A key benefit of Obamacare is stalling — here's why
The state of health care is a polarizing topic in the U.S. as the 2020 presidential election draws closer. And recent data suggests that the effectiveness of the Affordable Care Act (ACA), the 2010 legislation commonly known as Obamacare, is starting to slow.
A key part of Obamacare involved lowering the number of Americans without health insurance. And according to the U.S. Census Bureau, the uninsured rate increased from 2017 to 2018 — the first year-to-year increase in the uninsured percentage since 2008 to 2009. In 2017, 25.6 million people were uninsured and that number increased to 27.4 million people in 2018, a 0.5% increase.
Sara Collins, vice president at the Commonwealth Fund, said there are “probably four major factors” for this bump in uninsured: affordability issues, congressional and executive actions to counter the ACA, lack of access for undocumented immigrants, and lack of legislation to fix issues with Obamacare.
“Given these factors and particularly lack of Medicaid expansion in all the states and unaffordable premiums for people with incomes who are just over that marketplace subsidy threshold, Congress also hasn’t passed any legislation since the passage of the law that might alleviate some of those issues,” Collins told Yahoo Finance.

Affordability issues and Medicaid
Matthew Broaddus, a senior research analyst at the Center on Budget and Policy Priorities, stressed the importance of Medicaid in the American health care system.
“Medicaid serves many different groups of people who don’t have easy access to health insurance coverage,” Broaddus told Yahoo Finance. “In some cases, it’s people with disabilities who simply would not be able to find a comprehensive coverage plan they could finance. For other people, you’re supporting both children and adults in families who are working in low-wage environments where often health insurance coverage isn’t available.”
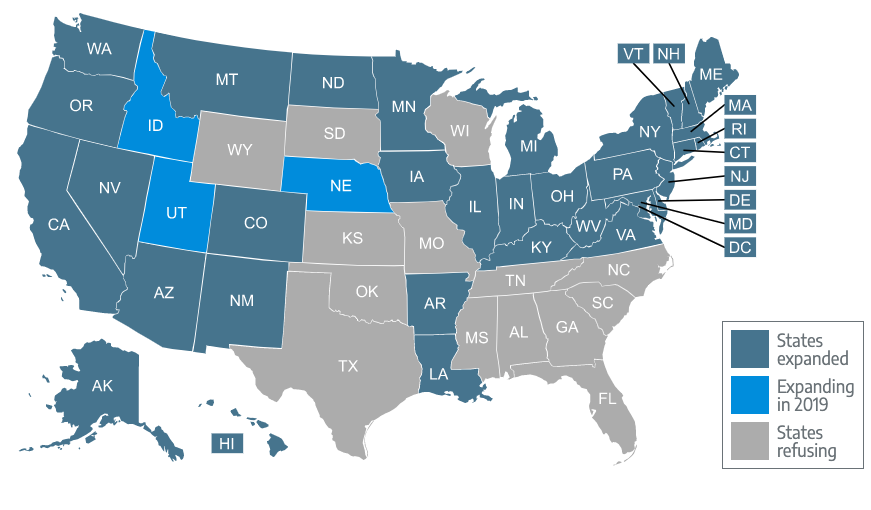
After the passage of the ACA in 2010, Medicaid expansion came under heavy focus. The goal was for those with household incomes up to 133% of poverty to be able to enroll in Medicaid.
“Often, people who don’t have access to Medicaid will go uninsured, and you’ve sort of seen the reverse of that story with the expansion of Medicaid coverage to low-income adults for the first time through the ACA,” Broaddus said. “You saw the numbers of uninsured plummet because of that and you saw greater coverage gains in states that chose to expand Medicaid to low-income adults in states that didn’t. For me, that really serves as evidence of how important Medicaid is and how, without Medicaid, often people don’t have another option for getting affordable health coverage.”
Additionally, there are “premiums that are hard for people to afford who have incomes that are just over that marketplace subsidy threshold, which is about $48,000 for an individual and about $100,000 for a family of four,” Collins said. “So, if you are without coverage through a job, you’re eligible for subsidies. But, if your income is right over that threshold, then you’re paying the full premium, and it can comprise a big share of people’s income when you’re just kind of right over that subsidy threshold.”
It doesn’t help that an estimated 23.6 million Americans with employer coverage had high premium contributions, high out-of-pocket costs, or both, according to a report from the Commonwealth Fund, and that “employer plan premium contributions and out-of-pocket costs, like those for prescription drugs, are eating up an increasing portion of household budgets.”
‘We’re kind of on a teetering spot right now’
Another major factor at play here that Collins stressed are the congressional and executive actions on the Affordable Care Act since 2016, which “includes the repeal of the individual mandate penalty … and Medicaid work requirements.”
The Centers for Medicare and Medicaid Services (CMS) imposed work requirements as a condition of Medicaid eligibility under the Trump administration. This means that Medicaid participants have to verify that they are involved in employment, job search, or job training programs, for a specified number of hours each week or seek an exemption.
“We know that when Arkansas had their work requirement in effect, about 18,000 people lost their health insurance coverage,” Collins said. “So, there have been some changes that have been put in place by Congress and the Trump administration that have had some marginal effects on health insurance coverage.”

Back in 2017, the Congressional Budget Office (CBO) and the Joint Committee on Taxation (JCT) estimated that repealing the individual health insurance mandate “would reduce federal deficits by about $338 billion over the 2018-2017 period and increase the number of uninsured people by 4 million in 2019 and 13 million in 2027.” The CBO is projecting that the number of uninsured people will increase from 30 million in 2019 to 35 million people in 2029.
“For that reason alone, I think you could anticipate, at least in the near term, both the number of uninsured and the uninsured rate going up,” Broaddus said. “And I think we in the policy world have a lot to do with the other levers that potentially could push the uninsured number in one direction or the other — depending on how much support is given to fully enforcing the ACA, people knowing what their options for coverage are, how they can access those options, making certain Medicaid is still available to low-income adults and is relatively seamless to access, not too many barriers like work requirements to getting Medicaid coverage.”
He continued: “Depending on which direction those policy changes go, I suppose you could also anticipate further increases in uninsured. We’re kind of on a teetering spot right now where we have some decisions to make that could push that number in one direction or the other.”
Broaddus noted research from the Commonwealth Fund, which found that hospitals bear a much great burden of uncompensated care costs when the number of uninsured people rises.
However, “the effects on the economy of growing uninsurance is of secondary importance compared to the harm to the health and financial security of the people who lose health coverage,” he said.

In December 2018, a Texas judge ruled that Obamacare’s mandate was unconstitutional. Judge Reed O’Connor agreed with plaintiffs who argued that the lack of a penalty invalidated the “individual mandate” provision of the law and, if that part of the law was now invalid, then the whole law was.
“It’s concerning that the number of people without health insurance has gone up even in a growing economy, but the uninsured rate growth we saw in 2018 pales in comparison to the coverage loss we would see if the Texas lawsuit succeeds in eliminating the ACA,” Broaddus said.
According to an analysis by the Urban Institute, if the Texas ruling were to be upheld, “the increases in uninsurance would be most heavily concentrated among people with the lowest incomes.” Additionally, the states that have implemented the Medicaid expansion through the ACA would see a 92% increase in the number of uninsured people.
“More than 20 million Americans have health insurance today who would not have it without the Affordable Care Act,” Doug Elmendorf, dean of the Kennedy School of Government and the former director of the Congressional Budget Office from 2009 to 2015, told Yahoo Finance earlier this year. “That’s a huge improvement in their access to health care and a reduction in the out-of-pocket costs that they face.”
Elmendorf continued: “Is the law perfect? No. Can we do more to expand health insurance coverage further? Yes. But we’ve wasted almost a decade now in discussing ways to tear apart that act. We should be looking for ways to build on it and move forward.”
Adriana is an associate editor for Yahoo Finance. Follow her on Twitter @adrianambells.
READ MORE:
Millions of Americans with employer health care are still spending a fortune
'Everyone’s health insurance is more expensive' as more Americans manage chronic diseases
'The system is broken': These doctors practice a less pricey form of health care
Read the latest financial and business news from Yahoo Finance
Follow Yahoo Finance on Twitter, Facebook, Instagram, Flipboard, SmartNews, LinkedIn, YouTube, and reddit.


