COVID-19 patients struggle to get highly touted yet elusive antibody treatments
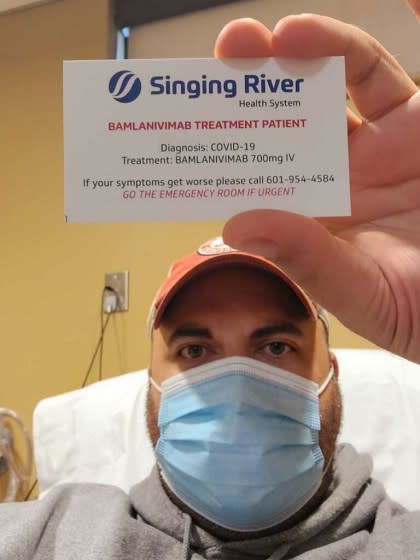
By the time he tested positive for a coronavirus infection, Gary Herritz was feeling pretty sick. His scratchy throat had progressed to a dry cough, headache, joint pain and fever. A liver transplant recipient, he knew his compromised immune system made him vulnerable to a severe case of COVID-19.
Herritz had read on Twitter about monoclonal antibody therapy, the type of treatment famously touted by Donald Trump after his release from Walter Reed National Military Medical Center. The Food and Drug Administration authorized its emergency use to keep high-risk COVID-19 patients out of the hospital — and, perhaps, the morgue.
But as his symptoms worsened, Herritz found himself very much on his own as he scrambled for access.
His primary care doctor in Pascagoula, Miss., wasn’t sure he qualified for the treatment. His transplant team in Madison, Wis., where he’d had the liver surgery, wasn’t calling back. From bed in Pascagoula, he spent two days punching in phone numbers for health officials in four states before he finally landed an appointment to receive the antibodies intravenously.
“I am not rich, I am not special, I am not a political figure,” Herritz, a 39-year-old former community service officer, wrote on Twitter. “I just called until someone would listen.”
The federal government has signed contracts to buy nearly 2.5 million doses of antibody treatments from Eli Lilly and Co.. and Regeneron Pharmaceuticals at a cost of more than $4.4 billion. Officials have allocated more than 785,000 doses of the treatments, and more than 550,000 of them have been delivered to sites across the nation.
But so far, only about 30% of the doses delivered have been administered to COVID-19 patients, according to the Department of Health and Human Services.
Across the country, high-risk patients who are eligible for the treatment have not been offered the option. Many aren't even aware that it exists.
The therapy is most effective if given within 10 days of a positive coronavirus test. Yet would-be recipients miss this crucial window due to a patchwork healthcare system that can delay testing and diagnosis.
“The bottleneck here in the funnel is administration, not availability of the product,” said Dr. Janet Woodcock, a veteran FDA official in charge of therapeutics for Operation Warp Speed.
Monoclonal antibodies are lab-produced molecules that act as substitutes for the body’s own infection-fighting antibodies. The treatments — which are delivered through IV infusions that require hours to administer and monitor — are designed to prevent the SARS-CoV-2 virus from attaching to and entering human cells.
Such treatments are usually prohibitively expensive, but for now the federal government is footing the bulk of the bill (though patients likely will be charged administrative fees).
The therapies are offered at nearly 4,000 sites around the country, but finding the sites and gaining access has been almost impossible, said Brian Nyquist, chief executive officer of the National Infusion Center Assn., which is tracking supplies of the antibody products.
Like Herritz, many patients seeking information about monoclonal antibodies find themselves on a lone crusade.
“If they’re not hammering the phones and advocating for access for their loved ones, others often won’t,” Nyquist said. “Tenacity is critical.”
Regeneron officials said their medical information line is fielding calls every day. And more than 3,500 people have flooded Eli Lilly’s COVID hotline with questions about access, a spokesperson said.
As of this week, states are required to list sites that have received the monoclonal antibody products, HHS officials said. But a listing doesn’t guarantee availability or access; patients still need to check.
Some health systems have refused to offer the therapies because doctors were unimpressed with the research results used to justify their emergency use authorization. Early studies suggested Lilly’s therapy, called bamlanivimab, reduced the need for hospitalization or emergency treatment by about 70%, while Regeneron’s cocktail of casirivimab plus imdevimab reduced the need by about 50%. But those studies were small, involving just a few hundred subjects, and the results were limited.
“A lot of doctors, actually, they’re not impressed with the data,” Dr. Daniel Griffin, an infectious diseases expert at Columbia University, said on his podcast “This Week in Virology.” “There really is still that question of, ‘Does this stuff really work?’”
As more patients are treated, however, there’s growing evidence that the therapies can keep high-risk patients out of the hospital. That not only eases their recovery, it decreases the burden on health systems struggling with record numbers of patients.
Dr. Raymund Razonable, an infectious diseases expert at the Mayo Clinic in Rochester, Minn., said he has treated more than 2,500 COVID-19 patients with monoclonal antibody therapies and seen promising results.
“It’s looking good,” he said, declining to provide details because his results are set to be published in a medical journal. “We are seeing reductions in hospitalizations; we’re seeing reductions in [intensive] care; we’re also seeing reductions in mortality.”
Banking on observations from Mayo experts and others, federal officials have been pushing for wider use of antibody therapies. HHS officials have partnered with hospitals in three hard-hit states — California, Arizona and Nevada — to set up infusion centers that are treating dozens of COVID-19 patients each day.
One of those sites went up in late December at El Centro Regional Medical Center in California’s Imperial County, a farming region on the state’s southern border that has recorded one of the highest coronavirus infection rates in the state.
For months, the medical center strained to absorb the influx of patients, but the new walk-up infusion site has already put a dent in the COVID-19 load. More than 130 people have received the two-hour infusions and then been sent home to recuperate.
“If those folks would not have had the treatment, they would have come through the emergency department and we would have had to admit the lion’s share of them,” said Dr. Adolphe Edward, the medical center's chief executive.
It’s important to make sure people in high-risk groups know to seek out the therapy and to get it early, Edward added. He and his staff have been working with doctors and nonprofit groups in the area and relying on word-of-mouth to spread the message.
“On multiple levels, we’re saying, ‘If you’ve tested positive for the virus, come and let us see if you are eligible,’” Edward said.
Greater awareness is a goal of the HHS effort, said Dr. John Redd, chief medical officer for the department's assistant secretary for preparedness and response. “These antibodies are meant for everyone,” he said. “Everyone across the country should have equal access to these products.”
For now, patients like Herritz say reality is falling well short of that goal. If he hadn’t taken matters into his own hands, he wouldn’t have been treated. And without the therapy, he fears he was just days away from landing in the hospital.
“I think it’s horrible that if I didn’t have Twitter, I wouldn’t know anything about this,” he said. “I think about all the people who have died not knowing this was an option for high-risk individuals.”
JoNel Aleccia writes for Kaiser Health News, an editorially independent program of the Henry J. Kaiser Family Foundation. It is not affiliated with Kaiser Permanente.
This story originally appeared in Los Angeles Times.
