Answers to your 24 most pressing questions about the coronavirus vaccine, from side effects and costs to when you'll be able to get one
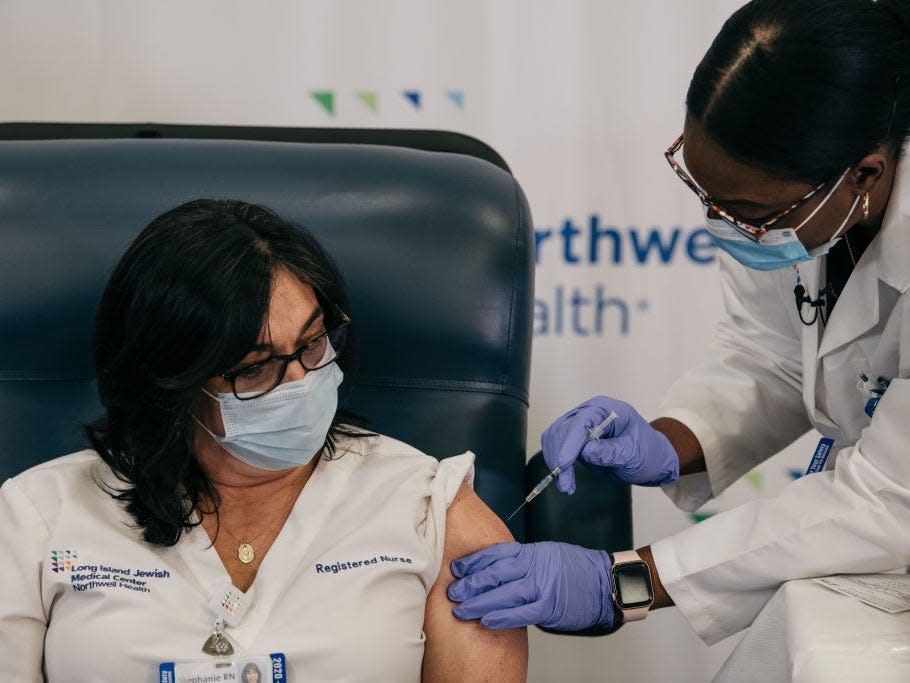
Coronavirus vaccines are the main chance the US has to dig itself out of the pandemic, and 10.6 million people have gotten their first shots so far.
People are desperate to get vaccinated so they can protect themselves, see loved ones, and return to normal.
The rollout so far has been slow and messier than planned, but US health officials say they're hitting the gas pedal in the weeks ahead.
Here's what you need to know about the vaccine, from timeline to cost and side effects.
Have a burning question you don't see here? Email reporter Kimberly Leonard at KLeonard@insider.com.
Coronavirus vaccines are finally out the door and going into people's arms.
It's the best shot the US has to dig itself out of a vicious pandemic that has killed more than 389,000 people and otherwise shows no signs of slowing. So far, the rollout has been slow and messy.
But now that the vaccine is here, you're probably wondering what it means for your loved ones and for you.
You might be desperate to get the vaccine as soon as you can so that you can protect yourself, knowing that you'd otherwise face serious illness from COVID-19, the disease caused by the coronavirus. Maybe you want to make sure your grandparents get it before you do.
Perhaps you're not ready to get the vaccine just yet. Or you got your shot and are now wondering what to do next. Maybe you're concerned about its side effects.
To help, we've answered some of the biggest questions everyone has about the coronavirus vaccine.
The sooner hundreds of millions of people get the vaccine, the sooner the country can overcome the pandemic. At least 75% of people in the US will need to get vaccinated to achieve herd immunity, according to Dr. Anthony Fauci, the federal government's top infectious diseases expert.
Don't see a burning question answered? Send it over to KLeonard@Insider.com.
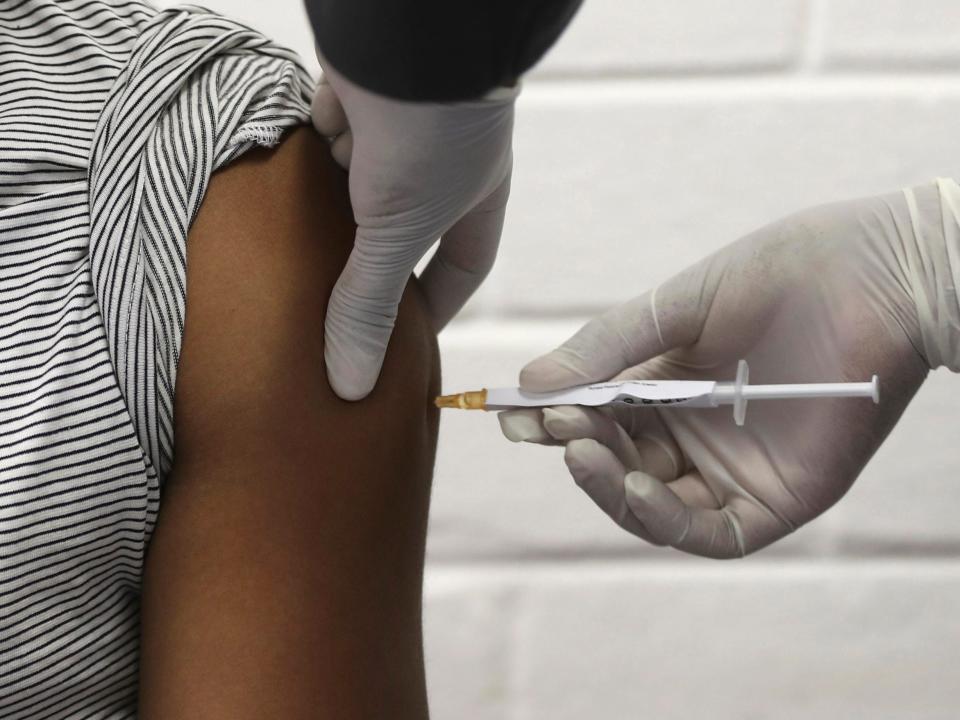
What's the best time to get a shot?
You should get a coronavirus vaccine as soon as your turn comes if you want it.
The Centers for Disease Control and Prevention recommends the first doses go to frontline healthcare workers and nursing home residents. But states are free to determine how they want to distribute the doses and the vast majority of them are following CDC guidelines.
A few are doing things differently. Florida, for instance, decided early-on on a broader prioritization group of anyone 65 years and older.
After frontline healthcare workers and nursing homes have been offered their initial doses, a CDC expert group recommended that people above 74, and certain essential workers - such as teachers, emergency responders, and grocery store employees - should be next in line. On January 12, the Trump administration also encouraged states to open up vaccines to people 65 and older and to people with chronic conditions.
The best place to start is to check your state and community's COVID-19 websites.
How will I know when it's my 'turn'?
It all depends on your job, age, health status, and your location. Every state and even city does things a little differently. Keep an eye on announcements in your local newspaper, and see what information your doctor has. Talk to your friends, community and faith leaders. Tune in to news conferences from your local health department.
Also check your local pharmacy. Major pharmacy and big-box retailers - including Walmart and Costco - are getting ready to help speed the vaccine rollout in the coming weeks and months.
If you're a healthy, young adult then you're likely to be last in line in most states. That changes, though, if you have an "essential" job, including working at a grocery store or in a meatpacking plant. If that's the case, you'll probably have access sooner because you're at higher risk of getting infected.
Once the vaccine becomes more widely available you'll be able to see where you can get one on the Vaccine Finder website.
How can I jump the line?
You may have read stories about how some people who aren't in high-priority groups have still managed to score a vaccine. What's happening is that some pharmacies and hospitals are finding themselves with already thawed leftover shots at the end of the day after they vaccinate people who are eligible for shots.
In some places, healthcare facilities are giving out those remaining shots to anyone who'll take them, whether it's the nearest shopper in the store or an employee who'd otherwise have to wait longer. Those precious vaccines would otherwise go in the trash.
A lot of places have policies saying that any extra vaccines should first go to other workers in the building, such as pharmacists, hospital, and grocery store staff, before being doled out to whoever happens to be nearby and is willing to get inoculated.
If you go the route of trying to find a leftover shot, you may have to wait in line for a long time. The lines may be indoors, and so you'll have to consider the risks of exposing yourself to the coronavirus while you wait with other people.
This isn't a surefire way to get a vaccine. Some people have waited in line for hours and still ended up going home empty-handed.
Read more about how Insider reporter Kimberly Leonard tried her luck at landing a leftover vaccine.
Can I just call a hospital and see if they'll take me?
Hospitals are focused on vaccinating their staff, but sometimes they do open up vaccines to more people. Keep your eyes peeled for announcements from your local hospital, but also bear in mind that there's a nationwide surge in coronavirus cases, and nurses and doctors are overwhelmed.
Nancy Foster, vice president of quality and patient safety policy at the American Hospital Association, recommended people check each of their state's COVID-19 websites to see when they can get a shot.
"At this point, we do not recommend that people call hospitals to try to schedule a vaccination," she said. "Hospital staff are incredibly busy trying to care for a large number of hospitalized patients."
Which shot should I get?
The short answer is - you should get the shot that's offered to you. There probably won't be much of a choice, as supply is very limited. Both Pfizer and Moderna's vaccines are highly effective in preventing COVID-19 infections.

Should I talk to my doctor first?
You're not required to talk to a doctor before getting vaccinated. But consider talking to your doctor about it if you have any questions or a major pre-existing condition.
Your doctor may recommend waiting to get a vaccine until more data becomes available, or may be able to provide tips about where you can get your shot. Be aware that some doctors charge for these kinds of consultations.
What if I'm healthy?
Great news! These vaccines are for you.
Vaccinations are designed to protect healthy people from future infections, not to treat diseases we already have. That's why safety regulations for approved vaccines in the US are so stringent. Moderna and Pfizer have both been granted a special FDA emergency use authorization for the pandemic, which is a bit less rigorous than the normal approval, but still tough. If you're healthy, go ahead and get a shot.
What if I already had COVID-19?
You can get a vaccine if you already had COVID-19, but if you're still sick, it's best to wait until you've recovered. The CDC recommends waiting 90 days, since it's highly unlikely you'll get reinfected again within the first three months post-infection.
It's possible you may have developed some level of immunity from your infection, but that immunity could be incomplete, or it could wane over time. For the surest level of protection against all circulating variants of the virus, it's best to supplement any potential natural immunity you might've built up through infection with a vaccine.
Moderna and Pfizer's vaccine trials didn't include very many people who'd had prior COVID-19 infections, but the data so far suggests that these vaccines have been safely administered to hundreds of people with previous COVID-19 infections, and the vaccines seem to protect them well from additional infections, particularly the severe kind. (Remember: reinfection is rare, but possible).
Immunologist James Hildreth recently suggested at an FDA meeting on COVID-19 vaccines that people who've had the virus could just get one shot, instead of two - with their infection serving the place of the initial, or "primer" dose, and the single shot as a "booster" - but that shot-saving strategy hasn't been tested out yet in people, so it's impossible to know if it would work.
Do I really need to go back for a second shot?
Technically, no. No one is going to force you to get a second shot.
But it's a good idea. Both Pfizer and Moderna's shots have been designed to work best in two doses, administered several weeks apart. Vaccine-takers get some degree of protection from their first shot - but it's only full-strength after the second one. And it's unclear how long that first shot protection would last, without the booster.
How will I know when it's time to go back for that second shot?
The CDC is giving everyone vaccination cards to keep track of when they get each shot. For Pfizer's vaccine, the recommendation is to get the second shot 21 days after the first, while for Moderna, it's 28. But, if you're a few days late, worry not: go ahead and get that second shot. In the trials, not everyone was perfectly on time for their second dose either, and a few days of lag time shouldn't be an issue.
What if I lose my vaccine card?
When you get your vaccine card, take a picture of it, so you remember the date you got your first shot. That way, you can still keep track of when it's time to get the second jab, even if you lose the little white card.

Can I throw my mask away after I get the vaccine?
Unfortunately, scientists don't yet know whether the vaccines protect people from carrying the virus and passing it on to others. That information is coming.
For now, you'll still need to wear a mask and keep physical distance from those outside your household.
Once more and more people are vaccinated, the guidelines about mask-wearing and social distancing will change.
How long will it take for me to become immune to COVID-19 after I get the vaccine?
In vaccine studies of tens of thousands of volunteers around the world, most people started to gain the benefit of some protection from infections after their first shot. This protection usually began to kick in at about the two-week mark after shot number one.
But, it's still important for people who've received one shot to keep wearing a mask in public, and adhering to social distancing, because the protection is not complete, and you could still easily get infected with just one shot on board; indeed, many people already have.
It's only after the second dose of the vaccine that your risk of infection can plummet to as little as 5%. Scientists measured that efficacy level beginning one week (for Pfizer) or two weeks (for Moderna) after the second shot. That's when you can expect the vaccine to have fully kicked in. It's still not known whether you could be an asymptomatic carrier after vaccination is complete, so it'll still be important to wear a mask to protect others after that.
I have severe allergies, should I skip the vaccine?
The odds that you will have a reaction to these vaccines, even if you have some severe allergies, are incredibly slim.
As of January 6, the CDC had counted up just 29 reports of people having allergic, anaphylactic reactions after vaccination, among nearly 5 million people who had received the shots. If you have a history of severe allergies, talk to your provider before you get your shot, make sure they have epinephrine on hand just in case, and wait on-site for 30 minutes after your vaccination to make sure a reaction isn't at hand.
The only adults the CDC is recommending should not get vaccinated are those who've had an allergic reaction after a previous dose of a COVID-19 vaccine.
How will I know if I get an allergic reaction? What should I do if I get one?
Reports of allergic reactions to coronavirus vaccines have been rare, but a few people in both the US and the UK have had non-life-threatening anaphylactic reactions in the moments after their vaccination. Tell-tale symptoms have included rashes, swollen lips and/or tongue, hoarseness, wheezing, and, in a couple of the most severe cases, trouble breathing or swallowing.
The CDC has recommended healthcare providers administering shots have EpiPens on hand just in case of an allergic reaction.
Will I get tested for preexisting conditions before getting the shot?
The healthcare provider who gives you a vaccine will ask you to fill out a form about your health status. It's likely to ask about allergies, your history with vaccination, your pregnancy status, and your medication regimen.
You'll have the opportunity to ask questions of the healthcare worker who gives you the vaccine before you take it.
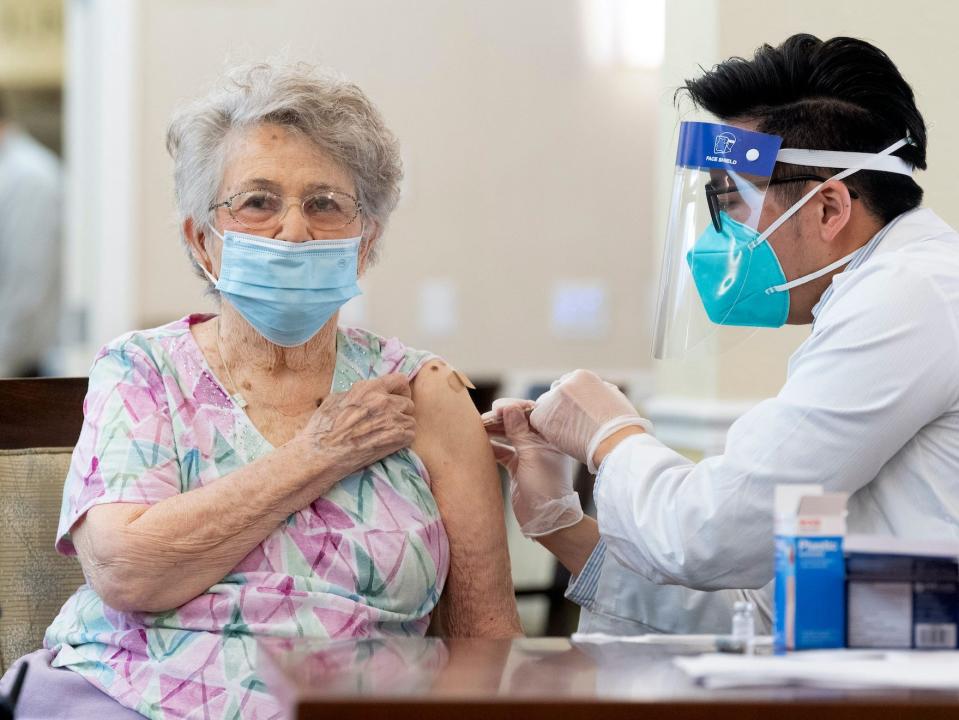
Will it hurt?
As much as any other needle-in-the-arm vaccine hurts, yes.
But many people who've had it say it's not an unusually painful jab. If you've ever had a flu shot, you likely already know what the moment it hits your arm muscle will feel like.
There are some side effects to prepare for after you go home: most people report some pain at the injection site, fatigue, and headaches, typically lasting a few days after vaccination. For some, the arm pain and drowsiness in those hours and days after vaccination can be somewhat severe.
How can I report any side effects?
After you get your vaccine, the CDC will send you a survey called V-Safe to fill out over text message that'll ask you whether you're having any symptoms. You'll be able to opt out if you choose, but opting in will help public health experts track any side effects they didn't know about before.
You'll get the survey every day for a week. If you report a serious illness, someone from the federal government will follow up with you to get more information.
You can also report any side effects from the shot with the federal government's Vaccine Adverse Events Reporting System.
What if I'm pregnant or breastfeeding?
Scientists haven't evaluated the safety or effectiveness of coronavirus vaccines during pregnancy.
This is common. Few drugs and vaccines are tested during pregnancy for ethical reasons, including concerns about harming a developing fetus.
The American College of Obstetricians and Gynecologists says that people can have conversations with their doctors about getting the coronavirus vaccine while pregnant or breastfeeding. The group also says these discussions shouldn't be required if a patient is comfortable going ahead and getting vaccinated.
It's important to keep in mind that people who get infected with the coronavirus while pregnant face an increased risk of death and severe illness, including the risk of giving birth prematurely, according to the CDC.
The World Health Organization has issued its first COVID-19 vaccine recommendations for pregnant women who are considering receiving Pfizer's shot. More guidance is expected soon for Moderna's. In its guidance about the Pfizer vaccine, the agency said there's still not enough data to know for sure what the risks and benefits might be of getting vaccinated during pregnancy. For now, the WHO recommends pregnant women who work in high-risk settings such as healthcare and frontline workers, and those with pre-existing conditions get these vaccines.
Is there anyone who shouldn't get the vaccine?
For now, children don't qualify. Pfizer's vaccine is only approved for people above the age of 16. Moderna's is for those 18 and above.
The CDC is also discouraging people from getting the second dose of the vaccine if they had a bad reaction to their first shot.
People who are currently infected with the coronavirus should also wait until their illness has passed before they get the vaccine.
How is the vaccination campaign going across the US?
Nearly 10.6 million people in the US have received their first dose as of early January, according to the CDC. The federal government's vaccine initiative, called Operation Warp Speed, has taken charge of securing the supply of doses and shipping them to states. Beyond that, states are in the driver's seat when it comes to putting shots into arms.
Warp Speed has distributed more than 31 million doses to date, but only about one-third of those have been used so far, according to CDC data. Warp Speed has faced criticism for overpromising and underdelivering, falling way short of reaching its goal of starting 20 million vaccinations by the end of 2020.

Can my employer force me to get a vaccine?
Yes, and some workplaces will mandate coronavirus vaccines.
States will have different rules, and there may be exemptions for religious or medical reasons.
Where Fauci works at the National Institutes of Health, annual flu vaccines are already required for anyone who works directly with patients. That's common for lots of healthcare facilities.
Fauci said he expects COVID-19 vaccines to follow suit.
"I have to get certified every year," he recently told Newsweek. "If I didn't, I couldn't see patients. So in that regard, I would not be surprised, as we get into the full scope of [COVID-19] vaccination, that some companies, some hospitals, some organizations might require [COVID-19] vaccination."
Already, at least one major nursing home chain is.
How much will the vaccines cost? Does my insurance pay for it?
President Donald Trump signed a bill into law last year that aimed at ensuring that patients don't get charged for coronavirus vaccines. Insurance companies are supposed to pick up the full tab, and doctors, pharmacies, and hospitals aren't expected to bill patients for the shot.
The vast majority of people probably won't have to pay anything, but some costs - even small fees- might end up slipping through the cracks. After all, coronavirus testing and care were also supposed to be covered without charging patients. But as Insider reported last year, many people faced charges anyway.
Be sure to ask whether there will be any fees associated with your vaccine visit. If you get a charge, call your insurance company and healthcare provider to ask about what's going on, and point out that you're supposed to get free vaccines under federal law.
There may just be a mix up or something that may have gone wrong in the process of billing for the vaccine. Sometimes doctors charge when you ask questions about another health ailment during the visit, or if you have other tests done while you're there.
What if I'm uninsured?
You qualify for a free shot. Healthcare providers are supposed to bill the federal government for all vaccines they administer to patients who don't have health insurance.
Did you get charged for a coronavirus vaccine? Tell us about it by emailing KLeonard@insider.com.
Read the original article on Business Insider
