Brain cancer in children is notoriously hard to treat – a new mRNA cancer vaccine triggers an attack from within
Brain cancers remain among the most challenging tumors to treat. They often don’t respond to traditional treatments because many chemotherapies are unable to penetrate the protective barrier around the brain. Other treatments like radiation and surgery can leave patients with lifelong debilitating side effects.
As a result, brain cancer is the leading cause of cancer-related death in children. Brain tumors in children frequently do not respond to treatments developed for adults, likely due to the fact that pediatric brain cancers are not as well-studied as adult brain cancers. There is an urgent need to develop new treatments specific to children.
We developed a new messenger-RNA, or mRNA, cancer vaccine, described in newly published research, that can deliver treatments more effectively in children who have brain cancer and teach their immune systems to fight back.
How do cancer vaccines work?
The immune system is a complex network of cells, tissues and organs whose primary function is to continuously surveil the body for threats posed by foreign invaders – pathogens that damage tissues and make you sick. It accomplishes this by recognizing antigens, or abnormal proteins or molecules, on pathogens. T cells that recognize these antigens seek out and destroy the pathogens.
Your immune system also protects you from domestic threats like cancer. Over time, your cells sustain DNA damage from either internal or external stressors, leading to mutations. The proteins and molecules produced from mutated DNA look quite different from the ones cells typically produce, so your immune system can recognize them as antigens. Cancer develops when cells accumulate mutations that enable them to continue to grow and divide while simultaneously going undetected by the immune system.
In 1991, scientists identified the first tumor antigen, helping lay the framework for modern-day immunotherapy. Since then, researchers have identified many new tumor antigens, facilitating the development of cancer vaccines. Broadly, cancer vaccines deliver tumor antigens into the body to teach the immune system to recognize and attack cancer cells that display those antigens. Although all cancer vaccines conceptually work very similarly, they each significantly vary in the way they are developed and the number and combination of antigens they carry.
One of the biggest differences among cancer vaccines is how they are created. Some vaccines use protein fragments, or peptides, of tumor antigens that are directly given to patients. Other vaccines use viruses reengineered to express cancer antigens. Even more complex are vaccines where a patient’s own immune cells are collected and trained to recognize cancer antigens in a laboratory before being delivered back to the patient.
Currently, there is a lot of excitement and focus among researchers on developing mRNA-based cancer vaccines. Whereas DNA is the blueprint of which proteins to make, mRNA is a copy of the blueprint that tells cells how to build these proteins. Thus, researchers can use mRNA to create blueprint copies of potential antigens.
mRNA cancer vaccines
The COVID-19 pandemic brought significant attention to the potential of using mRNA-based vaccines to stimulate the immune system and provide protection against the antigens they encode for. But researchers have been investigating the use of mRNA vaccines for treating various cancers since before the pandemic.
Our team of scientists in the Brain Tumor Immunotherapy Program at University of Florida has spent the past 10 years developing and optimizing mRNA vaccines to treat brain cancer.
Cancer vaccines have faced significant challenges. One key hurdle is that these vaccines may not always trigger a strong enough immune response to eradicate the cancer completely. Moreover, tumors are not made up of one type of cancer cell, but rather a complex mix of cancer cells that each harbors its own unique cocktail of mutations.
Our cancer vaccine seeks to address these issues in a number of ways.
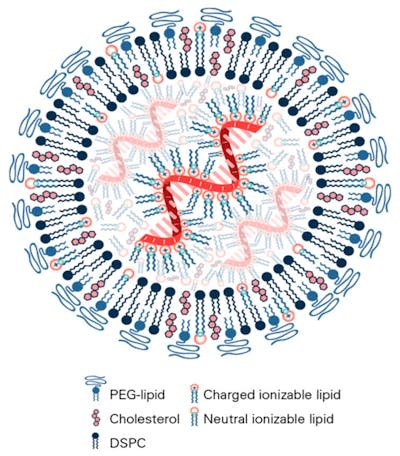
First, we designed our vaccines by using the RNA of a patients’ own cancer cells as a template for the mRNA inside our nanoparticles. We also packaged our cancer vaccine inside of nanoparticles made up of specialized lipids, or fat molecules. We maximized the amount of mRNA packaged within each nanoparticle by sandwiching them between lipid layers like the layers of an onion. In this way, we increase the likelihood that the mRNA molecules in our nanoparticles produce enough tumor antigens from that patient’s cancer to activate an immune response.
Also, instead of injecting nanoparticles into the skin, muscle or directly into the tumor, as is commonly done for many therapeutic cancer vaccines, our mRNA nanoparticles are injected into the bloodstream. From there, they travel to organs throughout the body involved in the immune response to teach the body to fight against the cancer. By doing so, we’ve found that the immune system launches a near immediate and powerful response. Within six hours of receiving the vaccine, there is a significant increase in the amount of blood markers connected to immune activation.
Looking to the future
Our mRNA-based vaccines are currently undergoing early-phase clinical trials to treat real patients with brain cancer.
We administered our mRNA-based vaccine to four adult patients with glioblastoma who had relapsed after previous treatment. All patients survived several months longer than the expected average survival at this advanced stage of illness. We expect to treat children with a type of brain tumor called pediatric high-grade glioma by the end of the year.
Importantly, mRNA vaccines can be developed to treat any kind of cancer, including childhood brain tumors. Our Pediatric Cancer Immunotherapy Initiative focuses on developing new immune-based therapies for children afflicted with cancer. After developing an mRNA vaccine for glioma in chidren, we will expand to treat other kinds of pediatric brain cancers like medulloblastoma and potentially treat other kinds of cancers like skin cancer and bone cancer.
We are hopeful that mRNA-based vaccines may lead to more children being cured of their brain tumors.
This article is republished from The Conversation, a nonprofit, independent news organization bringing you facts and trustworthy analysis to help you make sense of our complex world. It was written by: Christina von Roemeling, University of Florida and John Ligon, University of Florida
Read more:
John Ligon receives funding from the V Foundation, MIB Agents, the National Pediatric Cancer Foundation, Hyundai Hope on Wheels, the Pediatric Cancer Research Foundation, the Children's Miracle Network, the ChadTough Defeat DIPG Foundation, the Children's Cancer Research Fund, the DIPG/DMG Research Funding Alliance, the National Cancer Institute, and the Florida Department of Health Live Like Bella Pediatric Cancer Research Initiative.
Christina von Roemeling does not work for, consult, own shares in or receive funding from any company or organization that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.

