Britain’s terrifying isolation tent for the world’s deadliest diseases
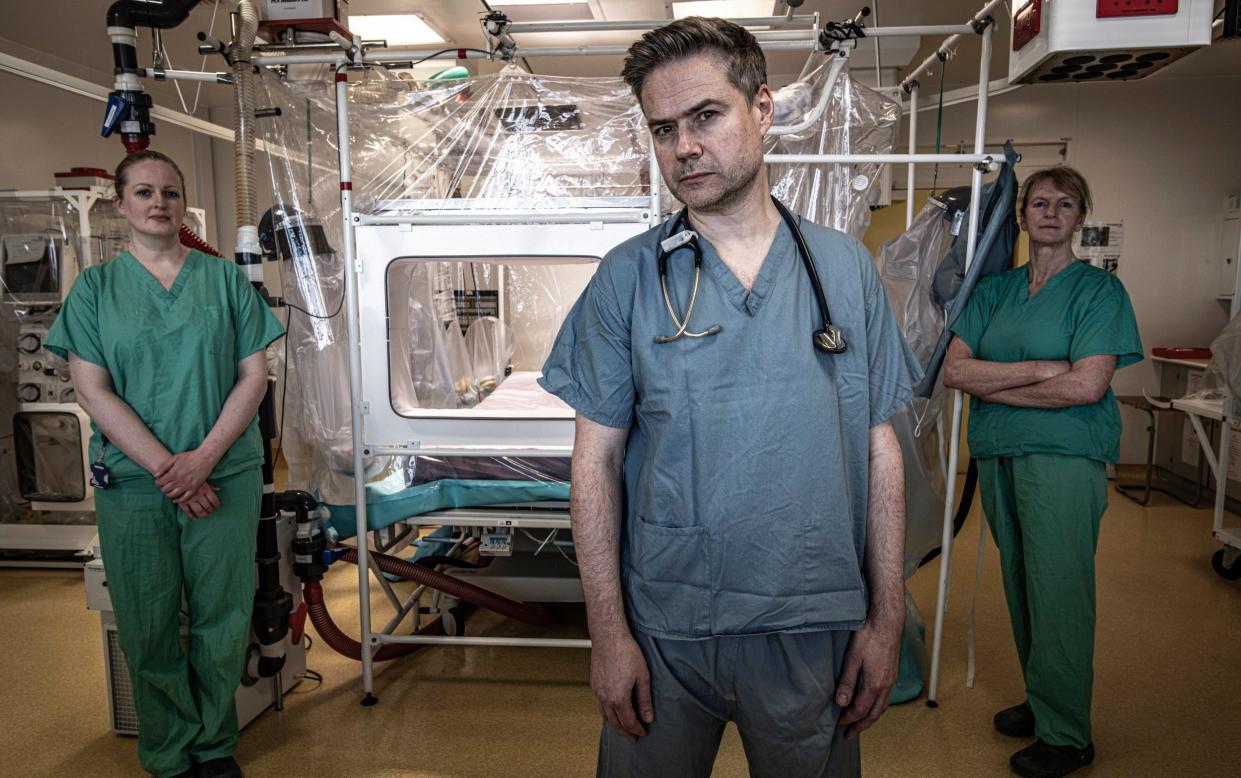
On the 11th floor of the Royal Free Hospital in London, a stone’s throw from the genteel hubbub of Hampstead Heath, a single bed stands shrouded and empty in an unlit room.
It’s an unsettling sight. The bed is forensically sealed inside a large plastic tent and rests solus in the centre of the room. From its frame, high-tech tubes and wires hang coiled. And in the walls of the transparent structure are five corporeal gloves, each large enough to envelope the arms and head of a nurse or doctor.
It’s here, in one of only two high-level isolation facilities in the UK, that patients sickened with the world’s most dangerous infectious diseases are brought for treatment. Whether it be Ebola or Marburg, Lassa or even Crimean-Congo hemorrhagic fever, care can be provided while the patient and pathogen remain entirely contained to prevent a wider outbreak.
The UK can go years without reporting any such infections, officially known as viral hemorrhagic fevers (VHFs) but this could be starting to change as immigration and travel to Britain become ever more global.
In February last year, three cases of Lassa fever were reported in England. The cases were within the same family and linked to travel to West Africa. One of the patients, a newborn baby, tragically died but both adults survived.

A month later, a case of Crimean-Congo haemorrhagic fever was identified, with the patient transported to the Royal Free’s isolation facility. Security staff manned the doors to the ward, as ordered by the Home Office, while a total of 158 rostered medics cared for the patient, who spent several weeks confined in the isolation facility.
“We only had about a week or two of downtime between this case and the cluster of Lassa fever cases we'd dealt with before that,” says Dr Jake Dunning, the lead consultant for high consequence infectious diseases at the Royal Free. “We just replaced the tent with a new one, and then we had to activate again.”
‘We’re seeing a genuine increase’
These emergencies came hot on the heels of the Covid pandemic, which, depending on estimates, has so far caused between 14 million and nearly 20 million excess deaths globally. Experts fear the frequency of these events is only going to increase in the decades ahead.
“I think we’re seeing a genuine increase in some of these diseases,” says Dr Dunning, who argues that climate change, globalisation and deforestation is bringing humanity and nature into ever-closer proximity with one another, increasing the risk of zoonotic outbreaks.
“Things like Crimean Congo hemorrhagic fever, which is tick-borne, you can find in Europe”, adds Dr Dunning. “I think we will see more cases of that in people who go hiking in Spanish mountains, for example.”
Last year, scientists identified ticks positive for the infection across Spain, indicating it is “widespread” in the country.
Then there are the ongoing, and simultaneous, outbreaks of Marburg in Tanzania and Equatorial Guinea. It is the latter which is generating the most fear among scientists, with authorities struggling to track cases of the disease. To date, there have been 38 cases and 34 deaths, suspected and confirmed, giving a case fatality rate of 89 per cent, although many infections are thought to have gone undetected.
“We’re concerned,” says Dr Dunning. “I’m more concerned about Equatorial Guinea than Tanzania currently, because there’s a wider geographic distribution of the cases I’ve seen across different provinces. We just have to watch it very closely.”

Should a case of Marburg make its way to the UK, several steps will be taken before the patient is passed into the care of Dr Dunning and his team at the Royal Free.
The first involves actually diagnosing the infection. This responsibility lies with the rare and imported pathogens laboratory (RIPL) run by the UK Health Security Agency.
The lab receives several calls a day via its 24/7 hotline from concerned clinicians whose patients have recently travelled abroad and are showing symptoms of a VHF, such as a fever and gastrointestinal complications. Most of the time, these calls come to nothing.
“Hardly any of those end up being positive and, in fact, a large number don’t need testing and we can stand them down based on the patient’s exposure history and clinical factors,” says Dr Claire Gordon, the deputy head of RIPL.
Especially at times of a high-profile outbreak, community clinicians can become hyper-vigilant if they’re dealing with a sick patient who has returned from overseas. This was seen during the recent spread of Ebola in Uganda, with the laboratory reporting a notable uptick in calls from worried GPs.
“We calmly try to take them through the actual history [of the patient], get the details, and ask what it is about this patient that made them call us and then what the other differentials might be,” says Dr Gordon.

Where there is genuine cause for concern, the patient in question will be subject to further investigations and fast-tracked for testing at RIPL, which is based in the government's high-security Porton Down facility in Wiltshire.
Here, Dr Gordon and her colleagues are capable of turning around a full set of tests “in a matter of hours” to determine whether the patient does indeed have a hemorrhagic fever or is actually infected with a less serious tropical disease like malaria, which is more commonly reported.
The testing team can be brought in at any time to conduct testing, including the middle of the night. “There’s always a team on standby and a backup team if needed,” adds Dr Gordon.
Once a test is confirmed as positive, the NHS springs into action. Depending on the infection – and whether it spreads by air or touch – the patient could be sent to any one of England’s dedicated centres for tropical and infectious diseases.
But only the Royal Free, in London, and Newcastle’s Royal Victoria Infirmary have the isolation facilities capable of treating a case as serious as Marburg, Ebola or Crimean Congo hemorrhagic fever.
Sealed in a plastic tent
The technology behind these units, known as a Trexler isolator, was first developed in the 1970s as means for creating a positive pressure environment, free of bugs and germs, in which pure lines of animals could be bred. Over time, it has been evolved to keep medics safe when treating patients with deadly infections.
Patients are effectively sealed into the plastic tent, unable to leave until they’re given the green light by doctors, who make a decision based on whether the pathogen, whatever it may be, is still detectable in blood, stool and urine samples.
The psychological and physical demands of this confinement are considerable, but “we do everything we can to make it more comfortable for them with TV and iPads and all those things,” says Dr Dunning.
The tent at the Royal Free even has a small exercise space where a patient can stand and stretch out.
For children, the team does not use the isolator tent, which can “be very distressing for all involved”. Instead the medics dress in full protective suits.
But the benefit of the Trexler isolator is that “I can train anyone in 10 minutes how to use that system,” says Dr Dunning. “We had 158 different members of staff over a three-to-four week period who had direct hands-on contact with the [Lassa fever] patient, including external specialists like a radiologist who came in to do a scan.”

The Royal Free has two of the tents, each based in a separate room. Nurses and doctors looking after an isolated patient must follow a strict one-way system: they enter through two sets of air-locked doors and, after delivering their care, leave via a walk-through shower.
“Even though we don’t wear PPE because the system is safe, we shower,” says Dr Dunning. “That’s also partly to provide reassurance to the staff working on the unit because there’s a psychological element of going home to your family dirty.”
All waste produced by patients kept in the Trexler unit is carefully removed in bags, mixed with granules that solidify it, and then sterilised – or “autoclaved” – in a room next door. At every stage of the patient journey, every precaution possible is taken to minimise the risk of an outbreak.
This commitment to protocol was put to the test in responding to last spring’s cases of Lassa fever and Crimean Congo hemorrhagic fever, which came after Covid-19 and a long spell without any patients with viral fevers. The last person to receive care in the isolation unit before then was Pauline Cafferkey, a Scottish nurse who was infected with Ebola in 2015 while working in West Africa.
“There was that element of ‘are we a bit rusty now?’,” says Dr Dunning. “We had also toned down a lot of our training because it was impossible to do our usual level during the pandemic.”
“But in reality, staff were amazing,” he adds. “It was slightly refreshing, in a sense, to deliver another type of expert care [different to Covid].”
When it comes to deadly diseases like Ebola and Lassa fever, it used to be assumed that luck would play as big a chance in a patient’s survival prospects as the care they received.
But the team at Royal Free have shown there is a way to dramatically improve the odds.
“In the old days, we’d say it’s too difficult to deliver intensive care to such patients,” says Dr Dunning. “Now, we’ve proved that we can do it.”
Protect yourself and your family by learning more about Global Health Security.

