — masking up, staying distant, avoiding indoor gatherings.
Or not. The U.S. is unlikely to have enough vaccine doses for every American until next spring, according to Fauci. The most perilous months of the pandemic fall between now and then. It’s largely up to us what happens next.
_____
Read more from Yahoo News:




