No, COVID shots won’t give you shingles. Here’s what causes it, what you need to know
- Oops!Something went wrong.Please try again later.
Right before Memorial Day, Suzanne Forbes changed to a different fragrance of Tide laundry soap. So when she broke out into what looked like hives on her stomach and neck, she thought she was having an allergic reaction.
But the pain, oh the pain, told her something else was going on. She had shingles.
Running errands that Friday, “I started feeling kind of weird,” said Forbes, who is 51 and lives in Belton. “And by that afternoon, I literally had to hold my clothes off of my stomach because it burned, it hurt, it itched. It was the worst feeling in the world. I would not wish them on my enemy.”
For several days, she couldn’t sleep. “Every hour, you feel that stab and you’re up and you’re sweating because it hurts so bad and there’s just nothing you can do,” she said.

One in 3 Americans can feel her pain. That’s how many of us are likely to get shingles in our lifetime. If you had chickenpox when you were a child, the shingles virus — cue the ominous music — is inside your body, waiting to be triggered.
Shingles is common, but the pandemic has people asking new questions about it, especially about any possible connection with the COVID-19 vaccine.
Anecdotal reports have surfaced on social media about people getting shingles after getting the vaccine, touching off frenzied rounds of strangers diagnosing one another online.
“I read online there might be link to it … people who got shingles after (the) Covid vaccine,” one poster on Reddit wrote this past week. “Mine didn’t show up until about over a month after vaccine so I don’t think it was the Covid vaccine.”
It likely wasn’t. Infectious disease experts say there’s little evidence of any connection.
Dr. Katherine Lee, who just treated a case of shingles this past week, hasn’t heard of any significant connection between the coronavirus vaccines and the painful rash also known as herpes zoster.
She thinks some of the “new hype” stems from the results of a small study by researchers in Israel, published in the journal Rheumatology, that found a few people who developed shingles after taking the Pfizer-BioNTech vaccine.
The six patients, out of 491 studied, were all women with compromised immune systems; some had rheumatoid arthritis.
“And from that small study it looked like around 1% of people who got the vaccine developed shingles,” said Lee, a primary care physician at Meritas Health Platte City.
“But you know how social media is. People jump on stuff like that and create headlines and a lot of clickbait out there.”
What is happening, though, is that the rate of shingles among younger and middle-aged adults is rising, according to the Centers for Disease Control and Prevention. It’s not apparent why.
A 2018 study found that case rates of shingles among Americans 35 and older had nearly tripled from 1993 to 2016.
Theories? “We’re not as healthy as we used to be, we’re under more stress, more people are overweight, more chronic disease burdened, that all could be related to one’s immunity,” said Lee.
Meanwhile, cases among older adults have plateaued since 2008, the CDC says, shortly after the first shingles vaccine, Zostavax, was introduced in 2006. It has since been replaced by Shingrix, a more effective vaccine, which the CDC recommends for anyone 50 and older.
Yes, shingles can be prevented.
Or, as the woman in a popular vaccine commercial exclaims: “Shingles can be whaaaaaaaaaaaaaat?”
What is shingles?
Most people who develop shingles have only one bout in their life, but you can have shingles more than once.
The rash usually shows up as a single stripe on just one side of the body or face, says the CDC.
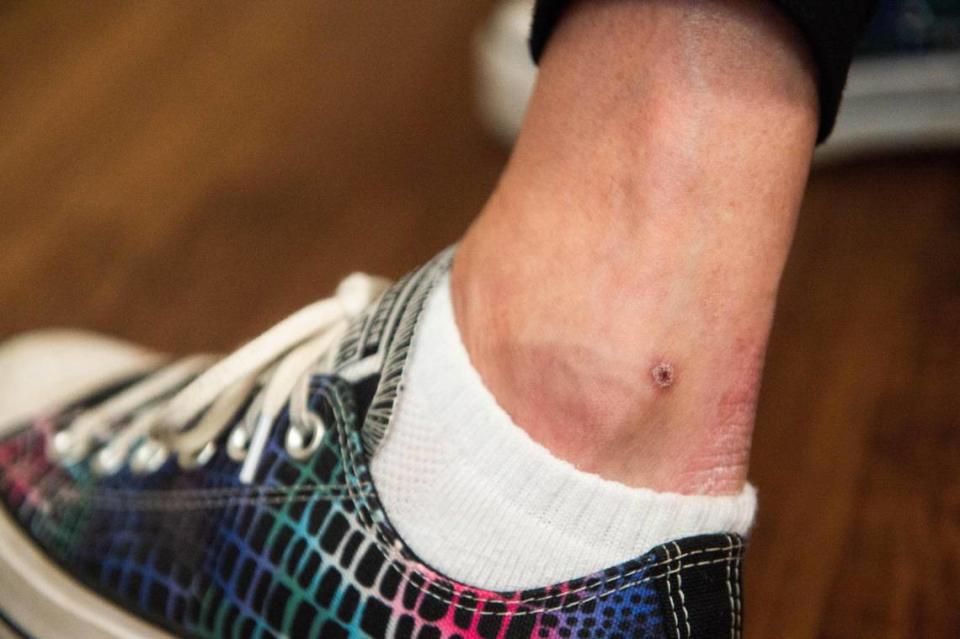
Forbes developed blisters on her legs, an ankle, on top of her hand, “in really weird places. My right trunk was the worst,” said the admissions director for a Kansas City skilled nursing facility.
People often feel the pain before the rash breaks out, said Dr. David Bamberger, professor of medicine at the University of Missouri-Kansas City and chief of infectious diseases at Truman Medical Centers/University Health.
The rash of blisters, which typically scab over in seven to 10 days, is the telltale sign, but other symptoms can include a fever, headache, chills and upset stomach.
“The cases that always make me nervous are the ones on the face around the eyes or around the ears because those can cause complications … especially blindness,” said Lee. “That would be my big concern when it’s around the eyes.”
Lee said people might not realize the complications — including stroke and meningitis — shingles can cause.
The most common is postherpetic neuralgia, or PHN, a condition where the burning pain lasts for months, even years, after the rash and blisters disappear. About 10% to 18% of people who get shingles will get PHN, the CDC estimates.
Fewer, about 1% to 4% of people who get shingles, end up in the hospital with complications, which is more likely to happen among older adults and people with weakened immune systems, the CDC says. That’s also the group that accounts for the fewer than 100 shingles deaths in the United States every year.

Cause of shingles
Shingles is caused by the varicella zoster virus (VZV), which also causes chickenpox. After you recover from chickenpox, the virus stays dormant in your body.
“When somebody gets infected with chickenpox, that virus remains in some of your nerve cells, near your spinal cord,” said Lee. “It doesn’t really do anything, it just kind of lays dormant there. But later in life it can sometimes reactivate,” causing shingles.
Several things can increase your risk for that.
“Age is the biggest one,” said Lee. “Sometimes when people get certain chronic diseases that lower their immunity they can get it. And we find that there’s a link with stress as well.
“Especially pretty severe stress on your body where you feel run down, your immune system isn’t working quite as well. That’s why we think it can reactivate that virus.”
Any health condition that compromises your immune system can increase the risk of that shingles virus reactivating, said Bamberger.
Forbes believes unrelenting stress that began with the death of her husband from cancer in October 2019, followed by COVID-19 that hit hard the nursing home where she works, triggered the virus in her body to roar to life.
“I think people still have a hard time understanding that you can acquire a virus as a child and that it remains dormant and then reactivates 50 or 60 years later,” said Bamberger. “That’s a hard concept to grasp your hands around. But that is the case.”
Forbes didn’t even know she’d had chickenpox when she was a child, which isn’t all that unusual, said Bamberger.
It’s assumed that if you were born in the United States before 1980 you’ve probably had chickenpox, whether you know it or not, he said.
But being vaccinated against chickenpox doesn’t necessarily mean a person can’t get shingles, though the possibility is lessened, some research has shown.

Is it contagious?
Chickenpox is highly contagious. Ask the Kansas City Royals, who dealt with a small outbreak in 2015 when pitcher Kelvin Herrera and outfielder Alex Rioshave contracted the illness.
But, “you cannot get shingles from somebody with shingles. You don’t catch shingles,” said Lee.
However, someone who has never had chickenpox or the chickenpox vaccine can catch the virus from someone with shingles — then get chickenpox.
The virus can be transmitted through direct contact with the fluid in the blisters, and “there actually can be some airborne transmission as well,” said Lee.
“If you have shingles, it’s OK to be around other people if they’ve been exposed to chickenpox or had that in the past,” she said. “But always be careful being around older people who maybe haven’t had that, people who have some immuno-suppression and kids who have never had chickenpox or the (chickenpox) vaccine.”
How is shingles treated?
Timing is key in treating shingles. Antiviral medicines are more effective if taken as soon as possible after the rash appears.
“It’s best to be done within 72 hours,” said Bamberger. “There’s some evidence that by giving antivirals … not only does it make the skin lesions heal better and you feel better faster, but also potentially reduces the likelihood of having the postherpetic neuralgia.”
Pain medicine, either over the counter or prescription, can relieve the pain.
And the itch? Wet compresses, calamine lotion and a lukewarm bath mixed with ground up oatmeal might help, the CDC says.
The shingles vaccine costs what?
The shingles vaccine recommended by the CDC, Shingrix, is a two-shot series, with the booster coming after two to six months.
“The efficacy of the vaccine is high,” said Bamberger.. “It does depend a little bit on your age and the risks of shingles that you have. But overall, it’s well over 90% effective.”
People younger than 50 can still be at risk — children get shingles — but the CDC recommends the vaccine for people 50 and older.
Younger adults are “a little bit less at risk for complications from it,” said Lee. “I don’t know if they’ll make a vaccine for younger people as well. It’s just at this time it’s not recommended.”
Since the vaccine is supposed to cover you for life there would be concern about giving it people younger than 50, Bamberger said.
“Yes, it might protect you for the next 15 years or so. But the concern might be that the duration of the efficacy of the vaccine might wane and that waning might occur when it’s most important to have the protection,” said Bamberger.
As vaccines go, said Bamberger, the shingles series is “a little bit expensive,” said Bamberger.
Recently, the lowest price on GoodRX.com for Shingrix was about $155, 24% less than the average retail price of $205.33.
Insurance doesn’t always pay for it, which makes it unattainable for some people.
“I find it a little bit frustrating because insurance coverage is highly variable. Some cover it very well, and some don’t,” said Lee. “It’s kind of unfortunate it’s that way.”
She tells patients to shop around because prices can vary so much.
Forbes remembers seeing a sign promoting the shingles at vaccine at a local CVS when she was getting her flu shot last September and thinking it didn’t apply to her because she’d never had chickenpox.
She knows better now and plans to get the shingles vaccine soon.
“I would say run, don’t walk,” she said.

