My family endured pandemic-like isolation once before – when our son was in the NICU
- Oops!Something went wrong.Please try again later.
When the Centers for Disease Control and Prevention signed off on the Pfizer-BioNTech COVID-19 vaccine for teenagers, I scrambled to get some into the arm of my 14-year-old son. He had recently been diagnosed with asthma. And the quarantine had been a reminder of an earlier time of isolation – one that many families endured before this pandemic, and which still must be enforced on nearly 1 in 10 babies born in America.
I’ve watched, and worried, about my son's lungs since he was rushed to intensive care shortly after his birth. He had arrived with a condition known as transient tachypnea of the newborn, or TTN: rapid, shallow breathing caused by amniotic fluid in his lungs. The lungs – unlike the heart – don’t "turn on" until the first breath. In some cases, the fluid lingers after birth and clogs the alveoli, air sacks in the lungs.
Most cases of TTN pass within a day or two, but this one didn't. He developed double pneumonia, his skin turned a bluish gray and he was transferred by ambulance to a neonatal intensive care unit, a NICU, where he was put onto a ventilator.
Vault for the vulnerable
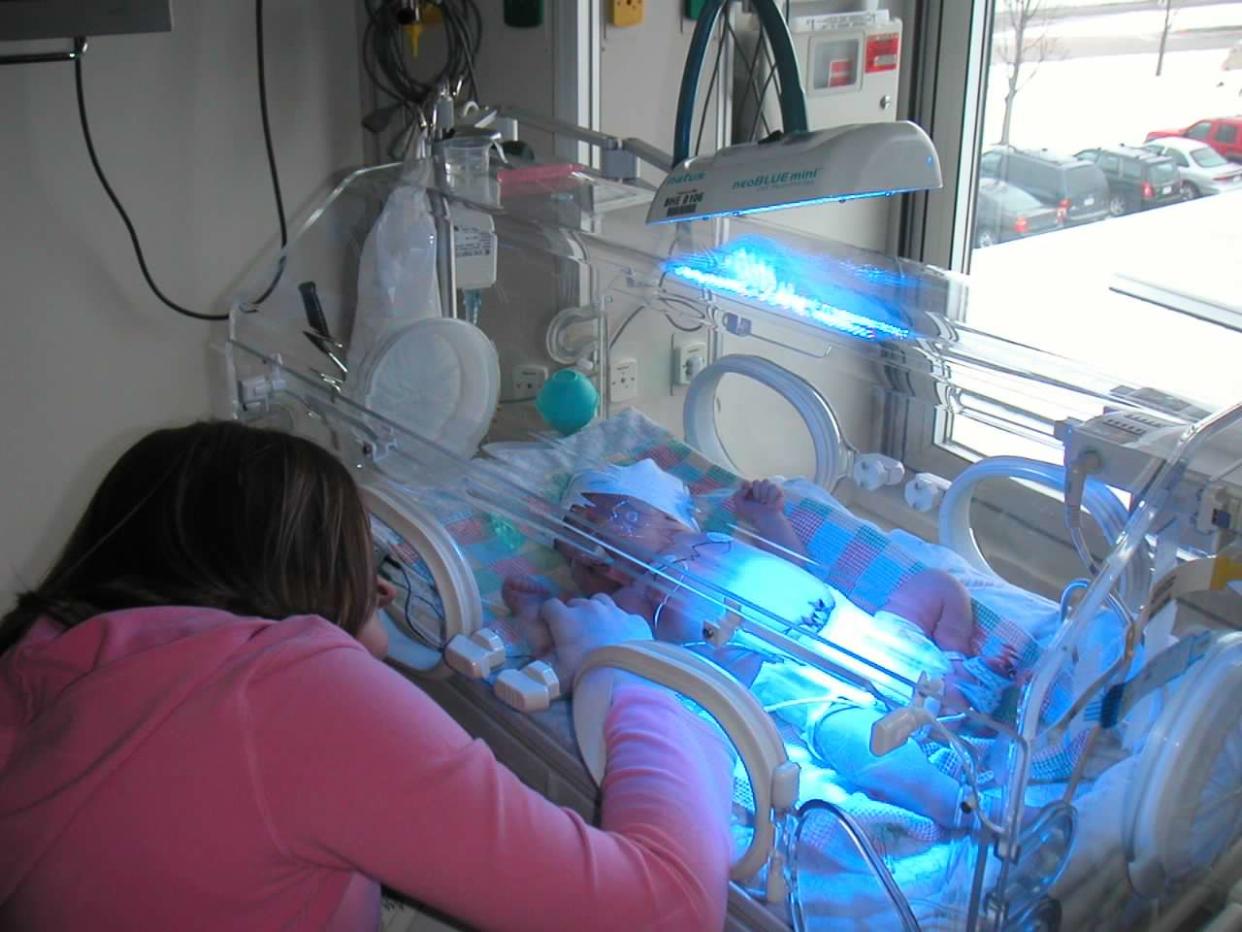
The NICU is a little-seen vault of a major hospital where some of the most heart-wrenching scenes unfold. When I peered through the windows of the other pod rooms, I saw newborns so tiny they defied logic: smaller than my hand and weighing barely more than a pound. They were flanked by glowing, hissing, honking machines, and by parents whose faces betrayed their fearful resolve to go the distance with their children.
These places are expensive, of course, and can even function as reserve armies in times of dire need. In December of last year, as regular ICU space in California plunged to nearly nothing, St. Joseph Hospital in the city of Orange changed a dozen of its neonatal beds for adult use, letting grown people use ventilators designed for tiny lungs, such as those of my son.
Teacher Larry Strauss: We're finally back to school after COVID-19 but it's complicated, confusing and strange
Then came a strange coincidence. A month after our son came home, my wife – a medical social worker – took a job in the NICU at our local Catholic hospital in Wisconsin. I was already fascinated by the NICU, given our experience, but once she started working there, I became obsessed. I plied the nurses and doctors with questions at every staff party we attended, and spent six months as a volunteer in the unit, motivated by nothing more than a desire to be closer to the stories my wife told over dinner.
Neonatal medicine has advanced at an almost meteoric rate in the last decades. In 1963, Patrick Bouvier Kennedy, son of President John Kennedy and first lady Jaqueline Kennedy, was born 5 1/2 weeks prematurely and died 39 hours later of respiratory distress syndrome, or RDS.
Today, thanks to the development of steroid therapy and surfactant replacements, the National Institutes of Health reports "a remarkably good chance of surviving” for infants born with RDS. Premature infants can often weather an ever-expanding list of conditions once considered deadly, and in general American hospitals will try to save babies born as early as 22 weeks of gestation.
In rare cases, babies born even earlier, barely halfway through pregnancy, have survived.
Watch and wait – and hope
For the “extremely premature” – babies born before 28 weeks – a NICU admission means months of quarantine not only inside the unit but also inside a Plexiglas Isolette. Complications, setbacks and surgeries, common enough that parents are warned to expect them, add days, weeks and sometimes months to the length of stay. Parents can do little more than watch and wait.
NICU families thus know what the rest of the world has only recently had to learn: the importance of masking and fanatical handwashing, and the blessing of a hot meal left on a doorstep. More than anything, they know isolation. While a preemie’s world is confined to a small box, the spaces occupied by the parents’ are only slightly larger: a corner of a small room, if they’re lucky enough to have a private room; otherwise, a glider chair in a curtained bed space.
Giving birth in a pandemic: Even as coronavirus rages, we have a reason to celebrate life
The lights inside the unit stay dimmed, the Isolettes covered with quilts, and everyone speaks in whispers. Due to the risk of infection, personal cellphones and visitors other than a baby’s parents are disallowed, and that often includes grandparents. During my stint as a volunteer, one mom told me that being in the NICU is like being in a vortex. She'd show up after breakfast and before she knew it, the sun was going down.
Once a baby left the NICU, often the rules got even tighter. For months, the baby could not go to the supermarket, church or family gatherings. Because the infants were housebound, so too were at least one of their parents. In most cases – though certainly not all – a baby’s immune system and lungs would eventually catch up and normal life, or something like it, could resume. But no one could say for sure when what would be.
After the storm
Many NICU parents I met told me their time in the unit was hard for their friends and families to understand, as was the anxious caution they felt for years afterward. Their babies had come through, hadn’t they? Wasn’t everything OK now?
Yes and no. While more premature infants survive now than ever before, the American Academy of Pediatrics reports that greater than 20% of NICU parents still experience symptoms of post-traumatic stress disorder a year after leaving the unit. You can take the baby out of the NICU, but taking the NICU out of the family is another matter.

Many people who’ve survived the coronavirus will likely experience similar PTSD symptoms, perhaps for years to come. So, too, will the family and friends who watched their loved ones suffer and die. Perhaps the pandemic, for all its horrors and inconveniences, will help us understand one another a little better.
The world changed forever: My son was born on 9/11 — now he's graduating high school in a global pandemic
I felt hopeful, watching the nurse plunge the needle into my son’s shoulder and deliver his first dose of the vaccine. He was safe, and we could finally start to put the pandemic behind us. Upstairs in the very hospital where our quarantine was ending, other quarantines were still going, and would keep going for a long time. Somewhere in my city, a baby was arriving impossibly early, on the very edge of life. That baby's quarantine, and his parents’, was only just beginning.
David McGlynn’s most recent book is "One Day You’ll Thank Me: Lessons from an Unexpected Fatherhood." He is a professor of English at Lawrence University in Appleton, Wisconsin, and recently completed a book about life in the neonatal intensive care unit.
You can read diverse opinions from our Board of Contributors and other writers on the Opinion front page, on Twitter @usatodayopinion and in our daily Opinion newsletter. To respond to a column, submit a comment to letters@usatoday.com.
This article originally appeared on USA TODAY: COVID: NICU babies, parents used to isolation, quarantine

