Omicron coronavirus variant seen as a clarion call to vaccinate the globe
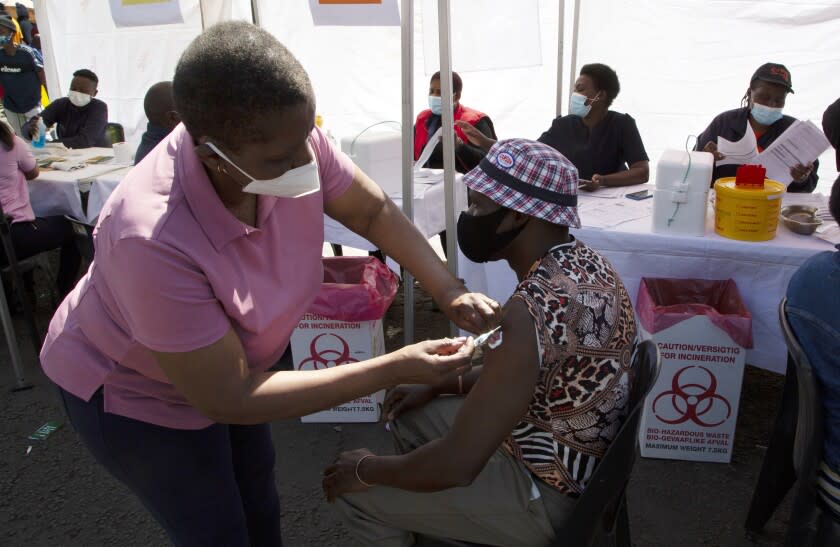
For almost a year since COVID-19 vaccines first became available, many leading health authorities have urged wealthy nations and vaccine manufacturing companies to prioritize inoculating people in poorer Southern Hemisphere nations to help prevent troublesome new variants from emerging.
Since then, vaccines have become readily available in the United States, Western Europe and other developed areas of the world. But in Africa, where the new Omicron coronavirus variant was first detected in recent days, vaccines remain extremely difficult to come by and just 7% of the population is fully inoculated, compared with 42% of the global population and 58% of the United States.
“With this level of vaccine inequality, variants like Omicron are completely predictable,” said Matthew Kavanagh, director of the Global Health Policy and Politics Initiative at Georgetown's O'Neill Institute on Friday. “Boosters and travel bans will not protect Americans. We will continue to live in fear until we fix the vaccine inequalities.”
On Friday, experts at the World Health Organization categorized Omicron as a “variant of concern,” the group’s most serious category.
Scientists caution against drawing conclusions about the variant’s capabilities too quickly: It will take days or even weeks for researchers to run tests and pore over data, according to Tim Schacker, the vice dean of research at the University of Minnesota’s medical school.
Still, the WHO’s announcement is significant: The “variant of concern” label is typically reserved for those with mutations that could potentially make the virus more contagious or virulent, or could render defenses such as vaccinations less effective.
Some previous variants have not lived up to the initial alarm. But the Omicron variant has more than 50 mutations, more than half of them on the virus’ spike protein, the key target of vaccines and subsequent antibodies. Michael Osterholm, an epidemiologist at the University of Minnesota who served on President Biden’s COVID-19 advisory board during his transition into office, called it “surely much, much more concerning than [the] Delta” variant, which now accounts for almost all COVID-19 cases in the United States.
“Of all the variants we have seen to date, this is probably the greatest public health concern we’ve had,” he said. “It could evade some or all of the immunity we have from previous infections and vaccines. We just don’t know.”
While multiple jabs and even boosters have significantly lowered the chances of serious illness or death to those who have taken advantage across the United States and much of Europe, large unvaccinated populations in the developing world provide far more opportunities for the coronavirus to evolve into new forms that could threaten the effectiveness of vaccines.
Africa’s two most populous countries, Nigeria and Ethiopia, both have vaccination rates below 2%. Unless the rate rises dramatically, global variants will be considered inevitable.
COVAX, the WHO initiative to deliver vaccines to low-income countries, has struggled with setbacks, including underwhelming investments by wealthy countries and a surge in Delta cases that kept shots from leaving India, where many of them are manufactured and have been distributed. The campaign is expecting to supply almost half a billion new doses by the end of the year, but has to date delivered only about a third of what it had anticipated.
Some public health experts worry about a discouraging cycle in which new variants prompt wealthy countries to order more boosters, depleting the manufacturing capacity for first and second doses needed in largely unvaccinated regions.
More than 60 developing countries, led by India and South Africa, have proposed temporarily suspending vaccine patents and other intellectual property to enable nations to produce their own vaccines, driving up inventory. Biden, under pressure to help vaccinate people in poorer nations, many in the Southern Hemisphere, has said he supports such a waiver. He repeated his stance Friday, saying that Omicron “reiterates the importance of moving on this quickly.”
But drug companies and the European Union oppose such a move because they say it could discourage pharmaceutical investment, and the United States has done little to push negotiations forward.
“For the last year, rich countries have hoarded doses and paid high prices for boosters in hopes that would keep them safe” instead of focusing on global vaccination, Kavanagh said. He pointed out that much of the cutting-edge vaccine development credited to private companies in 2020 was funded by U.S. taxpayers and used copious amounts of government research.
“It’s long overdue to share this publicly funded know-how with the world so Africa, Asia and Latin America can make vaccines,” he said.
Osterholm counters that although vaccine manufacturing capacity is finite, it is “not helpful or accurate” to suggest that the United States booster rollout had great bearing on the emergence of Omicron. There are other extraordinary challenges to vaccination campaigns in remote regions, including the need for refrigerated transport, coordinated teams of health workers, and — as evidenced in wealthy and poor nations alike — public confidence in the effort. Widespread vaccination depends upon both supply and demand.
“It’s not just an issue of handing people vaccines,” said Anne Rimoin, an epidemiologist at UCLA.
The United States, Britain, Australia and other wealthy nations were swift late this week to restrict travel from southern Africa, triggering backlash from critics who say their vaccine hoarding contributed to the emergence in the first place.
And while travel bans in some cases buy officials time to coordinate a public health response, they often come too late. Omicron has already been detected in locales including Hong Kong, Belgium, Israel and Britain. “The cat’s out of the bag,” Rimoin said.
She and other scientists credit South Africa for an impressive surveillance system that detected, analyzed and reported the new variant to the WHO quickly.
The United States “wouldn’t have caught it at nearly this speed,” Osterholm said. “Those who think of South Africa as contributing to a problem: You ought to be grateful to them.”
Once researchers know how current vaccine formulas stack up against Omicron, next steps will become clearer. Manufacturers may need to modify the formula, and officials would need to prepare a plan to deliver new ones.
In the meantime, public health experts urge global leaders to act upon what’s already clear: Without more vaccines in southern Africa, the virus will retain millions of opportunities to replicate and adapt.
“I’ve been saying for months and months that the future of this pandemic will come down to two issues: waning immunity and new variants,” Osterholm said. “What you see here is that, while so many people around the world are done with this pandemic, the virus isn’t done with us.”
This story originally appeared in Los Angeles Times.

