First in line, still no shot: Surprising number of hospital workers refuse vaccines
Bob Nevens hoped to retire at Houston Methodist, where the 47-year-old had served for a decade as director of corporate risk. Instead, Nevens was fired on April 29 after he refused to have a COVID-19 vaccine injected into his arm.
Nevens’ hospital in the Houston area was among the first in the nation to require the vaccine and remains one of a handful doing so. Houston Methodist set an early deadline for its 1,255 executives and managers and Nevens was one of only two managers who failed to step up. Other workers have until June 7 to comply.
Nevens has a list of concerns: the vaccines were made quickly, the FDA authorized them for emergency use, and the long-term side effects may not be known.
“I don’t want to take an experimental vaccine,” Nevens said. “We don’t know what it’s going to do to somebody 10 years from now.”
He is also convinced he has built-in immunity from contracting COVID-19 on a hiking trip with his wife in Hawaii in December 2019, about the time China revealed the first few cases in Wuhan. He has no evidence that he ever had the illness, however. An antibody test later came back negative; Nevens does not believe it.
“There’s no way that anybody could tell me what I had was the flu,” he said.

Houston Methodist CEO Marc Boom was disappointed that Nevens declined the vaccine. But he defended the hospital’s decision.
“It’s the right thing to do,” he said. “It puts patients first. It puts hospitals in a leadership position from a safety perspective.”
Hospital workers, many of whom risked their lives during this pandemic and saw the ravages of the virus up close, were first in line for the vaccines. Yet Nevens is among a sizable group of hospital workers still not vaccinated.
USA TODAY surveyed some of the largest hospital networks and public hospitals in the country. At the nine networks that responded, fully vaccinated rates ranged from 53% to 72%. Rates among 15 of the nation’s largest public hospitals ranged from 51% to 91%.
The survey encompassed 276 hospitals, or about 4.5% of the nation’s hospitals. Most fell below President Joe Biden’s goal of 70% by July 4. Staff included ranged from workers with medical training, such as doctors and nurses, to those in support roles, such as cafeteria workers.
The fact that so many hospital workers remain unvaccinated is troubling news for public health officials who are counting on the vaccines to stop the spread of the virus. Experts worry that the rest of the population will follow suit.
“I think it’ll be a bit of a struggle to get to that 70-to-75% vaccination rate,” said Stacey Gabriel, the chief executive officer of the 80-bed Hocking Valley Community Hospital in Logan, Ohio, where only 50% of her workers are vaccinated.
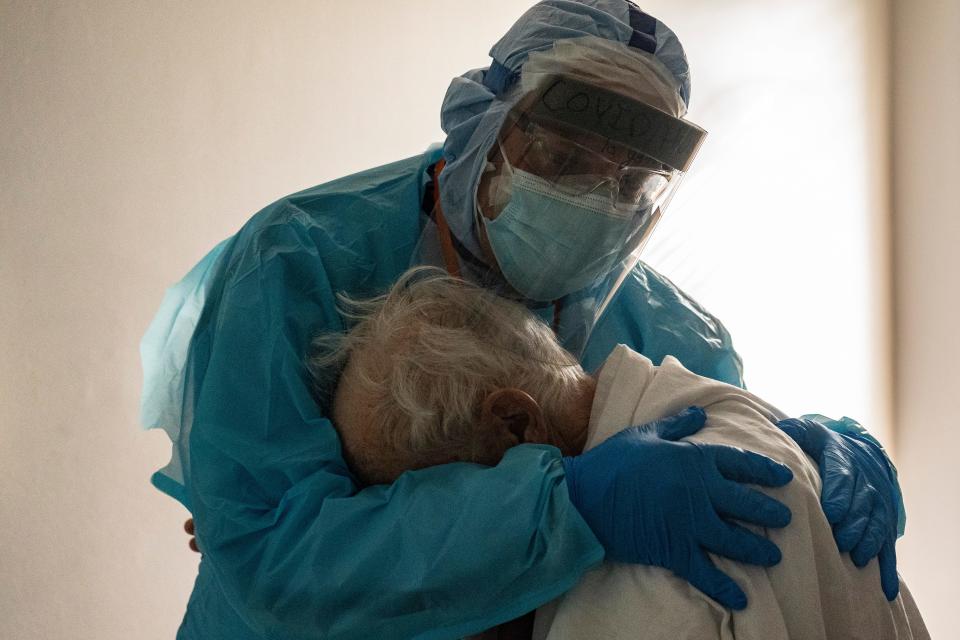
In the COVID-19 unit at Houston’s United Memorial Medical Center, Dr. Joseph Varon has taken only four days off since the outbreak began. Varon, who heads up the unit and is chief of critical care, is concerned that unvaccinated staff might spread the virus to patients.
“What I don’t understand is how come 40% of my nurses who have worked with me in my COVID unit, where three patients die every day, they still say no,” he said.
Hospital administrators say after an initial rush by those who could not wait to get the vaccines, demand plateaued and then fell dramatically. At most hospitals, the rates have remained stuck for weeks.
Vaccination sites are witnessing a similar pattern among the population at large. Gabriel said her hospital in a small community in Ohio was giving out 300 shots a week not long ago. In one recent week, only 16 people showed up. When the University of Pennsylvania planned to give out 2,500 shots at a high school in west Philadelphia, only 400 people came.
About half the adults in the U.S. are now fully vaccinated, according to the Centers for Disease Control and Prevention. Some experts suggest the country may need to hit closer to 80% of the entire population to reach herd immunity and fully contain the spread of the virus.
New COVID-19 cases nationwide have plummeted since people started getting vaccinated. Still, some are concerned that if 30% or more of the adult population remains unvaccinated and life begins to return to normal, another wave of COVID-19 cases could follow.
“I think that could leave a reservoir of vulnerable people out there,” said Patrick J. Brennan, an infectious disease doctor and the chief medical officer for the University of Pennsylvania Health Systems.
Mandating vaccines a balancing act
One way to increase the vaccination rates is for employers to mandate them. Although controversy continues about whether employers can require employees to get vaccinated, several colleges already are requiring the shots. A few hospitals have joined them.
So far, most hospital executives USA TODAY interviewed seem sympathetic to concerns that the vaccine is new and hasn’t gotten full FDA approval. That has contributed to the decision by many not to mandate it yet.
Houston Methodist started with an incentive, offering a $500 bonus to any worker who got vaccinated by March. Boom said that boosted the vaccination rate to almost 85%.
Then the flagship hospital and its six community hospitals, confirmed that it would mandate the vaccine. Today, rates are up to almost 99%.
So far, at least four other hospital groups have announced that they are mandating the vaccine, including Benefis Health System of Montana, RWJBarnabas Health in New Jersey and most recently University of Louisville Health in Kentucky.
The University of Pennsylvania also recently announced it would require that all employees and clinical staff be vaccinated by Sept. 1. Currently, nearly 70% of the staff are vaccinated, although Brennan said rates among doctors and pharmacists are closer to 90%.
A key factor in the decision was that the systems’ six hospitals treat quite a few cancer and organ transplant patients as well as elderly patients highly vulnerable to the virus, Brennan said. He believes that hospital workers are more likely than the general public to get vaccinated, but they also share many of the same fears.
Some of the greatest resistance is political. A Monmouth University poll in April found that 43% of Republicans versus 5% of Democrats do not plan to get vaccinated. Less than half of the GOP caucus members in the House have acknowledged getting vaccinated.
Sen. Rand Paul, a Republican from Kentucky and an eye doctor, has refused to get the vaccine. Paul, the first known senator to test positive, says he’s already immune.
“The hardest gap is the political battle – people who don’t want it for political reasons,” said Dr. Susan Smith, senior vice president of the University of California San Francisco Health, which includes four hospitals and outpatient clinics. “That’s hard to close because it’s just been so polarized nationally.”
UCSF is not mandating the vaccine but it is requiring all employees to either get vaccinated or seek a waiver by explaining why they are declining the vaccine by June 30.
One public hospital group that has taken a softer approach is the University of New Mexico Health. It reported the highest vaccination rate in the USA TODAY survey at 91%. The group was partly blessed by being in a state with a high vaccination rate. According to the state health department, 56% of the state is fully vaccinated now.
But the provider recently staged a 10-day campaign to get its rate to 100%. The campaign relied primarily on education and barely made a difference, increasing it to about 91.5%.
“Clearly, being unvaccinated still today puts you at risk,” said Douglas Ziedonis, the health care provider’s chief executive officer. “That message would be, ‘If you have not been vaccinated, get vaccinated. Just because you had COVID before doesn’t mean you’ll be immune from these new variants.’”
Rural hospitals fall farthest behind
Rates at hospitals tend to mirror the communities around them. While states in the Northeast and on the West Coast have among the highest vaccination rates, low rates linger across much of the South.
Ardent Health Services had one of the lowest rates in the USA TODAY survey at 53%. It owns and operates 30 hospitals in six states with most concentrated in New Mexico, Texas and Oklahoma.
The fully vaccinated rates in Texas and Oklahoma remain below the national average: 43% and 38% respectively, according to the state public health departments.
Rural hospitals have among the lowest rates. A survey by the Chartis Center for Rural Health and the National Rural Health Association found less than half of workers were vaccinated at nearly a third of the 160 hospitals that responded.
“We were gobsmacked,” said Chartis rural hospital expert, Michael Topchick. “We expected to see some with lower rates. We couldn’t believe the percentage with those rates right around 50%.”
Rural areas tend to be more Republican and echo some of the same skepticism about the illness as former President Donald Trump, who once called the CDC’s death toll for COVID-19 “far exaggerated.”
Melissa Fisher, 53, does not work at a hospital but, as a caretaker at an assisted living facility in Athens, Tennessee, she shares many of the hospital workers’ concerns. In addition, she has a religious objection, calling the vaccine the “mark of the beast.” Some of her church’s elders and her pastor have compared the vaccines to the apocalyptic prophecy in the New Testament’s Book of Revelation.
“We have a freedom of choice in this country. That’s what our forefathers fought and died for, and right now I think it’s being taken away from us with this vaccine,” Fisher said.
Her employer, Enlivant, based in Chicago, is requiring the vaccine, so Fisher had to find another job.
Legal questions arise about mandates
Most hospitals require employees to get flu vaccines annually, and data shows mandating that vaccine works. According to the CDC, at hospitals that required it, more than 94% of workers got the flu vaccine in 2019. At hospitals that did not require it, less than 70% got vaccinated.
The influenza vaccine has a long track record, having been introduced in 1945. The FDA approves it each year.
Hospitals may be hesitant to mandate the COVID-19 vaccine because none of the vaccines have full FDA approval. Two of the vaccine companies, Pfizer and Moderna, have applied for that approval, which would make their vaccines available even after the public health emergency ends. The FDA is reviewing their data.
The 2004 law allowing emergency use authorization says that each person must be told “of the option to accept or refuse administration of the product.”
Legal experts say that language does not necessarily preclude employers from mandating the vaccine, however. Both the U.S. Equal Employment Opportunity Commission and the Occupational Safety and Health Administration have given employers guidance for requiring the vaccine.
Boom, the hospital CEO, said lawyers for Houston Methodist have assured him that it is legal for employers to mandate the vaccine. He expects other hospitals to follow suit eventually.
“It is legal for health care institutions to mandate vaccines, as we have done with the flu vaccine since 2009,” Boom said in a statement. “The COVID-19 vaccines have proven through rigorous trials to be very safe and effective and are not experimental.”
Last week, 117 employees of Houston Methodist filed suit against the hospital system for requiring the vaccine. The lawsuit alleges that the clinical trials will not be completed for another year and the FDA still doesn’t know all the facts about the vaccines. The suit also harkens to cruel Nazi experiments and the Nuremberg Code, which says that people need to give consent to be part of an experiment.
One of the plaintiffs is Jennifer Bridges, a 39-year-old nurse who treated patients in the COVID-19 unit at the Baytown community hospital. That unit catered to patients who didn’t need intensive care, but Bridges said she did care for COVID-19 patients who eventually died.
Not only does Bridges refuse to get vaccinated, she also has an online petition to stop mandatory vaccinations currently signed by more than 8,000 people across the country.
“I speak for a lot of people,” Bridges said. “We just wanted it to be fully FDA approved. We wanted enough time for it to have the proper research.”
Bridges’ concerns go beyond waiting for more data; she is convinced the vaccine is making people ill.
“I’ve seen... everything from blood clots, heart attacks, heart arrhythmias,” she said. “We’ve had people that were perfectly healthy and the day after they took the vaccine, they literally woke up and they couldn’t move or feel their legs.”
The adverse events data is closely monitored by the FDA and an independent data safety monitoring board oversees data for ongoing trials of the vaccines. So far, the most serious adverse reaction linked to the Johnson & Johnson vaccine was extremely rare blood clots in the veins of the brain combined with a low platelet count. One person has died from that condition.
Bridges believes that her hospital is engaged in a coverup of adverse reactions.
“A lot of physicians are being told to not report it,” she said.
She also says a worker in information technology claims that they participated in a group chat with hospital managers who were instructing workers not to document adverse reactions on patient charts.
Houston Methodist adamantly denies Bridges’ charges of a coverup, saying in a statement: “This is also completely false and unfounded. We pride ourselves on being one of the safest hospital systems in the country, and we would never do what she alleges.”
“It is unfortunate that Ms. Bridges is choosing to act this way. She is a disgruntled employee making unfounded claims and putting herself before our patients by not getting a vaccine. Her messages have become increasingly personal and unprofessional and her efforts appear co-opted by the anti-vaccine movement.”
Contributing: Holly Meyer, The Tennessean.
David Heath is a reporter on the USA TODAY national investigations team. Contact him at dheath@usatoday.com or @davidhth, or on Signal at (240) 630-1962.
This article originally appeared on USA TODAY: Covid-19 vaccines refused by a surprising number of hospital workers

