Inside a Kansas City COVID unit: Busy nurses, ventilators, unvaccinated patients
- Oops!Something went wrong.Please try again later.
In a brightly lighted ICU room she lies in a bed, eyes closed, hair splayed against the pillow. She looks to be in her mid-40s but could be younger, because fighting for weeks to breathe when COVID-19 is stealing your air takes a toll.
Oxygen that’s been humidified and heated flows hard and fast into her nose through the tubing of a cannula. IV bags, hanging in a forest of tall metal poles next to the bed, drip fluids and medicine into her veins.
On this recent afternoon, she and nine other patients wage private wars in the COVID intensive care unit at University Health.
The ICU beds have been full nonstop for weeks as the highly contagious omicron variant sends waves of seriously ill patients to this hospital, formerly Truman Medical Center, and others across the region. Hospital leaders have banded together to warn that the record number of cases is pushing them beyond their limits.
University Hospital allowed a Star reporter and photographer onto the ICU unit at the campus south of downtown to see what the surge of cases has wrought for patients and staff.
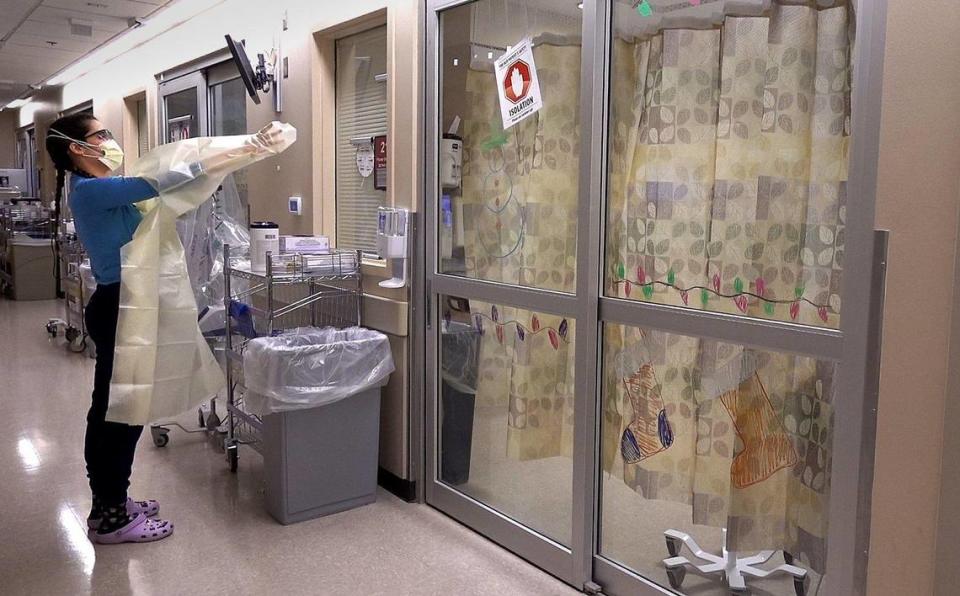
On this day, University Health is taking care of 133 COVID patients at this hospital and its Lee’s Summit campus. Among them, 26 are receiving intensive care.
“We have overflow of COVID ICU patients in all the other units, in the other ICU as well. This is the fullest we’ve been in the whole of the pandemic,” said Delaney Swanson, a registered nurse on the COVID unit.
Some patients have spent weeks behind the locked doors of this second-floor unit, where machines monitoring blood pressures and heart rates beep with metronome consistency. Once on this afternoon, a much cheerier sound rings out as Brahms’ Lullaby plays throughout the building when a baby is born.
COVID is pushing the staff hard. Phones are ringing constantly in the hospital’s call center, which takes up four adjacent conference rooms on the ground floor of the hospital near downtown.
Shannon Flint, manager of the operation, said the staff has fielded between 900 and 1,200 phone calls from the public every day for the last two weeks.
In early December, the daily number was 400.
Right now, most are calling to get tested for COVID at the hospital’s drive-thru operation in its parking garage, though there has been a slight uptick in people who — finally? — are following doctors’ recommendations and seeking the vaccine.
As of Friday, University Health had performed 191,847 COVID tests and given 135,077 doses of vaccines, a hospital spokeswoman said.
At this hospital, and every one in the Kansas City metro area, most of the COVID patients in ICU and dying are unvaccinated.
Last month, University Health made a video of two COVID patients who spent Christmas in the hospital pleading with people to get vaccinated. Sarah Kiehl, a registered nurse on the COVID ICU unit, knew one of the patients, Anita Gardner.
“She was with us for several weeks even before she was interviewed” in the video, said Kiehl, who in December 2020 was the first person announced in Kansas City to receive the vaccine. “And she had said to me, ‘As soon as I get better I’m going to get vaccinated.’”
Gardner died on Jan. 6.
Kiehl said ICU patients express regret “all the time” about not getting vaccinated, and many times it comes right as they’re about to be sedated and intubated with a tube snaked into their trachea so they can be placed on a ventilator. Reality spreads across their face.
They tell her they were scared of the vaccine and serious side effects or even death — which health experts say are rare.
“There’s a solemn look of concession, almost, and realization like ‘I made the wrong choice’ as it sets in just how severe the illness is. And they’ll usually mention that they wished they had gotten it,” she said.
The sluggish interest in vaccinations concerns Charlie Shields, University Health’s president and chief executive officer.
“If you look at what we’ve seen as a result of omicron, it hits really hard the unvaccinated population. I think if you’ve been vaccinated, the health care professionals would tell you that the odds are really with you that even if you get it, you will likely do well.”
The groups that Shields worries about “are unvaccinated and have the underlying health conditions that exacerbate their experience with COVID, whether they’ve got diabetes, whether they’re overweight. You can just see all these things that add up. … They’re very high risk.”

The Braid-y Bunch
The rooms on the COVID ICU unit, which used to house cardiac patients, are negative pressure, or isolation rooms, used for patients with infectious, airborne diseases. When the glass doors slide open, contaminated air stays inside because the air pressure is lower than outside the room.
The dirty air gets sucked out through an exhaust system that filters it before pumping it away from the building.
Patients here have spanned the age range; some have been teenagers. On this day, the patients are mostly in their 30s to 60s. Average length of stay has been two to three weeks, nurses said, though one patient they got especially close to spent two months with them.
The hustle around the nurses’ station is constant. Things speed up when patients leave because there are others sick with COVID waiting for those beds on other units in the hospital, in the emergency department and at other hospitals.
One nurse said it seems like death comes here more frequently now.
“I’ve unfortunately said goodbye to many patients, in the room, holding the hand of a patient after they passed while the family members stood outside crying,” said registered nurse Kenzie Yurkovich. “All of us have done that.”
They’re working extra hours because hospitals are understaffed as COVID cases surge and employees themselves get sick and stay home. Reports of nurses across the country leaving bedside care or leaving nursing altogether are becoming more frequent as the pandemic drags on.
“Obviously it’s been challenging,” said Shields. “We’ve been upwards of two years dealing with this now. It certainly wears on people.
“But I would tell you that when you go up in the ICUs and talk to our staffs, whether it’s nurses, techs, doctors, they’re doing this every single day. They’re still committed, the compassion is there.”

For these nurses, buying each other snacks and coffees and drawing holly leaves and Christmas decorations on patient’s doors are brief moments of joy in the belly of the beast.
University Health set up “resiliency rooms” on each campus, break rooms where staff members can take a breather, put on a virtual reality headset and escape to happy places like sunny beaches, if only for a few minutes.
Several female nurses wear their hair pulled back in braids — a plaited ponytail on one, two French braids on the back of another nurse’s head. They call themselves “the Braid-y Bunch.”
Braiding each other’s hair at the beginning of a shift gets it out of the way of masks and face shields, but has also become a comforting act of self-care. These nurses are taking care of each other, too.
“it’s tough to explain to the rest of the world what we’re experiencing,” said Kiehl, who has worked at the hospital eight years.
“It’s exhausting,” said Swanson. “We know what it’s like to work on a day when we’re understaffed so we don’t like to do that to each other.
“But we also know if none of us go home and take time for ourselves that we won’t really be able to recharge because it’s not easy.
“A lot of us are still trying to find ways even after all this time to stay afloat with it all, but I can’t say many of us have been successful yet. I think it’s almost like a Stockholm syndrome to it now. None of us want to step away from taking care of our COVID patients.
“But we all recognize that it’s been detrimental to ourselves and our loved ones because we pour a lot into our patients and each other at work and then we don’t really go home and have a lot of energy for things at home and for our hobbies and things like that.”

The nurses have had to educate a lot of people about this virus whose complications can come roaring back with a vengeance, even after a loved one seems to be recovering. It’s a confusing, frustrating cycle for family members.
“We see a lot of people pass away and a lot of families who don’t understand why they’re losing their loved ones to this COVID,” said Swanson, who joined the COVID ICU team six months into the pandemic to get intensive care experience.
They “have a hard time understanding why their loved ones, even if they tested COVID positive weeks ago, are still here in the ICU and why they’re still doing so poorly.
“And it often leaves so much residual damage to the lungs with COVID pneumonia that a lot of our patients, that’s what kills them.”
There’s been drama at the bedside as well. Some of these nurses have been accused by family members of not trying hard enough to save their loved ones, even after lengthy CPR procedures. That absolutely doesn’t happen, Shields said. Vaccinated or not, every COVID patient here is “going to receive great care,” he said.
“I want others to know that we do anything for our COVID patients, vaccinated or not,” said Swanson.
“We just want the best for them, healing for them, and it’s hard fighting something that is such a big beast after all this time and so many unknowns.”
The nurses have fended off slings and arrows outside of work, too. Some have been accused by strangers and even people they know of exaggerating, even lying about, the severity of the pandemic. It’s hard not to take it personally.
“It’s tough. But like I said, we lean on each other,” said Kiehl. “At the end of the day we know we come here and we do everything we can. At the very least we have our truths.”

Kansas City stepped up
In April 2020 the hospital allowed The Star in to see how it was preparing for the pandemic. The place was eerily quiet after elective surgeries were canceled, clinic visits were cut back and office employees sent home to work.
Shields was convinced at the time that if Kansas Citians would just stay home, socially distance and avoid crowded spaces, the city would be spared the chaos that COVID had created in bigger cities like New York.
And that’s just what happened because the community did the right things, said Shields.
“I think, if you go back, look early on in the pandemic, clearly the actions that were taken by the community, whether it was masking, social distancing, trying to limit big gatherings, that helped us get to a point where we didn’t exceed our capacity,” Shields said.
“At the time our therapeutics weren’t as evolved as they are today. We didn’t know as much. So all those actions were the right thing to do at the time and they helped us get to a place where we could manage.
“We never got to a position where we had to open up non-traditional settings as hospitals where we entered crisis standards of care, where we had to make really difficult decisions and triage patients.
“I think this community’s actions allowed us and prevented us from getting to that point, which I think was really important.”
The pandemic is roaring again thanks to omicron, but this time, even though vaccination rates are not where hospital leaders would like to see them, hospitals have therapies they didn’t have two years ago, said Shields.
New oral therapeutics are coming, “so even folks who are compromised because of other health conditions, but have been vaccinated, there are still solutions for them that should put them a little bit at ease,” he said.
The hospital also runs a monoclonal antibody infusion center for high-risk patients with mild or moderate symptoms, and is switching over to treatments specifically for omicron, Shields said.
Swanson said she doesn’t want to leave the COVID ICU until she sees more of those strides in patient care “and our abilities to treat this and not just constantly trying to catch up to the symptoms of it but to get ahead of it and help these people in ways we haven’t been able to yet.
“And I think that’s the biggest factor that keeps me with my COVID patients, is that we all want a victory over this. And I hope it’s soon.”
The Star’s Jill Toyoshiba contributed reporting.

