COVID-19 hit Northeast states hard. Here's what they're doing to prepare for a surge
In early April, New York Gov. Andrew Cuomo warned that the state had only enough ventilators to last six days, despite waves of seriously ill coronavirus patients flooding into hospitals.
He revealed a plan to take the lifesaving breathing machines from upstate communities with limited outbreaks to aid the New York City-area hospitals hit hardest by the virus.
"I’m not going to let people die because we didn’t redistribute ventilators," Cuomo said, announcing the National Guard would be deployed to take the ventilators.
It ignited a firestorm over the chaotic response to dire shortages of medical supplies.
New York narrowly avoided running out of ventilators after getting an 11th-hour shipment of 1,000 devices from China, but the episode revealed the consequences of U.S. over-reliance on overseas manufacturing.
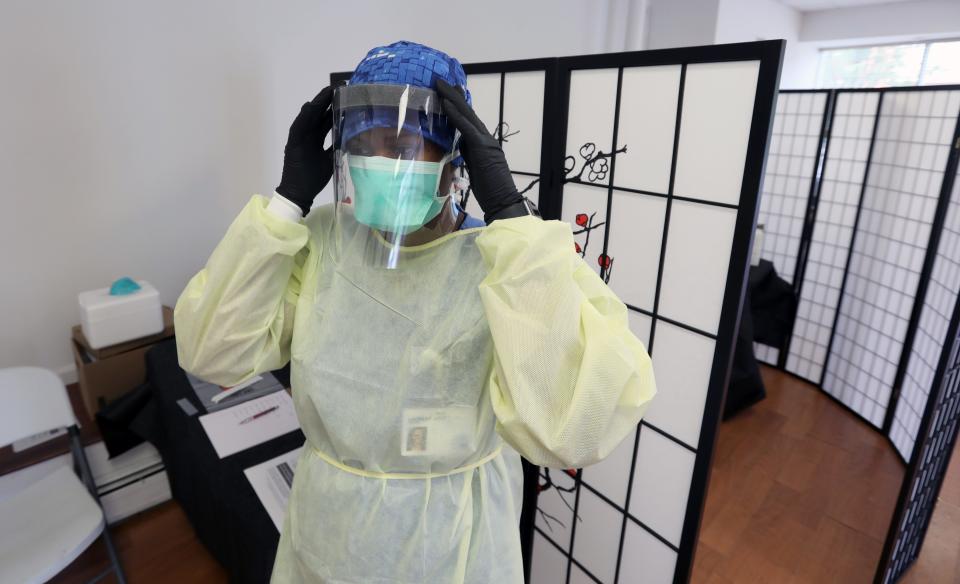
A dearth of personal protective equipment, which is also often made in China, underscored the problem and contributed to the coronavirus death tolls in New York and New Jersey of about 32,800 and 15,900, respectively, the highest nationally.
After all the death and suffering, the Northeast has the lowest infection rates in the country, but it is bracing for a second surge of COVID-19, the respiratory disease caused by the virus.
'We saw a spike in every borough throughout the city': NYPD creates Asian Hate Crimes Task Force after spike in verbal, physical assaults amid pandemic
Record-high COVID-19 infection rates in other parts of the country renewed reports of medical supply shortages, spanning from personal protective equipment (PPE) and testing supplies to disinfectant wipes and drugs.
Some health care workers and experts asserted all levels of government have failed to sufficiently shore up medical supply and distribution chains heading into the fall, complicating debates over reopening schools.
“We have not done enough, and I am deeply concerned that we will have ongoing COVID with influenza as well,” said Dr. Lewis Kaplan, president of the Society of Critical Care Medicine.
“I am very concerned that we will reach that same place … where we will perhaps not have enough PPE again, and we will not have enough ventilators,” he said.
Dr. Aliaksei Pustavoitau, a critical care expert at Johns Hopkins University School of Medicine, said the Northeast’s response during the pandemic peak this spring exposed gaping holes in emergency preparedness in American medicine.
“The magnitude of what happened was not matched in the plans,” he said, adding the “supply chain was designed, in general, to move things just in time.”
“When those supply chains started breaking down, everyone started getting short,” he said.
How did the stock market hit a record amid COVID-19-fueled recession? Here's what experts say about the rebound

PPE challenges remain amid COVID-19 surge
In New York, state and federal officials announced measures to boost domestic production of medical supplies.
About $11 million in grants have been awarded to 20 New York-based companies to retool operations and manufacture COVID-19 supplies. The deals aim to produce millions of N-95 protective masks, testing supplies and a broad range of other gear.
In announcing the grants, Cuomo said, “The nation has learned a hard lesson about not having a supply chain for vital supplies based here at home in the U.S., and as a result we had to scour the globe for livesaving products.
“That won't happen again in New York,” he added, citing the in-state manufacturing push.
Less than 10% of the masks used in the USA are made here. China makes almost half the world’s masks, gowns, gloves and other PPE.
New York state health officials issued orders July 21 requiring hospitals to maintain at least a 90-day supply of PPE by Sept. 30, and a similar directive mandated nursing homes maintain a 60-day supply.
Any facilities that fail to meet the requirements could have their operating licenses suspended or revoked.
Many hospital operators reported struggles this month in obtaining protective gear.
'These spaces need to be saved': LGBTQ bars work to survive COVID-19

“There is limited supply available, and prices remain very high,” said Bea Grause, president of the Healthcare Association of New York State, the Albany-based group that represents hospitals and nursing homes.
Grause said health care operators work toward meeting the new stockpile mandate. Efforts to replenish state and federal government PPE stockpiles could prove crucial as cases rise nationally, she said.
As federal efforts to boost PPE production are expected to fall short, the status of many state stockpiles of medical supplies remain shrouded in secrecy.
Jill Montag, spokeswoman for the New York Department of Health, said the agency’s policy prohibits commenting on its stockpile.
Similarly, New Jersey state officials refused to disclose many details of their PPE strategy, including how many days’ supply of protective gear the state aims to have on hand or how close it is to achieving that goal.
State officials cited “homeland security concerns” as the reason for not publicly revealing the information.
What health care workers say about COVID-19 surge, PPE shortages
Reports of PPE shortages triggered pushback from nurses across the county.
Health care unions demanded state governments and hospitals disclose PPE supply information and improve safety standards and training for workers.
Judy Sheridan-Gonzalez, president of the New York State Nurses Association, said the situation evoked memories of hospitals and health care leaders ignoring nurses’ concerns about unsafe conditions at the beginning of the pandemic.
“They basically say we have a supply of PPE and we’re prepared, but that’s what they said six months ago,” she said. Many nurses “didn’t feel protected at work, and a lot of us got sick.”
Nationally, 24% of nurses say their employer provides a safe workplace, according to a National Nurses United survey in July, which noted that more than 165 nurses have died in connection to COVID-19.
The Health Professionals and Allied Employees union in New Jersey said the lack of proper protective gear, inadequate training and lax government enforcement of safety requirements caused hundreds of health workers to be infected with coronavirus.
The union members said a massive PPE shortage remains as the state reopens and braces for a possible resurgence in cases.
“We know if we are not safe, neither are our patients,” said Debbie White, the union president.
COVID-19 requires more than boosting testing, ventilator supply
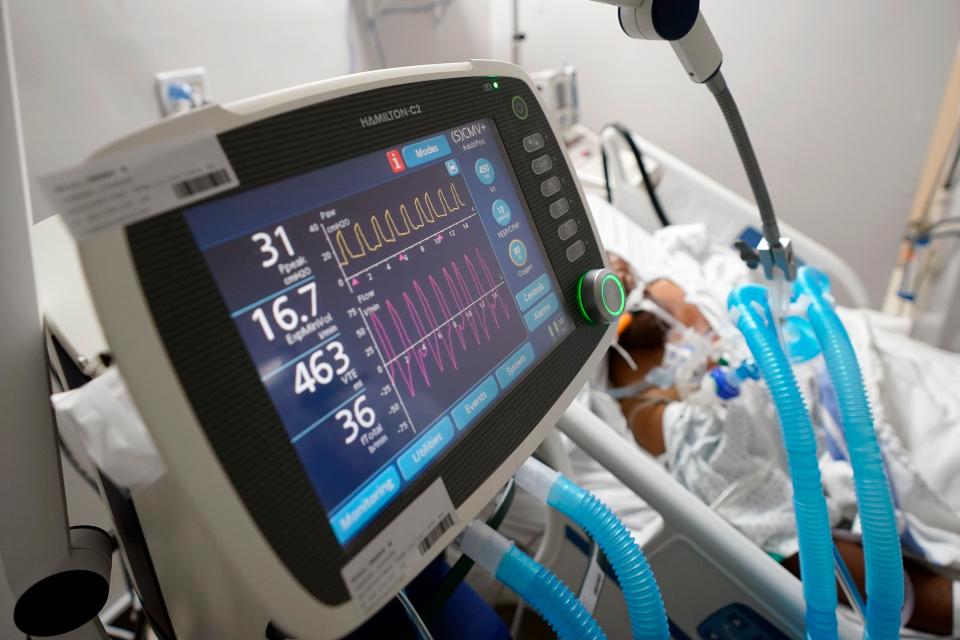
New York’s desperate scramble to find ventilators, in many ways, prompted federal officials to pay nine companies $2.9 billion for 187,000 of the breathing machines to boost national stockpiles during the pandemic.
Some health care experts expressed concerns that problems with distributing the ventilators, as well as deploying clinicians trained to use the devices across the country, remain unresolved.
“Globally, the ventilator supply is good,” Pustavoitau said. “But the problem that we have seen is how they were distributed to the areas of greatest need.”
Democratic lawmakers have pushed legislation seeking to federalize management of the medical supply chain, citing shortages throughout the pandemic.
The White House defended its handling of PPE and ventilator distribution and touted efforts to produce medical goods stateside, such as the $765 million government loan going to Rochester, New York-based Eastman Kodak to help expedite the domestic production of generic drugs.
Mounting concerns about surging COVID-19 cases have some health experts, unions and hospital trade groups warning that local and state leaders could lack the tools to contain the virus this fall.
New York's nation-leading COVID-19 testing infrastructure surpassed 6 million diagnostic tests since March, but challenges remain for contact-tracing programs to identify people potentially exposed to the virus and convince them to quarantine.
A Centers for Disease Control and Prevention survey last month found 54% of people infected with coronavirus were unable to pinpoint who may have infected them.
Experts said the survey results underscored how community and asymptomatic spread complicates contact tracing. In New Jersey, officials said this week people do not want to give information to contact tracers, hampering efforts to control the spread of the virus.
It all comes together as renewed strains on medical supplies and interstate travel endanger outbreak mitigation strategies across the country.
“This really needs to be a federal effort,” Kaplan said, which would entail better coordinating the flow of drugs and ventilators to doctors and nurses.
“We have a national health care crisis,” he said. “And I'd like to hear someone say we don’t have a national health care system, but in these key and important ways, we’re going to weld one together for all of us.”
Contributing: Lindy Washburn, Terrence McDonald and Alexis Shanes, USA TODAY Network
Follow reporter David Robinson on Twitter: @DrobinsonLoHud
This article originally appeared on New York State Team: After COVID-19 surge nationally, Northeast states prep for case spike

