Former CDC head on coronavirus testing: What went wrong and how we proceed
A series of errors with lab testing delayed the U.S. response to the Covid-19 pandemic. We need to be clear about what went wrong and how we can get things right.
A month after other countries started testing, we still had not. The administration made three mistakes: The Centers for Disease Control and Prevention test kit was flawed, and its response to that error was slow; the Food and Drug Administration was slow to allow hospital labs to develop their own tests; and the Department of Health and Human Services didn’t work with commercial labs to start developing broadly available private sector tests until far too late.
Because of this, communities missed the first indications of community spread, and response only ramped up after large numbers of cases started to appear, weeks after transmission began.
Failure to identify early community spread provided a false sense of security. The president claimed he inherited a “broken and frankly terrible system,” but during the 2009 H1N1 pandemic, the CDC developed and began shipping more than 1 million tests to all states and 140 countries just two weeks after the virus was discovered. Had HHS, the White House and CDC functioned in the coordinated way they had previously, the system could have performed as well as it did with other major health threats, including H1N1, Ebola, Zika and the Middle East respiratory syndrome (MERS).
There must be an organized, effective plan in place
Effective emergency response requires a systematic, coordinated approach. There must be a strategy that adapts through different phases of the response and includes contact tracing, isolation, health care worker safety, tracking systems, control of clusters and outbreaks, research, tracking of genetic change in the virus, and more. Testing works as an integral part of that response and has different roles at different times.
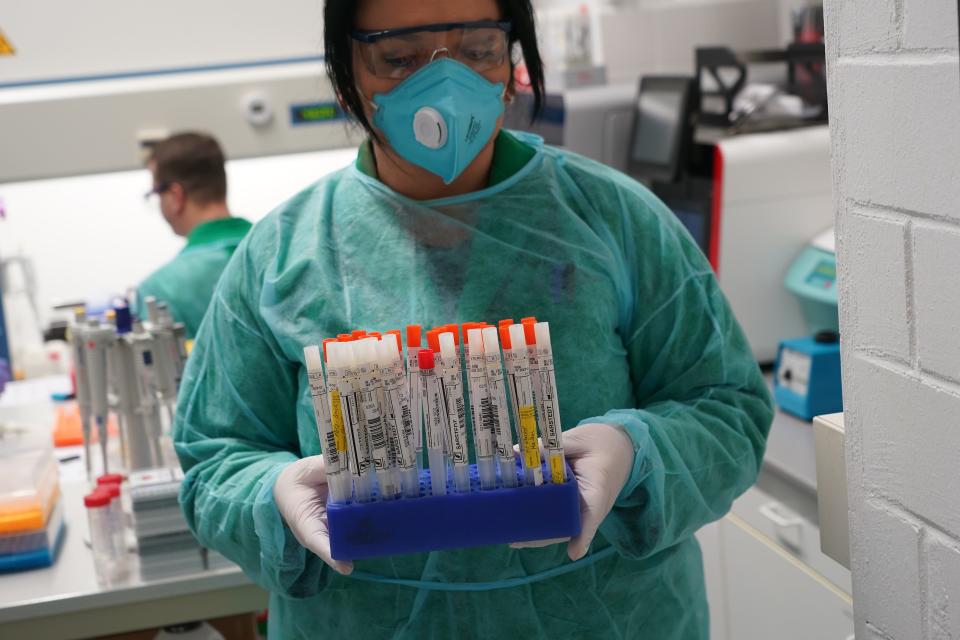
There is a confusion about testing. The right goal for testing depends on the stage of the epidemic at a given time and place. We have developed a concept of operations for actions to take at different stages. Initially, when cases are rare, the goal is containment by isolating each infected person, finding each of their contacts and testing those who develop symptoms (and, ideally, contacts who don’t). This — done extremely well — worked to control outbreaks of severe acute respiratory syndrome and MERS. But the COVID-19 virus has proved to be much more infectious.
My week with coronavirus: This is no joke, even a mild case in a young person
When containment fails and there are a large numbers of cases, as is happening today in New York City and many other parts of the country and world, contact tracing is simply not possible at the scale needed, and physical distancing interventions — sheltering in place — are needed. As cases decrease, contact tracing can resume in the suppression phase of the response, to prevent large scale transmission from happening again.
The role of testing changes over time
To help fight the pandemic as effectively as possible, the testing approach must evolve with the spread of the virus:
►In areas with few or no cases, testing can inform containment strategies and facilitate contact tracing. People who have symptoms can thereby be safely and rapidly isolated to prevent further spread.
►In areas with widespread transmission, testing is essential to find outbreaks in hospitals, nursing homes, homeless shelters and prisons. For people who don’t need to be hospitalized and aren’t in a congregate setting, a test won’t change what needs to be done: Stay home, isolate. People with only minor symptoms won’t benefit from testing. A negative test doesn’t mean you are in the clear; many patients who initially test negative will later test positive.
►In the suppression phase, more extensive testing, both for current and past infection, will help identify and stop emerging clusters and facilitate reopening society. We will need to respond rapidly to new clusters as they occur until we have a vaccine. Drive-thru testing may have a particularly important role in this phase, as it did in South Korea.
►Throughout all phases, for tracking, epidemiological investigations and planning, testing can help determine how widespread infection is, identify risk groups and transmission patterns, anticipate next steps, and guide planning and development of appropriate strategies. Every patient requiring mechanical ventilation or with pneumonia anywhere in the country should be tested to find out whether spread is occurring and to make health care safer.
Q&A: Coronavirus response sidelines CDC, and former CDC chief feels 'less safe'
New tests on the horizon promise results while the person waits. This will enable health care workers to know right away whether a person should be hospitalized, isolated or quarantined.
Testing is starting to catch up to the pandemic in the United States, but testing is just one part of a strategy. Testing can help protect health care workers, improve treatment and, when part of a coordinated strategy, reduce the number of new cases.
As the pandemic evolves, our ability to detect and respond to it is improving, and eventually so will our ability to limit its return.
Dr. Tom Frieden is a former director of the Centers for Disease Control and Prevention and a former commissioner of the New York City Health Department. He is president and CEO of Resolve to Save Lives, a global non-profit initiative that is part of the global public health organization Vital Strategies. . Frieden is also Senior Fellow for Global Health at the Council on Foreign Relations. Follow him on Twitter: @DrTomFrieden
You can read diverse opinions from our Board of Contributors and other writers on the Opinion front page, on Twitter @usatodayopinion and in our daily Opinion newsletter. To respond to a column, submit a comment to letters@usatoday.com.
This article originally appeared on USA TODAY: Former CDC head on coronavirus testing: Where we go from here

