Monkeypox in Kids: What Parents Should Know
The monkeypox outbreak in the United States appears to be slowing down, but numerous states have reported cases of monkeypox in kids, from New York to Oregon, Texas, Maine, Florida, Indiana, California and Washington, D.C.
According to the latest demographic data from the Centers for Disease Control and Prevention, at least 42 kids between 0 and 15 years old have been diagnosed with monkeypox in the U.S.
Monkeypox cases in the United States overall have surpassed 26,000, but the number of new cases per day recently are much lower than they were in July, August and most of September. On Oct. 5, there were 60 new cases reported, compared to 688 cases on Aug. 15. That said, people of color are still being disproportionately affected by the outbreak, with Black and Hispanic patients making up 68% of cases.
RELATED: As monkeypox outbreak spreads, these pictures can help you identify symptoms
The decrease in new cases is likely due to vaccines and at-risk communities changing their behavior due to growing awareness of how monkeypox spreads. The majority of cases have been reported in men who have sex with men, with sexual activity driving most of the cases. But the virus can also spread outside of sexual encounters; for example, in previous monkeypox outbreaks, the virus has spread among people living in the same household.
Numerous cases have been reported outside of the LGBTQ community, as well. For example, there have been over 500 cases in cisgender women, according to CDC data.
“The CDC has emphasized that monkeypox can affect anyone who has close contact with people who have monkeypox, and this includes children,” CDC spokesperson Kristen Nordlund told TODAY in an email.
What is the risk for monkeypox in kids?
Parents who are especially worried because they live in an area where case numbers are higher — such as New York City, which has reported three cases of monkeypox in a minor — should be reassured because overall the number of cases of monkeypox in kids remains low, Nordlund said.
“Right now children make up a very small proportion of the overall number of monkeypox cases, of which there are over 6,000,” Nordlund said. “Data about infections in children are limited and the CDC is working to learn more.”
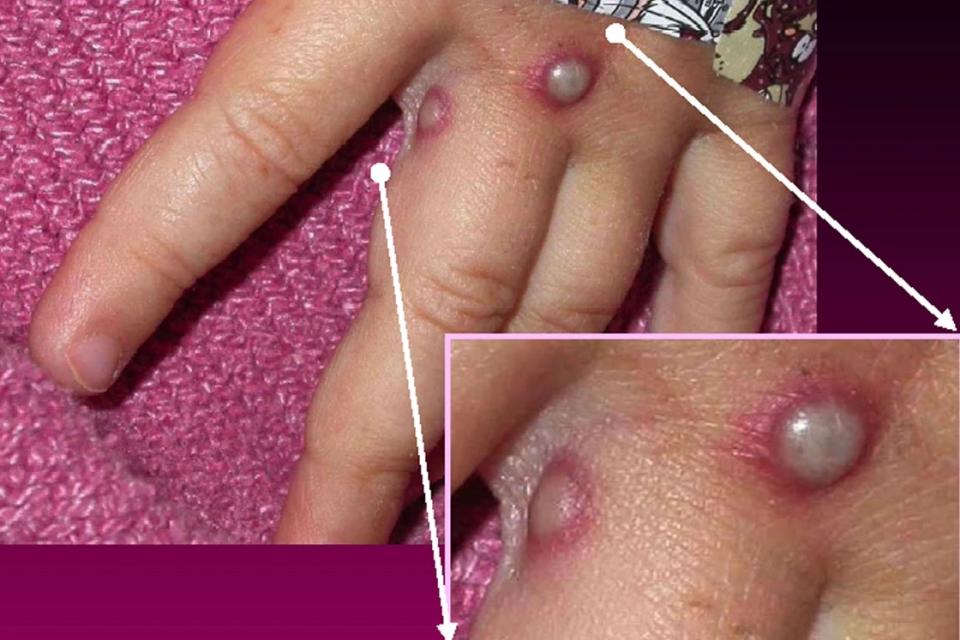
With the small number of infections reported in children as of early October, experts say parents shouldn’t be overly concerned about their kids catching the virus, unless they themselves have monkeypox, which they could easily spread to their children.
“Generally speaking, there isn’t much to worry about,” said Dr. Peter Hotez, co-director of the center for vaccine development at Texas Children’s Hospital and dean of the National School of Tropical Medicine at the Baylor College of Medicine. “I’m not worried about transmission in schools.”
Oregon health officials echoed this stance in a press release about the pediatric case. Dr. Dean Sidelinger said he believes the risk of monkeypox spreading in schools is low, as person-to-person transmission usually occurs from direct contact with a monkeypox rash, scabs or bodily fluids.
“Monkeypox is not COVID-19. This virus is not easily spread unless you have that prolonged, close, skin-to-skin contact with an infected person,” Sidelinger said.
But the risk of monkeypox for school children may change, Hotez said. “The trajectory has been going up pretty fast. If it continues to climb and the virus becomes more generalized among the population, that is a concern.”
The presence of monkeypox in wastewater suggests that the disease may be more spreading even faster than we think, Hotez said. Wastewater samples have come up positive for monkeypox in a number of locations, including the San Franciso Bay Area and southern Nevada. Other locations, including the Atlanta area and North Carolina, are beginning to check their wastewater.
While Hotez is not worried about kids in grade school, he is somewhat worried about college kids and those who live at boarding schools. “They live in such close quarters in dorms,” he said. “If it accelerates, there could be clusters.”
Some experts are recommending vaccination programs for colleges, Hotez said.
The people currently most likely to get monkeypox, per Nordlund, include:
Those who have been identified by public health officials as a contact of someone with monkeypox
People who are aware that one of their sexual partners in the past two weeks has been diagnosed with monkeypox
People who had multiple sexual partners in the past two weeks in an area with known monkeypox
People whose jobs may expose them to orthopoxviruses (the family of viruses that includes monkeypox and smallpox) such as laboratory workers and health care and public health workers
What are the common ways children may get monkeypox?
“Monkeypox spreads through close skin-to-skin contact, which, in the case of children, could include holding, cuddling, feeding, as well as through shared towels, bedding, cups and utensils,” Nordlund said. She added that the disease can also be transmitted to a fetus during pregnancy or to a newborn through close contact during and after birth.
Hotez pointed out that the virus can persist on surfaces, and those living with someone who has monkeypox need to be careful with bedding and other materials on which the virus might persist. He suggested that all potentially contaminated bedding, towels and clothing be washed in hot water and put through the dryer.
It’s really important to recognize that there have only been a few confirmed cases in children so far, and most if not all of those children had been in close contact with a known monkeypox case, said Dr. Buddy Creech, a pediatric infectious disease expert at the Vanderbilt Medical Center and director of the Vanderbilt Vaccine Research Program.
Keep in mind, Creech said, that the most likely scenario for children to get monkeypox is through sustained household exposure. “I can envision a father, a mother, a young adult or teen with monkeypox in the home,” he said. “Just like smallpox, it can be spread through respiratory droplets and contamination of surfaces, though it is not as contagious as smallpox.”
How does monkeypox affect children?
The kids who are at highest risk for severe disease are those who are under age 8, Creech said. “They tend to experience complications such as pneumonia and brain inflammation. The sores themselves can become infected and cause cellulitis and sepsis. The reason children are more likely to develop cellulitis and/or sepsis is that younger children have a harder time not scratching the lesions.”
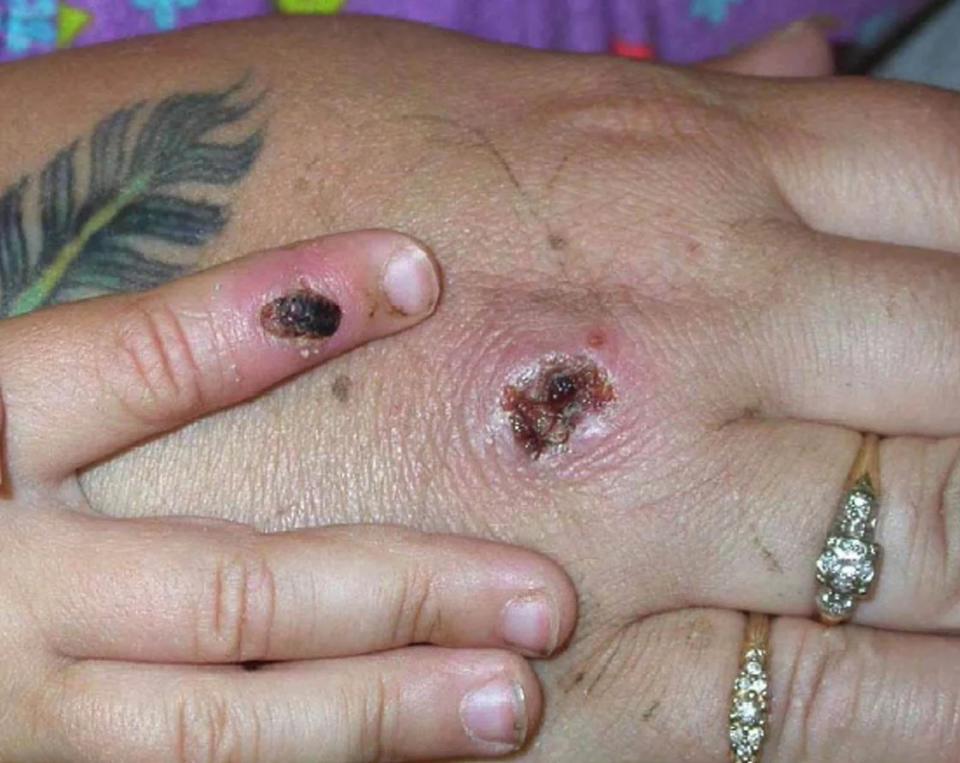
The lesions are often quite painful, Creech said. “They can be so painful that people sometimes need inpatient management of pain,” he added. “In children that becomes a real and heartbreaking challenge for us.”
The disease may not be as deadly as HIV, but nobody wants to experience that level of pain, Creech said. Moreover, it can cause significant scarring, he said. “Look at the older pictures of people who had smallpox,” Creech said. “Most people would want to avoid those scars.”
Both the monkeypox vaccine and an experimental treatment called TPOXX are now available for children under special expanded access protocols, according to Nordlund.
How can parents protect their kids from monkeypox?
“The number one thing parents can do to protect their children is to make sure they themselves do not get monkeypox,” Creech said. “That may mean abstaining from certain activities that place them at high risk and taking precautions they otherwise might not take.”
What it does not mean, Creech said, “is families isolating themselves and being fearful of casual exposures at restaurants or the mall or the grocery store. Casual exposures do not appear to be a leading risk factor. Rather, it’s sustained exposures in a household setting.”
The CDC recommendations for protecting yourself from monkeypox include:
Avoid skin-to-skin contact with people who have a rash that looks like or is confirmed monkeypox, including kissing, hugging, cuddling and sex.
Avoid contact with objects or materials that a person with monkeypox has used, such as utensils, cups, bedding, towels or clothing.
Practice good hand hygiene, especially before eating or touching your face and after using the bathroom.
Experts also advised that parents should be able to recognize the signs of monkeypox. In addition to a rash, symptoms may include fever, malaise, headache, sore throat, cough and swollen lymph nodes. (Not everyone in the current outbreak has developed such symptoms before the rash; some people get them after and others never do, NBC News reported.)
It’s important to recognize that sometimes “the lesions are not visible,” said Dr. Saad Omer, an infectious disease epidemiologist and director of the Yale Institute for Global Health. In other cases, there may be the beginnings of a lesion, but the person doesn’t recognize it as a sign of monkeypox because they don’t expect to have gotten it, Omer said.
Parents do need to keep track of what’s happening with the virus, he added. “They don’t need to obsessively pay attention to the news, but they can’t completely zone out,” he said.
The CDC cautions families in which a household member has been infected to avoid contact with that person, including their bodily fluids, bedding, towels and clothing. If contact with the infected person is necessary, the agency advises the infected family member wear a well-fitting mask or respirator as should the other people they're coming in contact with (except children under 2).
For children with monkeypox, the number of caregivers should be limited as much as possible, and caregivers should try to prevent them from scratching their lesions or touching their eyes. Caregivers should also cover areas of broken skin on the child with bandages when possible and avoid direct contact with the rash.
This article was originally published on TODAY.com

