Column: A new study calculates the incredible cost of ivermectin stupidity

A couple of things are known about ivermectin, the anti-parasitic treatment being promoted by a clutch of conspiracy-mongering mountebanks as a COVID-19 treatment.
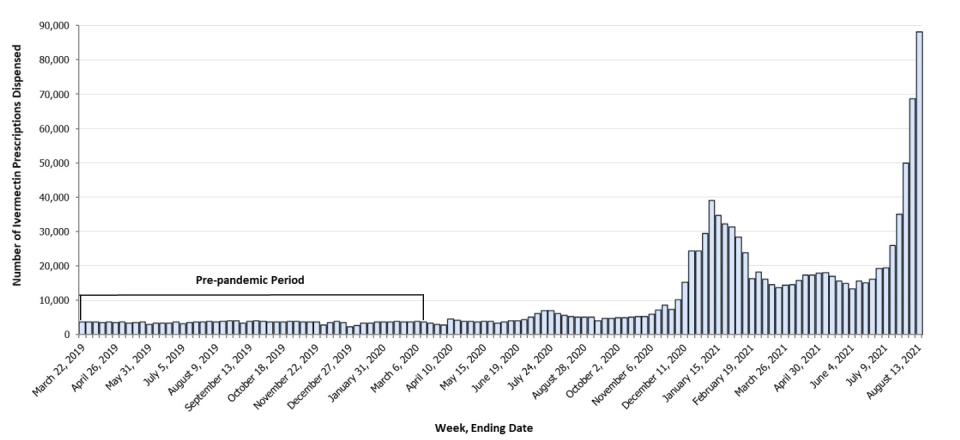
First, it doesn't work on COVID. Second, despite that fact, prescriptions for the drug have rocketed higher — from 3,600 a week pre-pandemic to 88,000 in one sample week in mid-August, according to the U.S. Centers for Disease Control and Prevention.
Third, the publicizing of ivermectin by anti-vaccine and anti-government activists duped naïve people to take a veterinary preparation of the drug, producing a spike in calls to poison control centers.
This is not the type of high-dollar item that an insurer is normally going to pay attention to. But the cost of inexpensive drugs, when dispensed frequently, can cumulatively add up.
Kao-Ping Chua, University of Michigan
Now, thanks to researchers at the University of Michigan and Boston University, we also know the financial toll of the ivermectin craze. In a research letter published Thursday by the Journal of the American Medical Assn., they estimated that Medicare and private insurers wasted an estimated $130 million last year on ivermectin prescriptions for COVID.
"That's not small potatoes," the lead author of the letter, Kao-Ping Chua of the University of Michigan Medical School, told me. The unit cost of ivermectin pills is low — about $1 to $1.50 per pill — but the volume of wasteful prescriptions adds up.
The $129.7 million spent on wasteful ivermectin, the letter's authors calculated, is more than the annual Medicare spending on unnecessary imaging for lower back pain, a low-value diagnostic order that has been widely researched. No one has paid much attention to the ivermectin expense, however.
The researchers' estimate may even be low for two main reasons. One is that their estimate is based on spending by private insurers and Medicare, but not Medicaid, which also covers the drug.
Second, they arrived at their figure by extrapolating from that one week highlighted by the CDC, when the average of new cases in the U.S. was running at about 150,000 a day. On Jan. 12, the daily average of new cases was more than 782,000. If ivermectin claims are tracking new cases, Chua says, then they may be getting filled at more than five times as often as last August.
Finally, consider the indirect cost. "By decreasing financial barriers to ivermectin, insurers are essentially facilitating access to a drug that some people use as a substitute for COVID vaccination," Chua observes. "In that sense, they could be raising their own costs for COVID complications."
That's correct. Ivermectin has become just one more item in the medicine chest promoted by the anti-vaccine crowd. The most serious study found it has "no effect whatsoever" on COVID-19. Ivermectin pushers do argue, as Chua noted, that it's an alternative to vaccination. That's not a conclusion based on science, but an instrument of ideologues.
As with the entire crusade against COVID vaccination, promoting ivermectin is a reckless attack on public health and a disservice to victims who are duped into making bad choices for their health and safety.
The researchers' letter points to what is fundamentally a breakdown in our system for overseeing drug prescribing.
It's true that ivermectin is approved by the Food and Drug Administration as a treatment for parasitic diseases. (Its more common veterinary use is as a deworming preparation for cats, dogs and livestock.) It's also true that doctors are generally permitted to prescribe any drug for "off-label" use — that is, for conditions for which it wasn't originally approved.
But that doesn't mean that pharmacists and insurers are legally bound to fill and pay for those prescriptions. Pharmacists are entitled to refuse to fill prescriptions they believe aren't intended for legitimate medical purposes. Indeed, some pharmacists have reportedly turned away patients who show up with ivermectin prescriptions for COVID. Insurers make judgments all the time about whether they'll cover certain drugs and for which patients.
But there are no indications that Medicare or private insurers exercised this crucial gatekeeping function on ivermectin. The probable reason is that each individual prescription is relatively cheap — about $35 to $50 for a 20-pill script, adding together customers' out-of-pocket co-pays and the insurance reimbursements.
"This is not the type of high-dollar item that an insurer is normally going to pay attention to," Chua says — a cancer drug, for example, that may run to tens of thousands of dollars per month or per year. "But the cost of inexpensive drugs, when dispensed frequently, can cumulatively add up."
Chua says that he was prompted to conduct his study after reading the CDC's estimate of 88,000 prescriptions in mid-August. "I thought to myself, 'I hope insurance is not paying for that,'" he says. But it is, and our entire healthcare system is shouldering the burden.
This story originally appeared in Los Angeles Times.

