It may not have started here, but the novel coronavirus became a US tragedy
On Feb. 29, 2020, hundreds of people packed into the Pullman Christian Reformed Church, a squat, beige brick building on Chicago’s South Side. An attendee began the ceremonies by blasting a shofar, the trumpet made out of a ram’s horn. Somebody played keyboard. And a long line of people waited to speak into a microphone about their memories of Angeli Demus.
The lifelong Chicagoan, who had died a month earlier at age 59, insisted she didn’t want it called a funeral. “Donate, cremate, celebrate,” had been her credo to her family near the end of a gutting battle with lung cancer, and with her eyes donated and her body cremated, all that was left was this party.
Her husband, Earl Demus, billed it as “Angeli’s Joyous Celebration,” and thought that the crowd it gathered spoke to his wife’s beloved nature. “Standing room only,” recounted Demus, who estimated there were more than 450 people there. "I stopped counting after a while.”
Your subscription makes award-winning journalism possible.
If you liked this story, read more of our most popular premium journalism:
How the FBI played a role in the capture of Princess Latifa of Dubai Prominent cheerleading gym disregards sex abuse allegations Collapsed condo born of botched construction and evidence of money laundering
The disconcerting news story that seemed recently to creep into every conversation, particularly after it tanked the stock market the previous week, didn’t make it past the doors of the church. Nobody wore a mask or kept their distance, and for the most part nobody even talked about the novel coronavirus. It had only started to trickle into the United States, as far as anybody knew, and the few cases in Illinois were said to be isolated and controlled.
A top health official had a week earlier assured Chicagoans that “the health risk to the general public from novel coronavirus remains low,” and the outlook from the highest levels of government was that, nationally, the few instances of the virus were disappearing. President Donald Trump had said three days earlier there were 15 cases in the country, and “the 15 within a couple of days is going to be down to close to zero.”
In a room off to the side of the church, people sipped soft drinks and picked at a spread catered by a neighborhood chef: finger sandwiches, sliders, fruit and cheese, chicken and Angeli’s favorite dessert, cheesecake. This room was where her father, Charles Dungill, spent most of the event.
Everybody called him “Cookie,” a throwback to his days as a drummer in a family band that toured everywhere Black performers were allowed in Jim Crow's America. Cookie shook hands, hugged and chatted with relatives and friends, some of whom had traveled from California, Michigan, Georgia, Ohio and Nevada. A family friend was fresh off a golfing trip to Arizona and another had recently returned from South Africa.
It was the West Chatham diaspora, a testament to the lasting bonds of the tight-knit Chicago neighborhood in which Cookie and his wife, Barbara, had raised Angeli and her three surviving siblings: brothers Sevil and Kyann, and sister Gina.
A couple of days after the celebration at the church, Sevil stopped by Cookie’s house to check on him. The kids were worried about their dad. They’d noticed little changes in his appearance: a slight droop to his posture, something different in his eyes.
It wasn’t just his daughter’s death with which he was reckoning. Barbara, his wife of 63 years, had died less than a week before Angeli’s celebration, after suffering from multiple ailments, including cancer.
But Sevil found his dad in good enough spirits, having enjoyed the event at Pullman so much that he wanted to plan the same thing for Barbara. Father and son chatted for about three hours, during which Sevil noticed that his dad had a slight hitch in his throat.
Probably post-nasal drip.
The next day after work, Sevil was driving back to his dad’s house, bringing him Barbara’s ashes from the crematorium, when he realized: Now he had a little cough, too.
“You know, just a hee-mmh,” Sevil later recalled.
***
Before the nearly 300,000 deaths, the widespread financial devastation, the isolation from loved ones and the fatigue of a daily disaster with no clear end, there was this: A tickle in a throat in Chicago. A woman’s sudden crash to the floor of her kitchen in the Bay Area. A playwright in Manhattan with three-quarters of a lung left in his chest, sensing doom and fleeing down the coast with his husband.
The virus shouldn’t have been able to sneak up on the United States. The world’s most powerful nation, historically among the most successful at stymieing infectious illnesses, had ample lead time during which the deadly pandemic was rampaging through Asia, and then Europe.

But in an early vacuum of leadership at almost every government level, with the message from the White House that the virus was not anything to worry about, Americans unwittingly spread the lethal virus to loved ones and strangers alike.
The U.S. squandered its early advantage. Roughly one year after the virus first came into existence, the country has suffered a loss of life far worse than any other.
Dr. Megan Ranney, an emergency physician and professor at Brown University, said COVID-19’s traits made it a formidable opponent for even those large nations most competent at fighting it.
But, she added, in the United States in 2020, the virus found an ideal victim. “The virus could not have emerged at a better time for spread than this year,” Ranney said. “We were in an election year. We had a president who didn't believe in science. We had underfunding of our public health institutions. It was a perfect storm.”
In an effort to better understand how the virus exploited the country's strengths and exposed its weaknesses, USA TODAY interviewed biologists and studied scientific genomic analysis, federal reports concerning super-spreading events, county medical examiner’s data from around the country, and state-level death and infection data.
Reporters used those sources to find and report the stories, many of them previously untold, of Americans in the path of the virus.
What emerges is a portrait of misinformation and confusion leading to a devastating failure to unite against a common threat.
Piecemeal policies offered a dangerously hollow illusion of control and safety. Scientists, intermittently ignored and villainized, were powerless. As citizens protested and rioted in response to racist police tactics, others detected a more subtle form of prejudice in apathy toward a virus that disproportionately sickened Black and Brown Americans. Early ignorance about the spread metastasized into partisan conspiracy-mongering and threats, leading to that most American phenomenon: a health official with a bulletproof vest.
The novel coronavirus didn’t start in the United States, but we have made it our own.
MLK Jr. Day: Zero official deaths
On Jan. 23, Dr. Benhur Lee stayed up late in his Manhattan apartment, working through the global ramifications of the virus Americans had been told was not a threat to them.
“We have it totally under control,” Trump had said the day before when asked about the single known case in the United States. “It’s one person, coming in from China. It’s going to be just fine.”
But none of the early epidemiological research Lee was picking up from China, where the virus had killed thousands and brought life to a standstill, suggested that assessment was correct.
Lee runs a research lab at Mount Sinai’s medical school in New York City. He made a name for himself as an HIV researcher in the early 2000s before moving on to tracking emerging viruses, becoming an expert on viruses such as nipah, the bat-borne sickness featured in the film "Contagion."
Lee was one of thousands of scientists throughout the world who had since December been piecing together small studies from doctors in other countries to understand the features of the virus that had emerged in Wuhan, with their clues as to how it could be stopped.
In early January, scientists from China and Australia released an initial genome sequence of the virus. It closely resembled SARS, the virus that much of the world barely dodged two decades earlier. And on this Thursday night, Lee couldn’t sleep because scientists had just released new findings estimating the human-to-human spread of the novel coronavirus.
It was as infectious as Ebola, slightly less infectious than the 1918 Spanish flu, and much less infectious than HIV and malaria. Lee tried to put the data in context by tweet. Over next few months, his Twitter account – @VirusWhisperer – would gain tens of thousands of followers.
Lee knew that the United States had previously benefited from a mix of luck and coordination between U.S. agencies and their international counterparts in stemming SARS and Ebola. That history was cold comfort to Lee, who knew that the factors making a virus dangerous were difficult to predict.
The scientific community was not yet in agreement that the virus was capable of asymptomatic spread. Because carriers often don’t know they have it and in turn don’t isolate, asymptomatic spread is a boon for a virus’s rate of infection.
Lee didn't need a double-blind study to determine what was happening. The way the virus had blitzed across China was evidence enough.
“There was obviously asymptomatic transmission going on,” Lee said.
Over the next few weeks, Lee would witness a study in contrasts in how seriously major nations were taking the novel coronavirus. On Jan. 25, he left for a microbiology conference in Sydney, stopping on the way in his home country of Singapore. It was the beginning of the Year of the Rat, and Lee was celebrating the holiday with a visit to his parents.
He landed just as news broke that Singapore had its first confirmed case, in a traveler from Wuhan. Officials with latex gloves and temperature guns checked for fever as he disembarked and boarded, and travelers from the Chinese province that includes Wuhan were barred from entering the country.
By the time Lee returned to the United States on Feb. 3, there were confirmed cases on both coasts and in the Midwest, and officials were announcing new ones every couple of days.
As he disembarked in Newark, New Jersey, Lee readied for the temperature check, the symptom screening, even the racial profiling of an Asian traveler.
Instead, he checked in at a digital kiosk just as he always did. There was no temperature check. The border official welcomed him into the country with no screening questions.
As he rolled his luggage out of the airport, Lee thought, That’s not good.
***
For Dr. Jeff Smith, the top administrative official of Santa Clara County in California’s Bay Area, it was a forgettable topic of conversation, just one spouse griping about work to another.
In December 2019, Smith – who in addition to being county executive is also a medical doctor and a lawyer – was chatting with his wife, a primary care doctor befuddled recently by an influx of patients seeking treatment for flu-like symptoms, including coughing, achiness and fever. But when she tested for influenza, it came back negative.
Smith had no reason to think much of it.
“It was just a matter of, ‘Well, gee, there’s people that are sick, and it’s a variant of the flu that doesn’t show up on the flu test,’” the county executive later said.
But the conversation nagged at him in the months to come.
By mid-January, the novel coronavirus was still just a slightly ominous curiosity to most Americans.

The first U.S. news reports about the virus, published earlier that month, were full of unanswered questions and mistaken reports from China, including the initial belief that the virus could not be passed between humans.
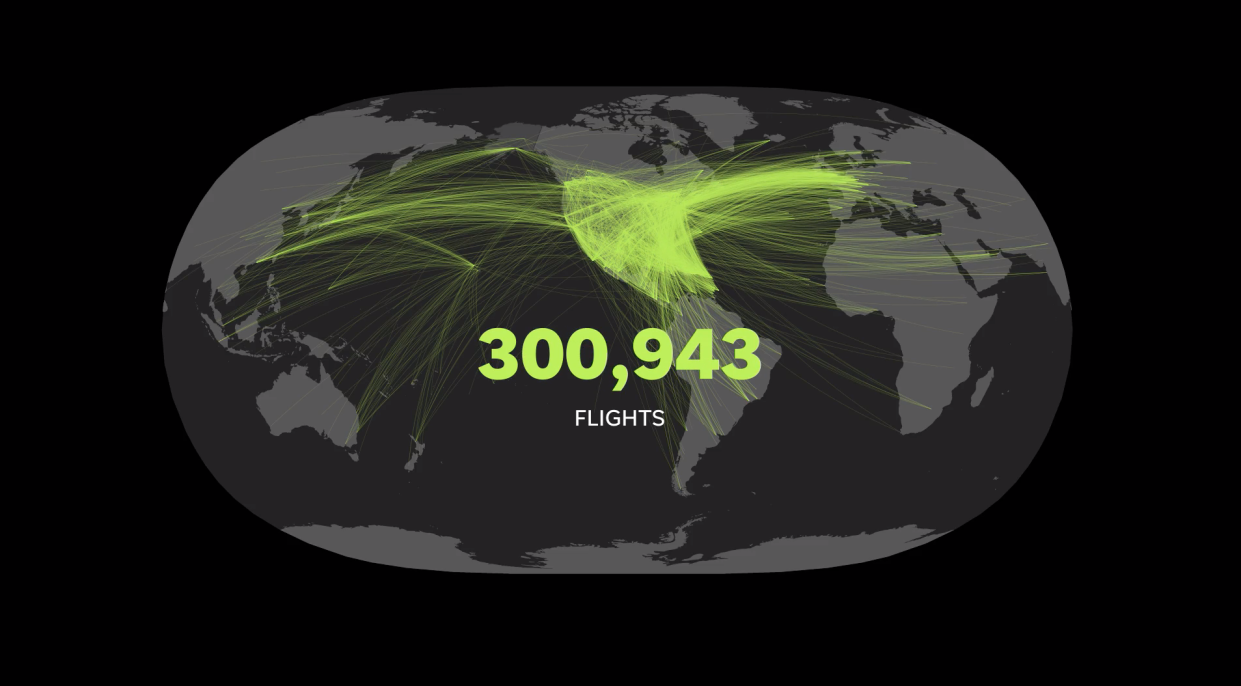
Life proceeded as normal. San Francisco's international airport was one of two in the United States that had direct flights to and from Wuhan. But members of the San Francisco Airport Commission, which oversees its operations, showed no concern throughout January that it was an open portal for travelers from the viral epicenter.
A review of the commission’s meetings that month showed that its members never discussed the novel coronavirus. The government body was instead immersed in its own drama: A restaurateur had been charged with attempting to give one of the commission members a $5,000 bribe to open a rotisserie chicken joint in the airport.
In the meantime, during the month of January, more than 2,400 passengers flew direct from Wuhan to San Francisco on China Southern Airlines Flight CZ659, according to a USA TODAY analysis of data on the VariFlight app.
When a member of the airport commission finally did address the virus in early February, it was to urge travelers not to change their plans for Chinese New Year, a holiday during which people often traveled abroad to visit their families.
"I think it’s important for us to continue these celebrations knowing that professionals and government are really taking the right precautions,” commissioner Malcolm Yeung said at the time.
The dynamics make the Bay Area a good case study for how the virus was allowed in unchecked.
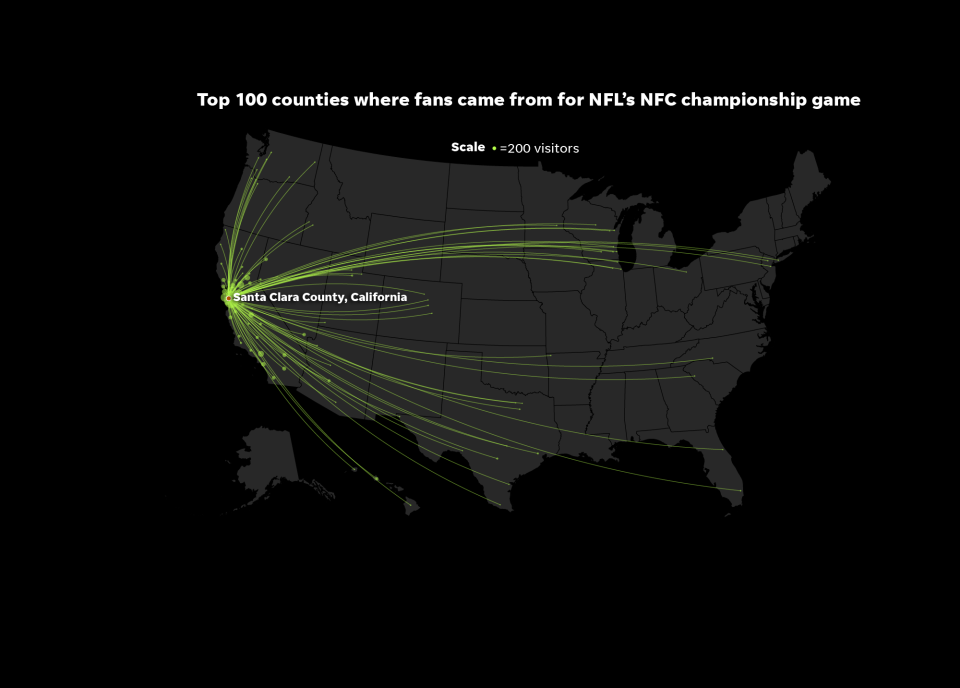
On Jan. 19, tens of thousands of fans packed Levi’s Stadium in Santa Clara for a major sports event: The NFL’s conference championship game between the hometown San Francisco 49ers and the Green Bay Packers. The winner would go to the Super Bowl.
At the time, most Americans knew relatively little about the novel coronavirus. The Centers for Disease Control and Prevention hadn’t announced any cases in the United States.
Fans flew in from all over the country to attend the game. Masks and social distancing were not yet part of everyday life.
Besides the few hours spent in the open-air stadium, fans stayed at hotels, ate at restaurants and shopped at stores in the surrounding Santa Clara County, population 1.8 million.

It’s impossible to draw a straight line from an event like this to a coronavirus outbreak without contact tracing, a non-factor at the time. But around the area, there were deaths unattributed to COVID-19 that seem suspicious in hindsight. Like a senior living home resident — stricken with symptoms including a persistent fever — whose family was stunned by her sudden decline.
Or the previously healthy 57-year-old woman who collapsed in her kitchen.
County health officials assured residents they had no reason to worry about COVID-19, even as coroners listed causes of deaths as “pending,” sometimes for months.
The virus wasn’t here, officials said.
On the same day as the championship game, a 98-year-old woman named Marjorie Waggoner lay in a hospice bed at a senior living center 14 miles away in San Jose, with a cold towel folded over her forehead as a measure against the fever that had plagued her for more than a week.
When her daughter Darryl Ospring took a photo of her that day, Waggoner was unconscious, scrawny and hollow-eyed. It was a dramatic change from how she looked less than two months earlier, in a photo Ospring took around Christmas.

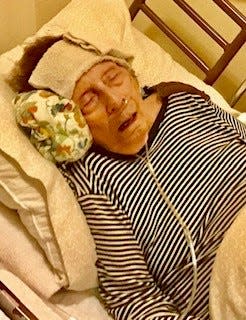
Waggoner, who her kids said always seemed decades younger than she was, wore carefully coiffed short curly hair, a cheesy holiday sweater, a necklace made of bells, and a big, childlike grin. She suffered from Alzheimer's and had been in hospice for a year following a series of falls, but she was faring so well that administrators were considering returning her to normal care.
But on Jan. 8, Waggoner was tired and had no appetite. Within a few days, she had developed a cough, and then a fever, and her condition rapidly spiraled from there. She died on Jan. 22.
Ospring was surprised by the cause listed on the death certificate – “complications from neurodegenerative disease” – given that her mother’s nurse had told her before she died that her chief ailment was her persistent fever.
Waggoner was not autopsied, and Ospring honored her request to be cremated, even if it ruined her chance at ever getting clear answers.
“I was trying to understand what happened to my mother in this small window of time,” she said. “It was as if the Angel of Death just came in and ushered her out.”
Unbeknownst to Ospring, she was not alone among residents of her county in being blindsided by the sudden demise of a loved one without a clear medical explanation.
On Feb. 6, a healthy 57-year-old named Patricia Cabello Dowd collapsed dead in her kitchen, the victim of what was initially declared a ruptured heart.
Twelve days later, 69-year-old Filipino immigrant Arturo Difuntorum Rivera was found partially decomposed in the home where he lived alone. For months, the medical examiner listed his cause of death as “pending.”
Their lives had no obvious overlap, and they occupied different social strata. Dowd was a manager at a semiconductor company that required regular international travel, though she hadn’t been overseas recently. Rivera was a security guard, who in recent employment at a hotel earned $14 an hour.
Neither was administered a blood test for COVID-19, and officially, there was no chance their deaths were related to the virus. That’s because Santa Clara County’s top health officials were unequivocal at the time in declaring that the virus was not spreading there.

At a public meeting Feb. 19, the county’s public health chief, Sara Cody, said there was no reason for residents to wear masks, cancel gatherings or seek testing for the virus if they were showing symptoms.
Cody said the county had only two confirmed cases, and both were travelers from Wuhan who had been ordered to isolate.
“If somebody’s not had travel to mainland China, we don’t consider them a risk for COVID-19 and don’t test,” said Cody, who projected a message reading: “Coronavirus is not currently circulating in our county.”
But there was no real way for county officials to gauge that, because testing was nearly nonexistent. On the day of Dowd’s death, there was a single novel coronavirus test administered in all of Santa Clara County, according to county data. On the date of Rivera’s death, there were two tests. The county didn’t top 1,000 tests a day until late April.

It wasn't until April 22 that the veil was partially lifted on what had been missed months earlier. Chief health officer Cody held a press conference announcing that posthumous tests had revealed that three deaths months earlier – those of Dowd, Rivera and a 70-year-old Filipino man named Rolando Olaguer – were actually due to COVID-19.
Cody called them "iceberg tips" of an unseen outbreak. Dowd became the earliest confirmed casualty of the virus in the United States, pre-dating a Seattle-area death on Feb. 28.
But for Ospring, who had no way of confirming whether her mother died of the virus, there was no such closure. Like many Americans, she tried to fill the void of ample initial testing with amateur epidemiological sleuthing. She went down a rabbit hole of trying to contact trace the person who did her mother’s nails shortly before she fell ill, attempting to see if she could link them to a known case.
She realizes she’ll probably never know. “The best I can do is get as close to the truth as possible,” Ospring said.
For county executive Smith, the revelation of early COVID-19 deaths made for a painful confirmation that his county’s policies had allowed residents to unknowingly infect and kill each other. He said his greatest regret was trusting the CDC’s guidance that there was no need for testing unless a person had symptoms and recent travel to Wuhan. Similar frustrations were expressed by health officials around the U.S. who felt the CDC, previously considered the world’s premier health agency, had failed the country due to egregious missteps and misinformation.
“I firmly believe that if the federal government had dealt with this appropriately, that many, many hundreds of thousands of Americans would not have died,” Smith said.
He’s thought back to those conversations with his wife in December, during which she told him about patients who had flu-like symptoms but tested negative for the flu. (Smith’s wife, who works for a private corporation, declined to be interviewed, citing medical privacy concerns.)
He now suspects that those patients had COVID-19, and that the virus has been circulating in his county since December. It’s a theory supported by academic research suggesting that the virus was in the U.S. then, including a UCLA study that revealed a major spike in patients with coughs and acute respiratory failure in the final month of 2019.
Smith shudders when he thinks back to the major gatherings such as sports events in the first few months of the year, including that NFC game in January that attracted more than 70,000 fans.
“Somebody in the future, some Ph.D. student, will do research on that particular game,” Smith said. “And I’m sure that there will be evidence that there was COVID spread.”
***
At the same time covid-19 was spreading unseen through northern California, it was gaining a similar foothold in other regions throughout the country.
For Sevil Dungill in Chicago, his family's battle – and to an extent his city's – with the virus began with thin-crust pizza and embraces of condolence from an old family friend.
It was Feb. 28, the night before the celebration of Dungill's late sister, and the friend brought him a pie from Home Run Inn.
They sat close together and, as they reached for slices of pizza, they lingered on everything but the novel coronavirus. Following the deaths of Dungill's sister and mother, the friend seemed to understand he could use a few-hour respite from talk of sickness.
SUBSCRIBE: Help support quality investigative journalism like this.
Dungill's friend wasn’t married and had no children. Instead he filled his life with extended families: his own, and those of which he was an honorary member. Every Thanksgiving he stopped by to visit the Dungills, and he called Sevil’s elderly parents on their birthdays every year.
Dungill's friend had recently had a little scare with the virus. He had briefly lost his senses of taste and smell. The friend, who USA TODAY is not naming because he declined to be interviewed, had been golfing in Arizona, where there were a handful of confirmed cases.
He knew the loss of those senses was a symptom. But his doctor prescribed him a steroid and assured him it was just his asthma acting up.
By the time Dungill's friend hugged him goodbye, saying he’d see him at his sister’s celebration the next day, whatever bug that seemed to have been bothering him was gone except for a mild case of the sniffles.
***
Less than two weeks later, at around 7 a.m. on March 11, Dungill sat in the emergency room waiting area of the Advocate Christ Medical Center.
Six others were also there seeking medical attention.
Dungill's illness had started about a week after his sister’s celebration. He had been at his office when, while reaching for a sweater, he realized he was freezing, while his eyes and forehead were burning.
“Hey, if a miracle happens, I’ll be at work tomorrow,” Dungill announced to his boss after toggling on his out-of-office email message. “Otherwise, I’m out sick.”
He made it back to his office after a couple of days off, but his fever persisted. His co-workers commented on how terrible he looked.
When it hurt to breathe, Dungill relented and had his wife drop him off at the emergency room.
The admitting medical personnel appeared unconcerned that his symptoms were related to the novel coronavirus. Though they gave Dungill a mask, none of the nurses or doctors wore any personal protective equipment themselves.
They told Dungill they couldn’t check for novel coronavirus. At the time, the CDC was only advising tests in cases that fit narrow parameters, such as if the person had traveled to mainland China.
However, because the doctors were concerned about blood clotting, they had Dungill undergo a CT scan.
The doctor who brought the results to Dungill's hospital bed donned a jarring get-up, now including a face mask and goggles.
The doctor explained that medical officials in China had reported that X-rayed images of the lungs of those infected with the novel coronavirus often displayed damage that looked like a starry night or a cobweb. Dungill's scans showed the same patterns.
Dungill blurted out a number: 845. It was the room in the same hospital where his dad was also laid up.
Cookie Dungill was dealing with his own persistent symptoms that doctors struggled to decipher. He had initially shown up to the hospital due to constipation causing stomach-clenching discomfort, but he had been sent home, diagnosed with a bad case of gas.
After the pain got even worse, he called an ambulance to take him back to the hospital. Even though one of the symptoms of COVID-19 was abdominal pain, the hospital had apparently ruled it out without a test. They had him share a room with a fellow patient.
“No, they didn’t test him,” Gina told Sevil when he asked about their father’s treatment. “They don’t think it’s that.”
Sevil said he urged his doctor to run the same CT scans on his father, and they came back with the similar telltale pattern. It kicked off chaos in Advocate Christ.
Nurses and doctors who had treated both Dungill men without protection were sent home. According to a later medical report, Cookie's “12 attending nurses were also tested and were positive for COVID-19 and quarantined.”
A spokesperson for Advocate Christ said they couldn’t comment directly on this case, but that their staff “consistently followed CDC guidance, which evolved as public health experts learned more about the virus and its transmission,” and that they required masks within the hospital starting March 31.
The doctors ultimately kept Cookie hospitalized but sent Sevil to the waiting area so his wife could pick him up and take him home.
It was 11:44 p.m., about 17 hours after Sevil had first arrived at the hospital. The room was now crowded with patients with symptoms just like his: red eyes and dry coughs and painful-sounding wheezes. Everybody had been given masks.
Sevil again took a tally. He stopped counting at 80.

***
The scientist Benhur Lee spent the first few months of 2020 trying to get people to fathom the severity of the virus already coursing through the country.
In mid-February, Lee bought Lysol spray, disinfecting wipes, and – even though the CDC was discouraging them – medical face masks.
Lee found it reprehensible that the agency was advising Americans against wearing masks and claiming that they were ineffective when scientists had long considered them a weapon against infection. So Lee carried with him a bag of masks and handed them out to strangers on the streets and subways of New York City.
He persuaded the doormen of his building to erect a plexiglass barrier between their desks and the lobby. He tried to convince colleagues – who were all scientists – that they were underestimating the virus. He joined a few dozen scientists who wrote a letter to New York City Mayor Bill De Blasio urging him to close schools.
Lee’s public health tweets got him branded as an alarmist. His inbox filled with threats or anti-Asian slurs, spurring Lee to take a hiatus from Twitter.
And then, in the second week of March – the same week that the World Health Organization declared the virus to be a pandemic – reality seemed to finally, if only partially, set in for the United States.
In a span of two days, the National Basketball Association suspended its season. Tom Hanks announced that he had COVID-19. And Trump declared a national emergency while banning many Europeans from entering the United States, adding to a partial ban on some foreign nationals who had visited China.
Lee’s employer, Mount Sinai, closed all biology labs, except for those doing research related to COVID-19. Lee pivoted to making an ingredient to test people’s blood for the virus.
The emergency declaration was, in the estimation of international scientists, long overdue, coming six weeks after the WHO had already declared the virus to be a global public health emergency.
Americans around the country would soon enter lockdowns. It was a fearful and painful moment, but also one where the damage from previous inaction was not yet set, said Ranney, the doctor and professor. She said that the federal government could have attempted to catch up on infrastructures for testing, contact tracing, and distributing PPE.
“But we didn’t,” she said.
Easter: 27,342 deaths
On a Monday in early March, the Rev. Jeffery Pate was on his way into the Ochsner Medical Center in New Orleans, where he is staff chaplain, when he encountered another chaplain on his way out.
“You look like you’ve seen a ghost,” Pate said.
After he scrubbed up and entered the intensive care unit, Pate saw why.
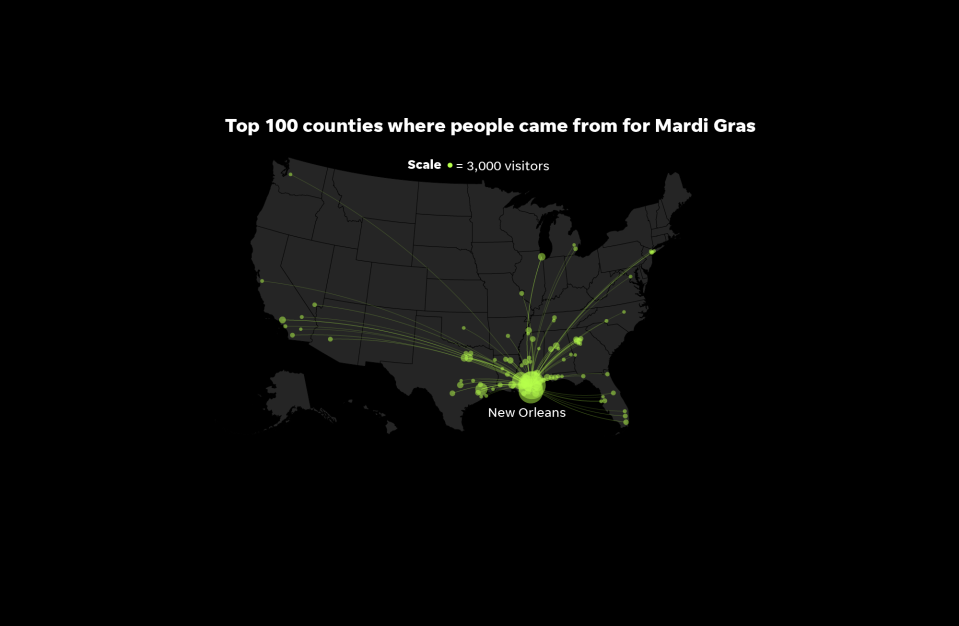
About two weeks had passed since a Mardi Gras celebration attracted revelers to the streets of New Orleans.
They came from virtually every corner of the country, including tens of thousands each from Texas, Mississippi and Florida.

The city had made no apparent attempt to curtail the festivities, with a top city health official assuring community health providers: “The chances of us getting someone with coronavirus is low.”
Fifteen days after the festivities ended, Louisiana confirmed its first five coronavirus cases, according to data from Johns Hopkins University. Cases surged to more than 5,000 at the end of March.
In New Orleans, Pate witnessed the sudden impact on the ICU, which had been mostly calm when he left work on Friday evening. Now, it was in chaos. Nurses scrambled between rooms to address a packed house of patients, most if not all of them on pumping ventilators.
Pate is on the hospital’s payroll to deal with what he calls the “why questions,” as in: Why has my higher power forsaken me? As he makes the rounds, he hunts for patients who look like they’ve lost hope or are filled with anxiety, and tries to talk them toward spiritual peace.
Pate and his colleagues thought that their experience during Hurricane Katrina prepared them for a major disaster.
But over the next month, Pate realized they weren't ready for the unrelenting nature of a deadly viral outbreak. It felt like a hurricane was slamming their ICU every day.
Pate struggled to combat the loneliness of a COVID-19 death. The hospital had a policy that nobody besides doctors and nurses were allowed into the rooms of those infected with the novel coronavirus.
One infected patient wanted to be baptized before he was put on a ventilator. Pate negotiated with a nurse to sprinkle the patient’s forehead with a sterile solution while the chaplain recited the ceremony via a video call on a computer.
But such work-arounds had their limits, as evidenced by Pate’s journal entries at the time, which were increasingly despairing.
March 20:
Today a daughter and her aunt and I stood outside the patient's room. The aunt asked me to pray over the body. Did she mean in the room? I told her I could pray outside the room with them. Was that disappointment I saw in her eyes?
April 1:
I already feel like I’m not making much of [a] difference in the hospital. We’re rubbed thin.

COVID-19 cases in Pate’s jurisdiction peaked in early- to mid-April, with nearly 900 in a single day on April 2 in Orleans Parish. The highest death count came two weeks later, with 32 on April 14.
As was the case elsewhere, it wasn’t just confirmed COVID-19 cases that spiked. Pate observed firsthand the phenomenon of excess deaths, mortalities which were not directly attributed to the virus but may have stemmed from it.
Pate recalled the brutal shift in which he handled the deaths or impending deaths of a newborn baby, a stillborn, an adult, and an elderly person. In an interview months later, Pate began to tally up all of the deaths he personally tended to in the first half of 2020.
"Yeah, we don’t disclose numbers,” interrupted a hospital publicist, who was present for the interview.
"Of what?” the chaplain asked her.
"Of deaths,” the publicist said.
"Well, we had a lot,” Pate responded, his voice breaking. “For me."
***
On March 17, two men hustled into a nearly-empty rest stop in Maryland. Four hours into their 1,200-mile drive from New York to Florida, they realized they weren’t going to make it on sandwiches and PowerBars alone, and stopped to fortify with Wendy's cheeseburgers.
One of the men was middle-aged and svelte. The other was more than two decades older, hobbled but still sprightly, with an oxygen tank piped to his nose and slung over his shoulder like a school bag. They wore face masks weeks before the CDC recommended them, and latex gloves.

As they exited the rest stop for the highway, Tom Kirdahy, then 56, and Terrence McNally, 81, felt safer with each mile they put between themselves and New York. It was as if they could feel the virus receding behind them.
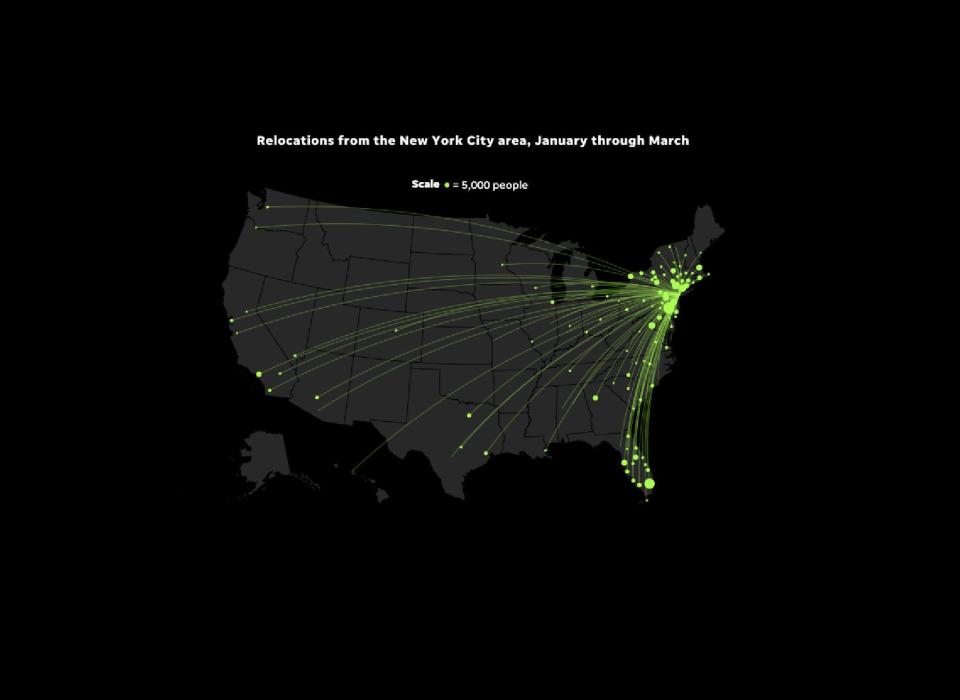
They were near the front of a great informal migration southward from the New York City area.
While other countries instituted national lockdown orders to freeze citizens and the virus in place, the United States had only localized, and relatively lax, versions of such edicts. Americans responded by moving more than ever.
McNally fled New York with husband Kirdahy because he had only three-quarters of a lung left and was terrified the virus would make quick work of him.
The couple’s history together had another pandemic as a backdrop. In 1995, Kirdahy, an attorney representing those infected with HIV and AIDS, was transfixed in a Broadway theater as he watched a gay male character kiss a purple scar on the chest of another.
In Kirdahy’s view, society had decided that eradicating the AIDS epidemic was not a priority because those it was killing, mostly gay men, were considered no great loss.
He had held the hands of many gay men as they died without the presence of family members who were afraid of infection or disdainful of their sexuality.
So attending “Love! Valour! Compassion!” written by McNally, whom Kirdahy then only knew as a famed playwright, was “like being in church,” he said.
It was the story of eight gay men on vacation together, including one, played by Nathan Lane, who kissed the AIDS lesion of another. Kirdahy and his companions at the theater, all of whom worked on the AIDS front lines or were infected with the virus, wept and hugged each other.
Kirdahy, a lifelong theater buff, met McNally six years later after inviting him to join a panel of famed gay playwrights he organized in the Hamptons, New York. They bonded over a shared familiarity with AIDS. Two of McNally’s previous partners had died of the virus, and the playwright had seen firsthand the isolation suffered by its victims in their last moments.
They married in 2003, with Kirdahy warning that he wasn’t going to shelve his ambition and become “Mrs. McNally.” He ultimately left his law practice to become one of the most prolific theater producers on Broadway and London’s West End, racking up armfuls of theater awards to rival those of his husband.

But a diagnosis only months after they had started dating injected their relationship with a perpetually fleeting quality. McNally’s former three-pack-a-day smoking habit had stricken him with lung cancer. Surgery left him with a quarter of his right lung and only half of his left. For decades he was in and out of the hospital, including with potentially life-ending bouts of pneumonia.
McNally made light of it. When he and Kirdahy bought a vacation apartment in Sarasota, Florida, in 2017, McNally predicted he would die there. “I know how this story ends,” he joked.
And in June 2019, when he was awarded a Tony for lifetime achievement, he accepted it with his oxygen tank attached and told the crowd: “Not a moment too soon.”
Despite his gallows humor, McNally was afraid of death, particularly the prospect that it might take him alone. Even before his lung cancer diagnosis, he had poured that fear into his writing of “Love! Valour! Compassion!”
In it, Lane’s character, who is HIV-positive, begs a friend: “Can you promise me you’ll be holding my hand when I let go?” Over the years, Kirdahy had many times made a similar promise to McNally.
During the first weeks of March, when it became clear that New York City was usurping the Seattle area as a national epicenter of coronavirus, they made hasty plans to drive to the apartment in Florida until its spread blew over.

At a roadside motel room in North Carolina, they napalmed every surface with Clorox and Lysol. In Georgia the next day, lunch was sandwiches handed off between latex-covered fingers at a Starbucks drive-through.
By dusk on the 18th, they were on their balcony rocking chairs in Sarasota, watching the sky turn a bruised pink over the Gulf of Mexico. McNally’s health had worsened, as he had grown weaker and short of breath. But he preferred sipping seltzer with his husband than more time in a hospital.
On the evening of March 20, McNally said, for the first time in their relationship: “I want to talk about dying.”
What followed was a long conversation, ranging from nuts-and-bolts estate planning to spiritual matters.
“We talked about family and friends and art and nature and gratitude,” Kirdahy said. “A lot about gratitude.”
At 9:21 the next morning, Kirdahy called 911 to report that his husband was coughing up blood.
***
Five days before Kirdahy's 911 call, Cookie Dungill called Sevil from his Chicago hospital room with a sudden concern.
Cookie couldn’t remember if he had paid his bills that month. He asked his son to head over to his house and make sure he was up to date on his gas and lights.
Sevil had for the last week been suffering an odyssey of severe symptoms from his own bout of COVID-19. He isolated on the first floor of his home, wearing a mask and leaving the second floor to his teenage son and wife, who brought him trays of food and stayed six feet away.
He had pneumonia, diarrhea and such severe night sweats that he had to get up in the middle of the night to change his soaked shirt.
But because he didn’t want his dad to worry about his own poor health, he agreed to check on his bills. He dragged himself out to his car, made it to his father’s house and slumped in front of the computer with Cookie on the phone.
It took them 2½ hours to puzzle through usernames and passwords to ascertain that Cookie had in fact paid his bills before he was hospitalized. They wheezed with laughter at their own ineptitude.
“Dad, don’t worry,” Sevil said. “We’re going to make it.”
Cookie called again a few days later, but this time his son couldn’t pick up. He was on the other line with an official from the CDC, who was pumping him with detailed questions about his movements and interactions in the previous two weeks.
The official wanted to know everything about the pizza dinner Sevil shared with his friend. He wanted to know who was in what rooms of the church the next day, who shook hands and hugged, and who ate from the buffet.
The health agency was following a cluster of Chicago cases that hinged on a single event: Angeli’s Joyous Celebration. The CDC was in the midst of declaring it one of the country’s earliest and most severe coronavirus spreading events, likely infecting at least 16 people.
And at its center was a single individual, Sevil’s friend, whom the CDC believed had brought the virus from Arizona. The friend had gone to a birthday party a few days after the funeral and apparently spread the virus to family members, according to the CDC. The virus then spread further when those family members went to sermon at a packed church, complete with a collection plate as a possible vector.
Even without the call from the health official, Sevil's vicinity to the epicenter of the spread of the virus in Chicago was already clear to him.
On March 16, his friend’s sister died. A warm, boisterous woman known for singing in church, she was the first official novel coronavirus death in Illinois. His friend lost another sister to the virus less than two weeks later.

When Sevil got off the phone with the contact tracer, he went to call Cookie back at the hospital. But his father was by then unconscious, having been put on a ventilator.
Sevil later learned from his sister Gina the words that were among his last.
Cookie had called her to say the hospital staff was urging him to go on the ventilator not because he needed it yet, but because he was experiencing labored breathing and the staff didn’t want to have run out of them when he did need one.
It was a reasoning common earlier in the pandemic that medical experts now regret, following studies showing that ventilators were overused and might have contributed to a higher death rate.
Gina encouraged him to follow the doctors’ recommendations, optimistic that it would help him recover. Though he agreed, she later said she could hear the fear in his voice.
“I don’t want to die,” he told her.
***
USA TODAY shared with Ranney, the emergency physician and Brown University professor, the stories of both the Dungills in Chicago and the ailing playwright McNally’s sojourn to Florida.
Ranney said that the thread that ran through both of their cases was that they had been failed by the government. A dearth of testing, medical equipment, and sound scientific guidance had abandoned them, like thousands of other Americans, to fumble alone through infection with a deadly virus.
Even if the government had handled the pandemic well, Ranney said, the virus still would have ripped a deadly course through the country.
“But it would’ve provided guidance to people like that man on what to do,” she said, referring to McNally. “It would have allowed him to get a test. And it would have kept people from having that abject fear that led them to flee, and to bring the virus with them."
After his husband, Kirdahy, called 911 to report that he was coughing up blood, McNally was taken to a Sarasota hospital. He was isolated and, within a couple of days, put on a ventilator. After a COVID-19 test came back positive and his oxygen levels dipped dangerously, Kirdahy made the decision to take him off of the ventilator.
Kirdahy’s promise to his husband that he’d be holding his hand while he died weighed heavily on him. He asked the doctors whether he could enter his hospital room, and they allowed him.
“I’m one of the lucky ones,” Kirdahy said of being able to say goodbye. He would later test positive for virus antibodies, suggesting he was an asymptomatic carrier.
Wearing scrubs, gloves and a mask, Kirdahy sat by his husband’s bedside. He played their song, Ella Fitzgerald’s “Always,” and then a couple of songs by Maria Callas, McNally’s favorite opera singer.
Kirdahy had texted an update to McNally’s circle of theater colleagues, who the playwright always referred to as his surrogate family, and was comforted that around the country those actors, producers, directors and crew members were playing Callas, too.
He thought of his promise. “Honey, squeeze my hand,” Kirdahy said. “Tell me you know I’m here.”
He felt the hand wrapped around his tighten hard.
Independence Day: 130,127 deaths
There was a window of opportunity in early spring — before Americans were dug intractably into separate trenches, before wearing a face mask had somehow become a defining political issue, and militia members were caught allegedly plotting to kidnap the Michigan governor over lockdown orders — when the country could have unified in order to beat back the virus.
“People were willing to listen to public health officials, and they were willing to take precautions,” Ranney said. “We squandered that.”
Part of the problem was the contradictory messages coming from government officials. The CDC recommended masks in early spring after months of advising against them, and elected leaders clashed over state and local rules — like whether to close Georgia's beaches — in the absence of a clear national edict.
Such at-odds approaches made it feel like safety measures were the whims of public officials, often determined by their political alignment.
The deepening political entrenchment was led by the president. Trump mocked face coverings even after his government recommended them. He publicly undermined Dr. Anthony Fauci, the government's top infectious disease expert. He called COVID-19 the “China virus” in spite of increased attacks against Asian Americans. And he made an axiom of declaring that the cure — lockdowns recommended by top members of his own national health team — was worse than the virus itself.

The division thrust into the spotlight government doctors, the kind of career public servants whose names the average constituent might never otherwise learn.
Scott Harris, Alabama’s state health officer, said he decided to go into public health after two decades in his private practice in Decatur observing how illnesses hit his Black patients harder.
“If public health exists for one reason it’s to promote health equity,” said Harris, a soft-spoken physician who wears black-rimmed glasses and often reads from a yellow notepad.
Harris encountered the politicization immediately after his state had its first official case, on March 13. Alabamians in his inbox challenged his counting of “presumed” cases, which follow a positive test, versus cases that the CDC reviewed and confirmed.
Later that month, Harris’s staff debated how to classify one of the state’s first deaths involving a positive test for COVID-19. The decedent was a young person who had a stroke while infected with the virus. In a deeply-red state under a Republican governor, Kay Ivey, Harris said his staff ultimately reported it as "death by stroke, in a person who also had Covid."
"And then, within a couple months, it became clear that’s one way people with COVID die," Harris later said.
“At that time there was all this pressure — well still is, this pressure,” Harris said. “These pressures to minimize what’s actually going on, and people were hyper-alert to try to make sure we counted our cases correctly.”
The hostility continued after the governor issued a stay-at-home order on April 3, in response to a crisis of overwhelmed hospital beds, infected health-care workers and a rising death count in nursing homes.
Emailers lectured him on states’ rights and personal liberty, and sent Benjamin Franklin’s Revolutionary War cartoon reading, “Join, or Die.” Even when email called him a dictator, Harris looked to see if they contained legitimate questions, and forwarded those messages to his staff so the experts could educate them.

Others explicitly threatened him. “I’m going to show up at your house, and you better watch out because I know where you live,” one person wrote.
The state gave Harris an around-the-clock security detail and a ballistic vest. They told him to fling it on and lock his door if he heard a loud noise.
Harris’s experiences were not unique: State health officers around the country experienced similar treatment, with hundreds facing threats or resigning.
***
On APRIL 28, Harris shared a stage with Ivey as the governor announced she was significantly scaling back her safety order and would reopen office buildings, retail stores and beaches.
“I want to go on the record that I said to Dr. Harris that, in my opinion, hairstylists, or at least mine, are essential to the function in the state government,” Ivey joked.
Ivey’s change in policy made Alabama one of the first states to lift restrictions following encouragement from Trump, who by mid-April had called for states to reopen their economies.
After the Alabama governor gave up the lectern to Harris, he struck a markedly different tone. His mask down around his chin, Harris spoke soberly about data emerging in Alabama, as it was throughout the country, that showed that the virus disproportionately impacted Black and Hispanic Americans. Black Alabamians represented a quarter of the state but half of its COVID-19 deaths to that point.
The decision to reopen most of Alabama may have been welcome to many residents, including business owners. To Linda Gilchrist, a nurse who works at a Montgomery senior home, it was devastating. After finishing a shift — followed by a lengthy clothes-washing and showering routine so as to not infect her family — she caught Ivey’s press conference on television.

Dozens of Gilchrist’s patients had died from the virus, and she had stood in a meeting that day where stakeholders discussed getting more patients into the rehab unit. In Montgomery, coronavirus cases had been steadily rising. Ivey’s policy change certainly wasn’t based on the state having flattened the curve.
“Oh my God,” Gilchrist thought to herself. “Why are we doing this?”
William Boyd, a lifelong resident of deeply segregated, majority-Black Montgomery, thought he had an explanation. Boyd had lost six relatives or close friends to the virus, including his brother. He saw the growing apathy toward the virus in Alabama as a result of policy-makers learning that Black people were most vulnerable. The CDC had just come out with that information on April 8.
DEADLY DISCRIMINATION: America’s history of racism was a preexisting condition for COVID-19
The hospital where Boyd’s brother died had a policy allowing loved ones access if they were near death, and he described sharing a waiting area with those who were about to say goodbye to a patient. “It was an ugly sight, and I saw all Black people,” Boyd said.
Boyd addressed the Montgomery City Council in June when they considered a mask mandate. “The question on the table is whether Black lives matter,” he said. The mandate failed after the eight-member council voted mostly along racial lines, Black members for the mandate and white members against it.
The next month, the Montgomery council members reversed themselves and passed the mandate. Ivey also revisited the statewide mask issue during another press conference, roughly six weeks after the one where she'd cracked the joke about her hairdresser. Harris was back at her side.
“We are almost to the point where our hospital ICUs are overwhelmed,” Ivey acknowledged in ordering a statewide mask mandate. “Folks, the numbers just do not lie.”
Cases in Alabama had more than doubled in the month before the announcement, to more than 60,000, adding more than 1,100 cases per day on average.
When Harris returned to his desk from the press conference, he watched his inbox fill up with vitriol.
How the South and Southwest became the global epicenter of the COVID-19 pandemic
***
The unique rub of the novel coronAvirus is that attempts to defeat it tend to open up another front of misery.
Extended lockdowns deliver their own world of grief, as the millions of newly unemployed Americans can attest. The tug-of-war between industry and public health has often resulted in public policy that keeps the economy afloat at the expense of the health, and often lives, of those with the least agency.
Nowhere has that been more clear than in the federal government’s handling of the meatpacking crisis.
In mid-April, Minnesota hog farmer Greg Boerboom heard from a representative of Smithfield Foods that the meat conglomerate had to delay its weekly purchase of several semi loads of his animals due to illness at the company’s Sioux Falls plant.

But Boerboom wasn’t worried the disruption would extend any longer than a few days. The meat industry had eradicated uncertainty a long time ago. Boerboom contracts with the few multinational corporations that control the meat processing industry. It’s a departure from the system he learned as a young man on his father’s farm, where they’d haul 30 hogs at a time behind their ‘59 Chevrolet three hours away to the stockyards in St. Paul to search for buyers.
Critics deride the ruthless efficiency of the business but Boerboom, 59, sees progress. “We can glamorize the good old days,” he said, “but the fact of the matter is they weren’t that glamorous.”
But the drawbacks of the modern meatpacking model began to show when a representative for Tyson Foods also called Boerboom to say COVID-19 cases were forcing the temporary closure of the company’s plant in Waterloo, Iowa.
The two plants represented roughly 60% of Boerboom’s business. And as a month came and went, and the plants remained closed, his stock of roughly 100,000 overgrown hogs crowded against each other in his barns. Boerboom had to consider ways to quickly reduce his inventory, including whether to execute a large number of them with a handgun.

His colleagues were doing it, those who weren’t pumping carbon monoxide into their barns to kill thousands of their hogs. All across the country, hog farmers faced the same grim scenario.
But Boerboom couldn’t stomach the idea of wasting the animals. He slashed his prices, offering to sell his hogs to local buyers for $40 a head, a $100 loss on each. Deer hunters left with live hogs in the beds of their pickups. Members of Minnesota’s sizeable Hmong community, from Southeast Asia, pulled up to the farm and popped car trunks. One diehard drove from outside Seattle, a 3,000-mile round-trip, to load 10 of Boerboom’s hogs into a horse trailer. Mennonites made three trips from Pennsylvania with a semitrailer.
As his business hemorrhaged money, Boerboom said he didn’t blame the meatpacking corporations. Instead, Boerboom, who says he speaks for many of his colleagues, blamed those line workers at the meat plants, or more precisely, the labor organizers he said were overstating the danger the workers faced.
“They were given bad information” about the risks of the novel coronavirus, Boerboom said. “That it was going to be a death sentence.”
***
IT WAS A KNIFE of the same sort she had used for the past 15 years to carve hams out of their fatty exteriors. Perpetually dull, with a blade a little longer than a dollar bill. But Sandra Sibert found she suddenly couldn’t lift it.
On April 7, Sibert manned the hambone table at the Sioux Falls Smithfield Foods plant. Sibert had logged thousands of hours there, a sometimes overwhelming station where the hunks of meat and bone came so fast her hands would swell.
But now she experienced a weakness like she hadn’t felt since giving birth. She was hit by a chill, and then a surge of heat. She coughed and sneezed and fought for breath.
A co-worker gave her a knowing, alarmed look. Gossiped information about the symptoms, and how quickly they could lead to worse, had been flying on the meat line.
Sibert found a supervisor and asked if she could leave her post: “Please, I can’t breathe.”

Sibert later recounted that the supervisor brusquely denied her, explaining that they’d already sent home 38 workers that day.
Sibert attempted to return to the hambones. She mostly focused on staying conscious.
A co-worker’s voice — “Sandra, you OK?” — brought the realization that she wasn't at the hambone line but was now by the employee lockers.
“Don’t come over here,” she warned.
Then she was outside, fumbling for her phone to call her husband, James. Then in his car, at a drive-up test site.
Then, results: COVID-19 positive.
Sibert left Honduras for the United States three decades earlier and has spent 15 years in South Dakota, all of it working on the line at Smithfield. She clocked nine hours a day, six days a week, for $17.10 an hour, and became a union steward. A few years back, the mother of five had contracted breast cancer. "But God still loves me and left me here,” she said.
She pictured it all now coming to a quick and unceremonious end. I’m going to die, she thought. I’m going to die and leave my babies.
***
In a video statement the previous month, Smithfield CEO Ken Sullivan had stressed the essential nature of his employees. “Food, after all, does not get made on the internet,” he said, and assured consumers there was “no evidence that COVID-19 can be transmitted by food.”
A month later, and five days after Sibert got her test results, Smithfield closed its Sioux Falls plant. More than 230 workers had tested positive.
The meat may have been safe, but Sibert and many other line workers felt far from secure processing it. She had since March tried to get her supervisors to make face masks mandatory and to put distance between workers on the line. But health measures had ranged from lax to non-existent even as dozens of her colleagues fell ill.
She and her colleagues, most of whom were also immigrants, would turn to prayer at lunch or while sharpening their knives. Sometimes they couldn’t hold back tears on the meat line. They prayed for their sick colleagues to recover and come back. A few never did.
Even before she got sick, Sandra had been isolating at home from James and their two youngest daughters, Devorah and Valeriah. When she came home, she threw her clothes in the washer, showered and hid in her room.
If she left the bedroom to use the bathroom, she wore a mask. If her husband wanted to talk, he called her.
For the month after she stumbled out of the meatpacking plant, stricken by COVID-19, she was bedridden, barely able to muster the strength to walk to the bathroom and then bleach the toilet and sink before she left.
Not hungry for three weeks, she drank cupfuls of tea with honey and prayed.
She did not kiss her daughters. They did not get sick.
One of her older children came to visit but could only talk through the window. Sandra peered through the glass, feeling like an alien. Her son broke down: “I don’t want to let you die.”
When she saw on the local news on April 28 that Trump had signed an executive order compelling meat processing plants to stay open during the pandemic, she cried. She felt Smithfield wasn’t safe, and that the president made the wrong call.
She reported back to work on May 8, her symptoms finally having abated. Her co-workers who had hugged her when she returned from cancer now mostly kept their distance.
More than 800 workers at the plant had tested positive.
Sibert said some workers and supervisors still refused to wear masks and face shields correctly. Smithfield's policy is to notify all employees who were in close contact with somebody who caught the virus, but Sibert said that didn't always happen.
“Keeping a secret like that — it’s not safe,” Sibert said.
Smithfield declined to comment directly on Sibert's allegations. They instead sent statements, including one they said was from one of Sandra’s colleagues, asserting “there is no place we feel safer” in Sioux Falls than the plant.
***
The virus had forced farmer Greg Boerboom to revert to his dad’s old way of doing business, selling a few hogs here or there and stocking the butcher shops on nearby Main Streets. But Boerboom isn’t the nostalgic type. When the Smithfield and Tyson buyers returned in late May, he rejoiced and credited Trump’s executive order.
The order was a boon for those major corporations, which as it turns out were never at risk for a severe meat shortage. In fact, a significant portion of the hogs Boerboom sold to Smithfield and Tyson likely ended up not in American kitchens, but in Chinese ones.
Market data showed that during the period when meatpacking executives were warning that the food supply chain was breaking, they were exporting millions of tons of meat overseas – even more than in previous years.
How a third wave of COVID-19 engulfed the US
The federal government had prioritized the production of meat over the safety of low-paid, mostly-immigrant workers. In the months following Trump’s executive order, plant operators claimed to have implemented safety guards such as plexiglass barriers and mandatory masks. But there was little federal oversight monitoring those measures. COVID-19 cases in the plants skyrocketed, and often so did the case counts of their surrounding communities.
As of September, there would be more than 200 deaths among meatpacking workers who had contracted the virus.
Boerboom thinks the media has mostly ignored the real story, which is post-traumatic stress and depression he predicts will linger with hog farmers. “The big story is going to be the financial and emotional drain to the farming community in small-town America,” he said.
But he says Trump deserves gratitude for returning the business to the status quo even in the midst of a pandemic. “I think that’s what saved our industry,” Boerboom said. “If he had not done that, we would be out of business today.”
Thanksgiving: 263,456 deaths
In early April, Gina Jere drove to a cremation center where a man in full protective gear dropped into her trunk a triple-bagged Hefty containing Cookie Dungill's watch, glasses, cell phone and a container of his ashes.
When her brother Sevil Dungill learned that their father had died, he was still in the throes of his own severe sickness, isolated on the first floor of his house.
He kept six feet away as he told his teenage son about Cookie’s passing.
“We’re not going to grieve right now,” said Dungill, who was terrified of infecting his wife and son. “Because grieving makes you weak.”
Dungill finally left his home after nearly two months of sickness in isolation. He emerged to a changed world full of face masks and strange new rituals at the supermarket. Protests and riots then followed and brought shattered storefronts to his Chicago neighborhood.
“You just want to wish it away,” he said of the events of 2020.
Like other families that have lost loved ones this year, it's hard to predict when, if ever, the Dungills will be able to properly grieve. There was no funeral or memorial for Cookie Dungill and, considering the results of the family’s last gathering to mark a death, there probably never will be.
For Sevil Dungill, the lack of closure concerning his father’s death has also consumed his perspective on the other family members he lost in 2020. Like Darryl Ospring’s fixation on her mother’s January death in the Bay Area, Dungill suspects that COVID-19 was responsible for the deaths of his sister in January and his mother in February.
Before his family’s saga with the illness, he accepted without doubt that their deaths were a result of cancer.
But he has since thought back on their sudden declines. His sister Angeli was put under a hospital ventilator before dying, according to her death certificate, of acute respiratory distress syndrome, pneumonia and metastatic lung cancer. His mother’s official cause of death was aspiration pneumonia and congestive heart failure.
The lung-related conditions are hallmarks of COVID-19 deaths. But Dungill will never know for sure, since both women were cremated and not autopsied. Jere and Demus, Angeli's husband, don’t share his determination that they died of the novel coronavirus.
At least in Barbara Dungill's case, it’s an uncertainty that, like much of the story of the nation's early outbreak, would’ve been prevented by readily accessible testing early on.
The Dungills got one of the earliest tastes in the United States of the devastation of COVID-19. They thought it would be under control by now. The three surviving siblings expected to come together for Thanksgiving to begin coping with life without their father, mother and sister.
Thanksgiving was Cookie’s favorite holiday, especially after he became his ailing wife’s caretaker and learned to cook for her. The menu was locked: Cookie would make the prime rib, ham, corn and green beans. Gina would bring the sweet potatoes, dressing, macaroni and cheese, rolls, turkey and a sugary fruit punch. Angeli was in charge of dessert. The surviving siblings planned to re-create the meal as best they could.
But instead of the virus being under control, case counts in Illinois and around the country instead reached grim new heights to kick off the holidays, resulting in lockdowns and a singular faith in the vaccine as our only hope.
For Gina, Thanksgiving became takeout at home and plans for a Zoom call with family that never came to fruition.
Gina, who Cookie called “Gee,” had a landline phone that only her father ever still used. It rang several times in the months following his death.
Momentarily forgetting, she expected to pick up and hear his usual schtick, which was boasting of some dish he had made for her mom that night: Gee, I fixed some pork chops. Oh my God, they were perfect. … Gee, I fixed this steak. It was so tender.
But it was always telemarketers. Eventually Gina yanked the cord out of the wall.
Contributing: Matt Wynn, Dian Zhang and Brett Murphy
How we did it
USA TODAY reporters used a variety of data sources for the "American Virus” story. The following lists each source in the order that each graphic appears:
People traveled from Wuhan: VariFlight provided data for flight CZ2659 from Wuhan to San Francisco with flight dates and occupancy rate. USA TODAY extrapolated the population of each flight based on the capacity of the Boeing B777-300ER, the plane used by China Southern Airlines.
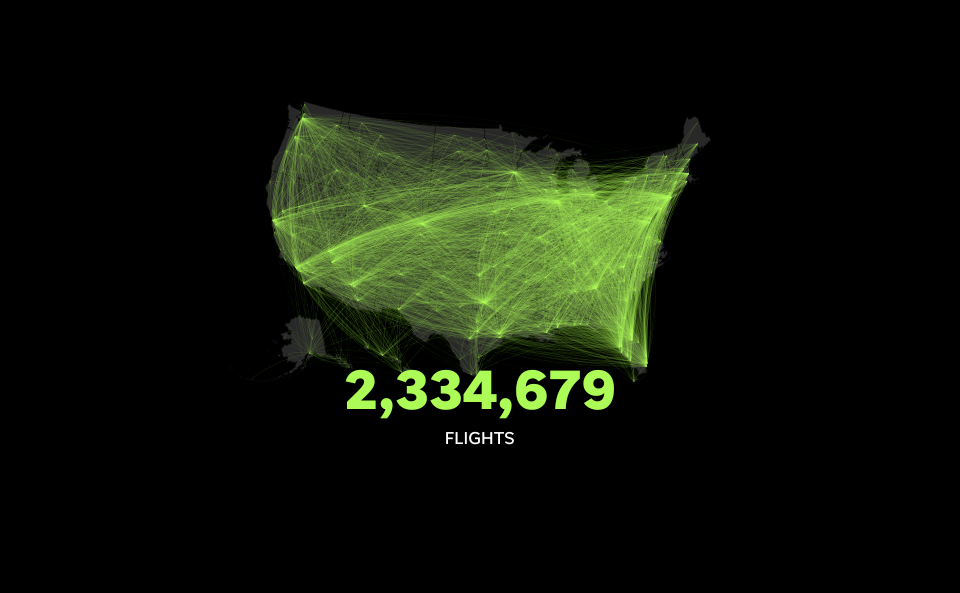
International and domestic flights: Flightradar24 provided daily flight data from Jan. 1 to April 30. USA TODAY removed flights with unknown or unconfirmed departures or arrivals from the final count. Then, reporters counted the flight routes and analyzed them using the provided 3-letter IATA airport code.
NFC game: Cuebiq provided data that tracks movement of cell phone devices. Devices used in this analysis were present at Levi’s Stadium in Santa Clara County from Jan. 20 to Jan. 26. Cuebiq provided the top 100 counties of origin. USA TODAY extrapolated population numbers using data from the U.S. Census Bureau.
Bay Area deaths: USA TODAY obtained death records for these cases under the California Public Records Act from the Santa Clara County Medical Examiner.
Death counts in headers: USA TODAY used data from Johns Hopkins University that includes all 50 states, the District of Columbia and territories.
Mardi Gras: Cuebiq provided location data from cell phones in New Orleans’ French Quarter between Feb. 17 and March 1. Cuebiq provided the top 100 counties. USA TODAY extrapolated population numbers using data from the U.S. Census Bureau.
New York State population change: This is based on Cuebiq’s “home-switcher” data that uses cell phone devices to determine who changed homes, in what location, and when. Cuebiq provided the data broken down by the balance of population in the state. USA TODAY extrapolated population numbers using data from the U.S. Census Bureau.
New York State relocation destinations: This also uses Cuebiq’s “home-switcher” data. Cuebiq provided the data by week for all states. USA TODAY cut the data to observe only New York State from Jan. 1 through March 31 and extrapolated population numbers using U.S. Census Bureau data.
New York City relocation destinations: This also uses Cuebiq’s “home-switcher” data. Cuebiq provided the data broken down by week for Census-designated metropolitan areas. USA TODAY cut the data to observe only the New York City area from Jan. 1 through March 31 and extrapolated population numbers using U.S. Census Bureau data.
Florida deaths related to travel: USA TODAY obtained medical examiner data under state public records law. The deaths span from March 5 to April 14.
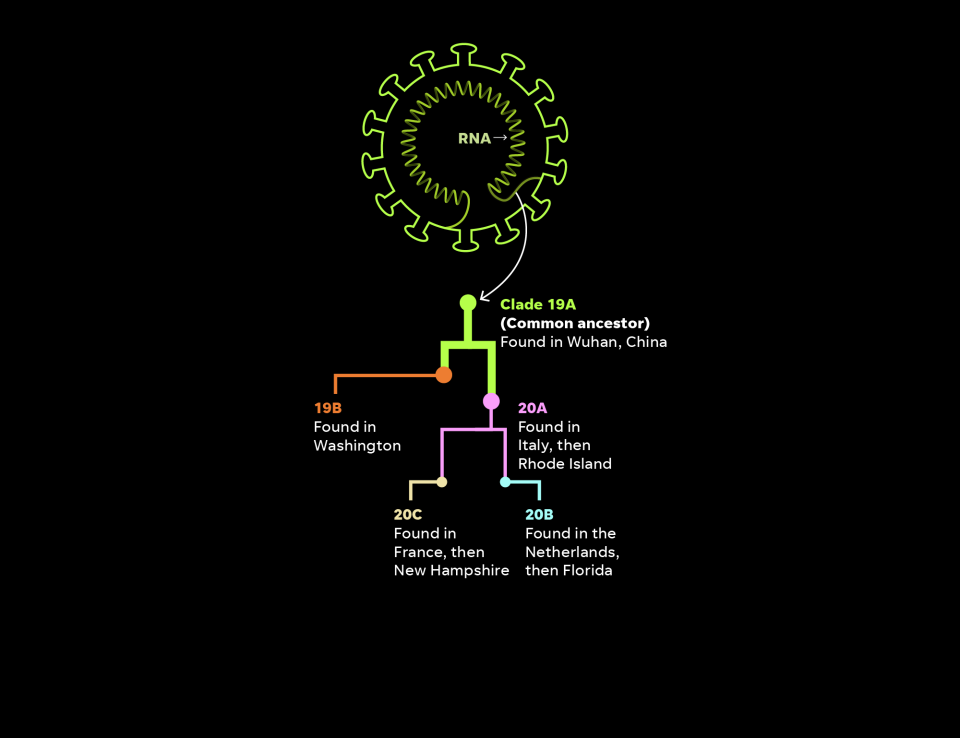
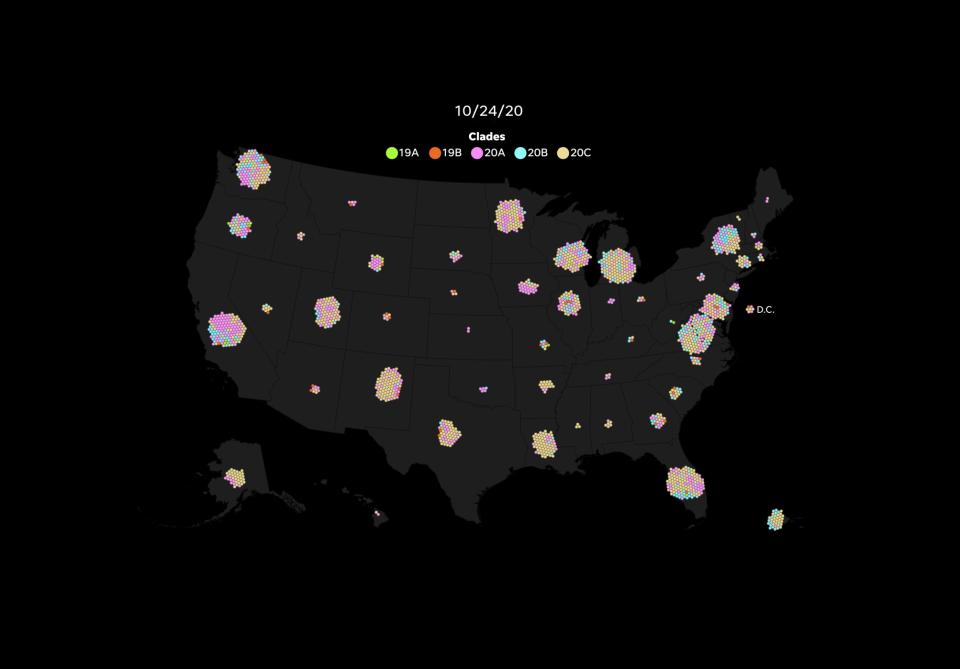
Clades: Starting in May, USA TODAY periodically downloaded data on NextStrain.org that originates from the international repository GISAID. The graphic depends on NextStrain’s build of cases in North America from Nov. 17 that USA TODAY filtered to include only cases in the United States. Early cases are cross-referenced with news reports to provide additional information. Clades reflect NextStrain methodology as of November.
The team behind this story
REPORTING AND ANALYSIS: Gus Garcia-Roberts, Erin Mansfield, Caroline Anders, Matt Wynn, Dian Zhang, Brett Murphy
EDITING: Chris Davis, Matt Doig, Kelley French
GRAPHICS AND ILLUSTRATIONS: Ramon Padilla, Mitchell Thorson, Shawn Sullivan, Javier Zarracina, Karina Zaiets
PHOTOGRAPHY: Emily Johnson
COPY EDITING: Melissa Galbraith
DIGITAL PRODUCTION AND DEVELOPMENT: Andrea Brunty, Annette Meade
SOCIAL MEDIA ENGAGEMENT AND PROMOTION: Mary Bowerman
This article originally appeared on USA TODAY: How US failed to meet the challenge of COVID-19

