Oxygen supplies, wasted vaccines, Mummers defiance: News from around our 50 states
Alabama
Montgomery: The state notched almost a third of its coronavirus cases in December, an alarming bulge that echoed the warnings of medical experts who said the state would see some dark days before the widespread availability of a vaccine to fight the pandemic. Alabama saw 109,000 of its 361,226 confirmed and probable COVID-19 cases reported in December. The surge came after the Thanksgiving holiday, and health officials said they are concerned caseloads will continue to grow in January from the fallout of Christmas and New Year’s gatherings. “We are being overwhelmed right now,” State Health Officer Scott Harris said. “I believe, unfortunately, we are going to see even worse numbers than we have now, and the ones we have now are pretty bad.” The cumulative number of confirmed and probable cases was 251,787 on Nov. 30 and rose to 361,226 cases Dec. 31. While there were some backlogged cases recorded in December, almost all of the reported cases were from December.
Alaska
Anchorage: Health officials said the state plans on receiving almost 53,000 doses of coronavirus vaccines this month from drug companies Pfizer and Moderna. That figure is about 7,000 fewer vaccines than the state received in December. Thus far, only front-line health care workers in hospitals, residents and employees at long-term care facilities, emergency personnel, community health aides and people conducting vaccinations have been eligible to be inoculated in Alaska. Starting Monday, another tier of people will begin receiving vaccines. That group includes people working in health care who are at the highest risk of contracting the virus, are considered essential to the health care system, and do regular work that can’t be done remotely or postponed. Almost 50 Alaska residents spoke at a public hearing last Monday to advocate for their demographic to be included in the next vaccination group. That group included teachers, older adults and seafood industry workers, the Daily News reports. Alaska has so far vaccinated over 13,000 people, according to a state tracker last updated last Monday.
Arizona
Phoenix: Despite a surge of coronavirus cases, Gov. Doug Ducey on Saturday rejected the state’s top education official’s call for him to order public schools to use only distance learning for the next two weeks unless they have waivers from health officials. “Given the severity of our state’s situation and the virus’s trajectory after the holiday period,” schools need a “two-week quarantine period” for education leaders and local officials to use local health data “to decide the appropriate instruction model for their communities,” Superintendent of Public Instruction Kathy Hoffman said in a Twitter thread. Hoffman called for the two-week “quarantine period” for schools after the Department of Health Services on Saturday – the second day of the new year – reported nearly 8,900 additional known COVID-19 cases, giving the state a two-day pandemic high for new cases. However, Ducey spokesman C.J. Karamargin said the governor “will not be considering this request or issuing this kind of mandate. This is a local decision. The online option is already available, and the governor has repeatedly made his preference clear: Kids have already lost out on a lot of learning, and he wants schools opened, safely.” Many schools are set to resume classes this week after the winter holidays.
Arkansas
Little Rock: Coronavirus hospitalizations in Arkansas have again set a new record high, as the pandemic strains medical resources across the state. There were 1,216 people in Arkansas hospitals with confirmed cases of COVID-19 on Saturday, state health officials reported, an increase of 31 from the day before. Arkansas has repeatedly broken previous records for hospitalizations and case counts over the past week, as the virus surges following holiday gatherings and travel. The Arkansas Department of Health also reported 1,597 new confirmed cases of COVID-19, 403 more probable cases and another 18 deaths. Those case counts are down from Friday’s record high, but Gov. Asa Hutchinson warned that the numbers were deflated by a drop in testing on New Year’s Day. The actual number of cases is believed to be far higher because many people haven’t been tested, and some who get sick don’t show symptoms.
California
Los Angeles: Hospitals struggling to provide enough oxygen for the sickest coronavirus patients in the Los Angeles area began to receive help Saturday when U.S. Army Corps of Engineers crews arrived to update their oxygen delivery systems. The collaboration comes as the six aging hospitals struggle to maintain oxygen pressure while treating an unprecedented number of patients with respiratory issues. Some COVID-19 patients can require 10 times as much oxygen as a normal patient. California started the new year Friday by reporting a record 585 coronavirus deaths in a single day. The state Department of Public Health on Saturday reported another 386 deaths and more than than 53,341 new confirmed COVID-19 cases. More than 20,000 people were hospitalized as of Saturday with COVID-19; 4,500 of them were in intensive care, according to state records. The southern half of the state has seen the worst effects, from the agricultural San Joaquin Valley to the Mexico border. Hospitals are swamped, and intensive care units don’t have any more beds for COVID-19 patients. Makeshift wards are being set up in tents, arenas, classrooms and conference rooms.
Colorado
Denver: A day after Gov. Jared Polis announced that restrictions for places like restaurants and gyms will be eased in much of the state starting this week, some local public health officials said they were concerned about the move. The governor cited improving statewide COVID-19 metrics in lifting certain restrictions in 33 counties, including Denver and the entire Front Range, but his announcement Wednesday came as not all of those counties meet the individual requirements to downgrade restrictions, the Denver Post reports. “It appears that if there’s enough pressure from the business and economic forces in the state that we will change the dial to meet those demands, and that’s kind of frustrating,” said Mark Johnson, executive director of Jefferson County Public Health. The announcement came a day after Colorado said it had confirmed the United States’ first case of a new and apparently more contagious variant of the coronavirus. “We don’t believe that it in any way reflects the spread of the disease or how dangerous the disease is or our concern about what is going to happen with Christmas, New Year’s or the new variant that is more infectious,” Johnson said.
Connecticut
New Haven: Some of the city’s public school students will return to their physical classrooms later this month for the first time since last spring, according to the superintendent of schools. Superintendent Iline Tracey announced on the district website Thursday that officials are preparing for “a limited return of students to a hybrid learning model” starting Jan. 19. The New Haven district has been closed for in-person instruction except for some special-needs programs since the coronavirus pandemic forced schools across the country to shut down last March. Officials in New Haven chose to keep school buildings shuttered in September as other districts in Connecticut offered either full-time or part-time in-person learning. A plan to reopen New Haven’s schools on Nov. 9 was shelved amid rising COVID-19 cases. Tracey said schools will open Jan. 19 to students in prekindergarten through fifth grade as well as students in special-education programs and programs for new immigrants at two of the district’s schools. Two schools, Quinnipiac School and West Rock School, will remain closed because city health officials determined that a lack of ventilation renders them unsafe during the pandemic, Tracey said.
Delaware
Wilmington: After health workers, long-term care staff and long-term care residents are inoculated, the next people to get the COVID-19 vaccine in the state will be front-line essential workers and residents 65 and older. Dr. Karyl Rattay, director of the Delaware Division of Public Health, announced the state’s decision during Gov. John Carney’s weekly coronavirus press briefing Tuesday. Front-line essential workers include first responders such as firefighters and police, as well as teachers, U.S. Postal Service workers and grocery store workers. The group also includes corrections officers, food and agricultural workers, day care workers and public transit workers. But these people likely won’t start getting the vaccine until mid- to late January due to the limited supply of the vaccine. “Please be patient with us. There’s just not enough vaccine for everyone right now,” Rattay said, adding that employers need to start planning how they will administer their vaccine to workers. People who work in Delaware but live in a neighboring state will likely be eligible for the vaccine in Delaware because they will likely get it through their employer.
District of Columbia
Washington: Curators Sam Vong and Shannon Perich at the National Museum of American History are collecting written submissions from people across the country describing how they experienced 2020, WUSA-TV reports. “As historians, what we really want to do is document what’s going on before it kind of escapes from us,” Vong said. The Smithsonian museum has put out an open invitation to submit, with the hope that Americans’ recollections will preserve for the future the experiences of a year that really was like no other. “All of these stories will help people drill down or will open up new avenues of exploration and research,” Perich said. The submissions can be mundane. “What did it mean to sit in your home by yourself?” asked Perich. “The only way we’re ever going to know the answer to that question is if people tell us.” Or they can be extraordinary, like one of Vong’s favorites so far from a former Bhutanese refugee who resurrected a grassroots media outlet to share information during the pandemic. The submission period opened in December and runs through March.
Florida
Fort Lauderdale: Health officials reported a two-day total of 30,767 new cases of the coronavirus in the state and 217 new deaths Saturday. Florida’s Department of Health did not release numbers on New Year’s Day. The state has also chosen not to report COVID-19 cases on two other holidays, Thanksgiving and Christmas. The two-day total brings the overall number of confirmed COVID-19 cases in Florida to 1,354,833. The agency posted that 21,015 cases were reported Friday and 9,752 reported Saturday. The state’s death toll throughout the coronavirus pandemic stands at 22,074. On New Year’s Eve, the state reported the highest daily jump in COVID-19 cases ever detected in Florida, with 17,192 new cases. Also on Thursday, state health officials disclosed in a statement tweeted on the department’s HealthyFla site that evidence of a new and apparently more contagious coronavirus strain first seen in England has been detected in a Martin County man with no recent travel history. Martin County is north of Palm Beach County, which along with Miami-Dade and Broward counties have comprised the state’s hardest-hit region in dealing with coronavirus cases.
Georgia
Augusta: As vaccines are being administered to health care workers and long-term care facility residents and staff, law enforcement and first responder agencies are in line to get them soon. Gov. Brian Kemp and Georgia Department of Public Health Commissioner Dr. Kathleen Toomey announced Wednesday that adults 65 and older, law enforcement officers, firefighters and first responders were being added to Phase 1A – the highest-priority group eligible to receive vaccinations. Some Augusta-area firefighters and deputies have already started getting vaccinated. The Richmond County Sheriff’s Office said some deputies were inoculated last week, and it is in the process of compiling a list of deputies interested in getting the vaccine. Dr. Stephen Goggans, the director of the East Central Health District, said the timeline for first responders and those 65 or older to get vaccinated was moved up because some parts of the state have already completed or are close to completing vaccinations for health care workers and long-term care facilities.
Hawaii
Honolulu: Residents have been warned to be extra vigilant and continue to follow safety guidelines as cases of a new, seemingly more contagious strain of the coronavirus have recently been reported in the U.S., health officials said. The Hawaii Department of Health, along with the Centers for Disease Control and Prevention, said there have been increased efforts to find the new variant and to understand how it is transmissible, the Honolulu Star-Advertiser reports. It has not been detected in Hawaii. Confirmed cases of the new coronavirus strains have been found in the United Kingdom and South Africa and in the U.S. in Colorado, California and Florida. “All we know is that we have not yet found it,” State Laboratories Division Dr. Edward Desmond said. “We’re going to cast a wide net to see if we can quickly find it when it is here, and then we can make decisions about whether that should impact our community mitigation measures.” The vaccines being distributed are thought to be effective against the new strain. Health officials have said about 25,000 COVID-19 vaccines have been administered statewide. Local pharmacies received a surprise shipment of 3,800 doses last week, boosting the total delivered in December to 65,250.
Idaho
Boise: Gov. Brad Little plans to propose tax cuts and investments in transportation, education and water projects to lawmakers this month following another monthly revenue report that exceeded projections despite rising coronavirus infections and deaths. The Republican governor in a statement last month spent little time trumpeting the budget numbers and his fiscal conservatism as he has in the past during live news conferences. The latest numbers show a projected budget surplus of $630 million after November tax revenue came in $45 million higher than expected. For 2020, state revenues were ahead of projections by nearly $170 million, or 10.6%. Little warned that tax cuts and investments are threatened by the pandemic that could overwhelm hospitals with COVID-19 patients. Among those getting sick with the virus are health care workers, he said. “Health and the economy are intertwined,” Little said. “Idahoans must choose to do a better job of wearing masks and avoiding gatherings with people outside their households if we are going to continue this trend.”
Illinois
Chicago: The state’s public health department reported 29 COVID-19-related deaths Saturday, the smallest one-day total in Illinois since mid-November. Not only was the total, included in a news release from the Illinois Department of Public Health, lower than any single day since Nov. 13, but it is also just about a quarter of the 111 daily deaths the state has been averaging over the past two weeks. The latest numbers bring the number of COVID-19-related deaths in Illinois since the pandemic began to 16,674 and the number of cases to 975,352. The health department also reported that there were 4,762 new confirmed and probable cases, bringing the total since the pandemic began to 975,352. But the release included a potentially worrisome statistic as well. The cases that were detected among 61,987 tests submitted on New Year’s Day helped raise the statewide average positivity rate over the past week to 8.3% from 6.8% a week ago, according to the Chicago Sun-Times.
Indiana
Indianapolis: Anxiety, depression and other mental health conditions have become more prevalent among Hoosiers since the onset of the coronavirus pandemic, the state’s top health officials said in calling for renewed attention on mental health resources. Many of those reporting mental health woes are affected by COVID-19 itself, Jennifer Sullivan, secretary of the state’s Family and Social Services Administration, said during Gov. Eric Holcomb’s weekly briefing Wednesday on the state’s coronavirus response. That includes dealing with loss and fear, disruption to daily life with recurrent needs for quarantine and isolation, changes to school and work schedules, unexpected illness of friends and family, and disruption to normal social supports. Cold weather and the holiday season, too, have likely added difficulties for people with existing mental illnesses and those experiencing acute stress, she said. As a way to help, Sullivan encouraged Hoosiers to use the state-run BeWellIndiana.org to take a mental health self-assessment. Since April, more than 25,000 Hoosiers have completed those assessments. For more than three-quarters of those taking the surveys, there was confirmation of a mental health diagnosis, Sullivan said.
Iowa
Des Moines: A federal judge has rejected an argument by Tyson Foods that is is not liable in the death of a worker because it was following federal guidance when it kept meatpacking plants open during the coronavirus pandemic. Tyson was sued in August by the family of Isidro Fernandez, who worked at the company’s plant in Waterloo, after he died April 26 from complications of COVID-19. More than 1,000 Tyson workers tested positive for the virus in May, and at least six died. The families of Fernandez and at least three other employees who died claim in lawsuits that the company was negligent in how it reacted to the pandemic. Tyson fired seven managers in December after an investigation found that supervisors held a betting pool on how many employees would test positive for the coronavirus. The Fernandez case was filed in state court but was moved at Tyson’s request to federal court after the company claimed it was following the direction of federal officials, including President Donald Trump, when it remained open in April. But last Monday, U.S. District Judge Linda Reade rejected the argument.
Kansas
Topeka: The state will rely on genetic tests to identify cases of a new and apparently more contagious coronavirus strain that was first seen in England, the director of the state Department of Health and Environment said last week. No cases of the new strain have been detected in Kansas. Cases have been confirmed in Colorado, Florida and California. Dr. Lee Norman said Kansas already does genetic testing with about 1% of COVID-19 patients and plans to increase its lab capacity so it can do more tests. Norman told reporters during a Statehouse news conference that Kansas already has seen other variations of the virus that causes COVID-19, including a “Utah strain” and a “Wisconsin strain.” “Viruses always change, kind of over time, with minor genetic variations. Mostly, they don’t make much difference,” Norman said. “They’re more alike than different, quite honestly.” The state on Friday reported another 138 deaths from COVID-19 since Wednesday, for a total of 2,879 since the pandemic began. Kansas has confirmed 227,745 COVID-19 cases, an increase of 5,312 since Wednesday, the health department said.
Kentucky
Louisville: New coronavirus cases leaped in the state in the week ending Saturday, rising 22.7% as 18,408 cases were reported. The previous week had 14,999 new cases of the virus that causes COVID-19. Kentucky ranked No. 24 among the states where the coronavirus was spreading the fastest on a per-person basis, a USA TODAY Network analysis of Johns Hopkins University data shows. Testing has changed around the holidays, making comparisons difficult. Labs and testing sites closed. People traveled or prepared for the holidays instead of getting tested. The worst weekly outbreaks on a per-person basis were in Boyle, Lawrence and Clinton counties. Adding the most new cases overall were Jefferson County, with 2,743 cases; Fayette County, with 1,170 cases; and Kenton County, with 702. Weekly case counts rose in 79 counties from the previous week. The worst increases from the prior week’s pace were in Oldham, Hardin and Jefferson counties. The share of Kentucky test results that came back positive was 18.9% in the latest week, compared with 13.6% in the week before, a USA TODAY Network analysis of COVID Tracking Project data shows.
Louisiana
Baton Rouge: With the announcement that the state soon will allow people ages 70 and older to get the coronavirus vaccine, residents clamoring for the immunizations have hurried to pharmacies trying to receive a shot, even though those vaccinations don’t begin until Monday and require a scheduled appointment. The Louisiana Department of Health said Friday that it has received multiple reports of people who meet the new, expanded criteria showing up at pharmacies, overwhelming their phone lines and even calling some hospitals trying to get vaccinated days before doses are available. Health department spokeswoman Aly Neel stressed that only a limited supply of 10,000 Moderna vaccine doses will be available this week for those newly eligible, that only certain pharmacies will be administering those doses, and that appointments are required to receive the shot, or the person will be turned away. Still, news of wider availability was drawing intense interest, which Neel described as a promising sign. With thousands of first doses of the two-dose vaccines administered to the first-prioritized groups, Gov. John Bel Edwards announced Thursday that he is expanding the list to include anyone 70 and older, people with kidney failure and additional health care workers.
Maine
Augusta: Protesters gathered outside the Maine Statehouse on Saturday to criticize how Democratic Gov. Janet Mills has handled the coronavirus pandemic. WABI-TV reports the protest organized by the Swinging Gate Organization attracted a large crowd despite snowy weather. “There’s this undercurrent of pent-up energy that’s not doing well under this governor’s rule, and it’s important to harness that organic energy that’s out here that needs something to do; their hands are tied,” said event organizer Dick Campbell. More than 25,000 people have tested positive for the virus in Maine, including nearly 350 new confirmed cases announced Sunday. One additional death was announced, bringing the total since the pandemic began to 359. Just under 33,000 people in the state have been vaccinated against the virus. The seven-day rolling average of daily new cases in Maine increased over the past two weeks, going from 445 on Dec. 19 to 528 on Saturday.
Maryland
Baltimore: The Maryland Department of Health is working with regional and federal partners to test patient samples for infection with the new variant of the coronavirus. The Baltimore Sun reports the U.S. Centers for Disease Control and Prevention are collaborating with the state’s public health lab, as well as state laboratories in California and Delaware, to test for the apparently more contagious variant. There have been at least two cases of the COVID-19 variant identified in the U.S., one in California and another in Colorado. A Maryland health department spokesman said the variant has not been detected in Maryland. The CDC has said medical professionals do not now believe that the new variant is more deadly than existing ones or that it will not respond to vaccines. But it could much more contagious and make the pandemic even harder to contain.
Massachusetts
Boston: Gov. Charlie Baker signed a wide-ranging health care bill Friday that he said will codify in law many of the emergency changes made to the state system in response to the coronavirus pandemic. The Republican said the new law extends requirements for all insurance carriers in Massachusetts to cover COVID-19 testing and treatment. It also increases insurance coverage for telehealth services, which have become vital during the pandemic. Baker’s office said the law also expands the scope of practice for nurse practitioners, other specialized nurses and optometrists; takes steps to protect consumers from surprise medical bills; and calls for a study on the effects of COVID-19 on the health care system, among other steps. Meanwhile, a COVID-19 field hospital that was supposed to open at UMass Lowell last week instead will open Monday after staffing shortages delayed the “soft launch.” While the site has capacity for 77 beds, the facility has so far only recruited enough nurses to staff one 14-bed pod. Lowell General Hospital currently has 63 COVID-19 patients at its main campus.
Michigan
Calumet: A judge has ordered the shutdown of a cafe in Michigan’s Upper Peninsula where customers have been supporting an owner who has defiantly served indoor diners despite coronavirus restrictions. Gov. Gretchen Whitmer’s administration got a restraining order against Cafe Rosetta in Calumet, a small town in Houghton County. Since November, bars and restaurants in Michigan have been limited to carryout service or outdoor dining in an effort to reduce the spread of the coronavirus. Kristi Painter, a state food scientist, visited the cafe for an undercover exam and observed a busy place with 17 people eating or drinking. She ordered a cup of bean soup and a half turkey sandwich. “I did not observe any signs encouraging mask use. … I observed a tip-jar like container that was labeled ‘Legal Fund-join our fight to stand up for your rights,’ ” Painter said in a court filing. Cafe co-owner Amy Heikkinen, a mother of six, said she can’t afford to limit her business to carryout orders. She said sales are up because of her dispute with authorities. “It’s my right to earn an income to protect and feed my family,” she said. “That’s the right of every American. You can’t make me not work.”
Minnesota
Minneapolis: The state on Saturday reported 54 deaths from COVID-19, along with 2,543 positive coronavirus tests, in its final reporting period of 2020. The new numbers bring the state’s pandemic death toll to 5,377 people. A total of 417,832 cases of the coronavirus were detected since the pandemic began. The Department of Health has reported a slowdown in new cases, with the average number of daily new cases decreasing by 48% over the past two weeks. In that period, the state reported one of the nation’s lowest rates of new cases per capita, according to Johns Hopkins researchers. Gov. Tim Walz has kept a ban on indoor dining in place through the holiday period, but some businesses defied that order for New Year’s celebrations. The attorney general has sued one such bar, Alibi Drinkery in Lakeville, for repeated violations of the order. Despite a court injunction ordering it to close, people packed into the bar for a New Year’s party, the St. Paul Pioneer Press reports.
Mississippi
Columbus: A hospital is offering $5,000 bonuses for qualified nurses as it works to recruit staff during a pandemic and at a time when health care workers are in short supply. WCBI reports Baptist Memorial Hospital - Golden Triangle is offering a number of incentives including the bonus as it works to recruit amid a nationwide nursing shortage. Johnny Judson is responsible for recruiting nurses for the hospital. “I am literally in every school, nursing school, in the area, including along the Alabama border,” he told the station. “I go up to north Mississippi, south Mississippi, and I go to these nursing schools, and I talk to these students.” He said the country’s nursing shortage has been going on for years, and the coronavirus pandemic has made things worse. The bonus is for registered nurses with at least two years of experience. Judson stressed that there are no shortcuts when it comes to hiring new staff. “We put incentives in place to attract more people, but we don’t lower the standards,” he said.
Missouri
Jefferson City: The chairman of the Missouri Veterans Commission resigned after releasing an investigative report that criticized the commission for its response to the coronavirus pandemic, which has claimed more than 140 lives at seven veteran nursing homes since September. Tim Noonan told the St. Louis Post-Dispatch on Thursday that he was resigning, citing comments Gov. Mike Parson made last week about the veterans and the commission. A summary of the investigation was released earlier in December, but Noonan, who was commission chairman since 2017, had resisted an open records request from the Post-Dispatch to release the full report. Officials inside Parson’s administration and state Sen. Jill Schupp, a Democrat from Creve Coeur, had urged Noonan to release the full report, and he did so after Attorney General Eric Schmitt directed him to, Noonan said. That came after Parson on Wednesday expressed frustration with the commission, which is an independent body. “I’m not going to worry about everybody’s personal lives that sit on the commission, or the chairman,” Parson said. “I’m just going to absolutely worry about the veterans, and that’s my whole focus.” Noonan said he resigned because of those comments.
Montana
Bozeman: Montana PBS has announced plans to renew a broadcast created at the beginning of the coronavirus pandemic in March to support schoolchildren who were learning remotely or in temporary quarantine. The new schedule for the Learn at Home broadcast was set to launch Monday and continue through the end of the school year June 4, the Bozeman Daily Chronicle reports. The shows run each weekday from 6:30 a.m. to 5:30 p.m. and cover multiple subjects from language arts, social studies, science and math for elementary and middle school students. “We know that not all households in the state have the same access to devices and a strong internet connection but that most homes have a TV that receives our broadcast signal,” Montana PBS Director of Education Nikki Vradenburg said. Chief Operator Paul Heitt-Rennie estimated most households have tuned into the Learn at Home program. He said Nielsen data through the summer showed it was watched by up to 150,000 households, or up to 45% of households in the state. “Every educator we talked to asked us to keep it going,” Vradenburg said.
Nebraska
Omaha: Restaurants that were allowed to start selling carryout cocktails amid the pandemic want to continue doing so even after the public health crisis wanes. The Omaha World-Herald reports the Nebraska Restaurant Association plans to push for the expansion during the upcoming 2021 legislative session. The waiver extends until the end of the pandemic emergency. “This is a way for our restaurants to survive and come out the other side of this pandemic,” said Zoe Olson, the executive director of the restaurant group. Olson said the association’s proposal would include a requirement for some sort of seal on carryout beverages that, if broken, would indicate someone had opened their takeout drink in transit. The proposal would also end to-go drinks at some point, so legislators could review the policy and decide whether it should be extended. But the idea is getting some pushback from groups that oppose binge drinking and drunken driving. “When you increase the availability and the ease of access to alcohol, that’s when you get increased harms,” said Chris Wagner, executive director of Project Extra Mile, an Omaha-based group that seeks to prevent or reduce problems associated with alcohol.
Nevada
Las Vegas: Community advocates and health officials are working to engage with the state’s diverse communities and reach out in Spanish and other languages as Nevada lays plans for mass coronavirus vaccinations. Erika Marquez, a University of Nevada, Las Vegas public health professor and vice chair of the Nevada Minority Health & Equity Coalition, said merely translating information about the vaccine into other languages is not enough. “We had to engage these communities in the conversation, and that takes some time,” Marquez told the Las Vegas Sun. Nevada is a diverse state with a 29% Latino population that includes native Spanish speakers. Nevada also has a fast-growing group of Asian American and Pacific Islanders, of which 70% speak a language other than English at home, according to data shared by Asian and Pacific Islander American Vote. Marquez’s coalition has been working throughout the pandemic to share information encouraging physical distancing, hand hygiene and masks with diverse communities and is preparing vaccine education materials in English, Spanish, Vietnamese, Korean, Chinese and Thai.
New Hampshire
Concord: The state has set a goal of administering 100 shots per hour at each of the 13 state-run COVID-19 vaccination sites when it moves to Phase 2. Perry Plummer, the former assistant commissioner of safety, is overseeing vaccine distribution. He told WMUR-TV the goal is realistic, but it will take time to get the effort up to speed. “We expect this to be a little bit of a windy road and to make sure we’re ready to take turns wherever we need to, to make sure we can get people vaccinated in the State of New Hampshire as quickly as possible,” Plummer said. The first phase of distribution has focused on health care workers, nursing home residents and staff, and first responders. The second phase includes teachers, critical workers in high-risk settings, homeless shelter residents and others. As of Friday, more than 21,000 vaccines had been administered.
New Jersey
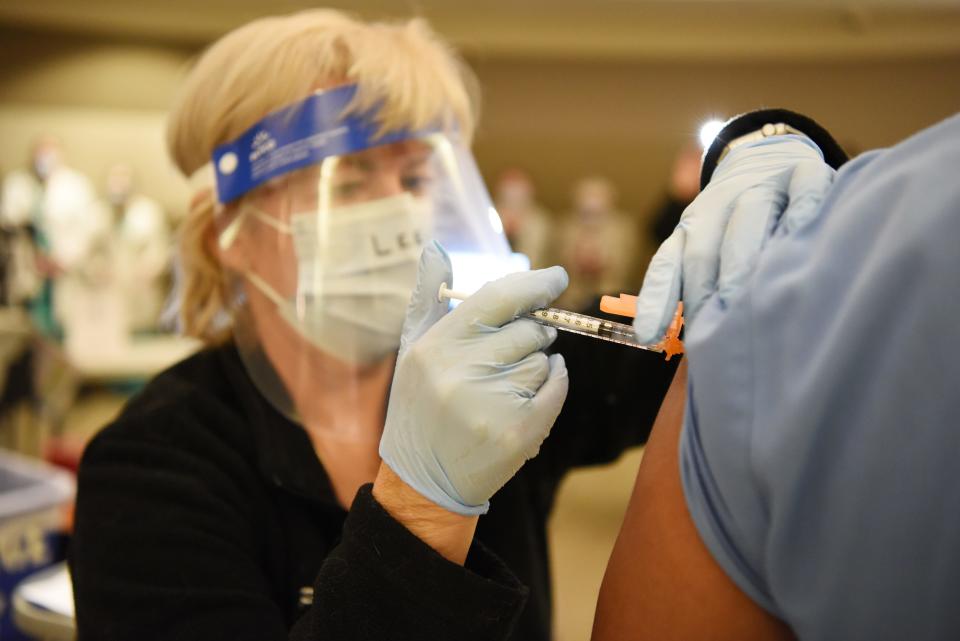
Trenton: More than 70% of the state’s supply of COVID-19 vaccine had not been used as of Thursday, echoing a national trend of slow distribution, according to data released by state officials. Of the 265,000 doses of the Pfizer and Moderna vaccines that have been delivered to New Jersey, 72,657 residents had been given a shot by Thursday afternoon. Despite months of planning, state officials said Wednesday that a lack of personnel, along with logistics and timing issues, was to blame. “Remember, you need health care workers to do this,” Gov. Phil Murphy said at a briefing. “I’m not qualified to deliver these vaccines.” The slow rollout has been frustrating to a public eager to end a pandemic that has infected at least 477,000 New Jerseyans, killed more than 19,000 and caused vast economic hardship. State Health Commissioner Judy Persichilli said the rollout of the Moderna vaccine in particular has been slow because it was delivered just before Christmas. Persichilli said 57% of the state’s stockpile of Pfizer doses had been administered as of Wednesday, calling it “one of the highest percentages that I’ve seen nationally.”
New Mexico
Albuquerque: More than 6,500 businesses and nonprofits will receive up to $50,000 under a state program created to help companies cope with economic fallout from the pandemic. That’s about half of the companies that applied, the Albuquerque Journal reports. “The number (of applications) that we couldn’t fund was very hard for us,” said Marquita Russel, CEO of the New Mexico Finance Authority, the state agency that administered the program. The state implemented the program to help businesses as part of a bigger $320 million coronavirus relief package passed by New Mexico lawmakers. The program uses $100 million in federal coronavirus relief funds allocated to the state. About $40 million of that sum was allocated for businesses located outside the state’s four largest cities. Russel said while her agency had expected to receive roughly 10,000 applications, it received more than 14,000. In all, 6,530 applications were funded. Russel said the agency prioritized businesses that experienced the most significant losses as a result of the pandemic.
New York
New York: The New York City Sheriff’s Department shut down a series of illegal New Year’s Eve parties for violating coronavirus restrictions, operating without a liquor license and other infractions, authorities announced Friday. More than 300 people gathered Thursday night for karaoke and dancing at an illegal bottle club on 58th Street in Queens, the department said on Twitter. Five people were charged with offenses including violating emergency orders that ban indoor gatherings, providing alcohol without a liquor license and obstructed egress. Deputies also raided an illegal gathering on Prince Street in Soho, where more than 145 people were partying in a space with no liquor license, the department said. Four people were charged with multiple offenses. The patrons were not wearing masks in the venue’s overcrowded sixth floor. Deputy sheriffs also found nearly 80 people dancing and smoking hookah at Stars Hall in the Sunset Park section of Brooklyn. The organizer of the event was ticketed for violating an executive order.
North Carolina
Raleigh: COVID-19 hospitalizations and test positivity rates both are reaching record highs in the state. The News & Observer of Raleigh reports there were a record-high 3,576 people hospitalized with COVID-19 over the weekend, according to data reported by 95% of the state’s hospitals. Two weeks ago, there were 2,783 people hospitalized with the virus. That’s a difference of 793 people. On Friday, the last day for which data is available, the state’s health department says 13.6% of COVID-19 tests came back positive. That brought the seven-day average of daily testing results to 14.2%, the highest rate since at least April. The average is seen as giving a better indication of COVID-19 spread because it better accounts for daily spikes and valleys. Every day since Christmas has seen a double-digit positivity rate, including Thursday’s record-high 15.5%.
North Dakota
Fort Yates: The Standing Rock Sioux Tribe is prioritizing the distribution of COVID-19 vaccines to those who speak Dakota and Lakota languages. Standing Rock Tribal Chairman Mike Faith told KXMB-TV the policy is aimed at keeping customs alive. “It’s something we have to pass on to our loved ones – our history, our culture, our language. We don’t have it in black and white; we tell stories. That’s why it’s so important,” Faith said. The Standing Rock reservation straddles the North Dakota and South Dakota border and is home to about 8,000 people, more than half of whom live in North Dakota. Faith said only about 300 people on the reservation are fluent in the language. Front-line health care workers already have begun receiving the vaccine at the Fort Yates hospital, but starting this week, priority will be for those who speak their native language. In addition to those who can carry on the culture, the next phase includes elders, law enforcement, tribal courts and the school system, tribal officials said. Tribal Health Director Margaret Gates said the Lakota and Dakota speakers “are the most important asset to our tribe and people because of the language.”
Ohio

Columbus: As Gov. Mike DeWine applies pressure to get COVID-19 vaccines administered faster throughout the state, those charged with inoculating people against the virus say a combination of factors has contributed to a slow rollout. Vaccines arrived during the holidays, when more workers were off and less likely to be available to get the vaccine. In some cases, “vaccine hesitancy” has contributed to lower demand as well, they say. Shipments also have been unpredictable, sometimes arriving later than expected or in smaller quantities than previous allotments, making it difficult to plan for distribution. Protocols require a 15-minute observation window for each patient, limiting the number of people who can cycle through a chair each day. “This is not your routine stop by the primary care office to get a flu shot. This is a whole different operation,” said Dr. Andy Thomas, chief clinical officer at Ohio State University’s Wexner Medical Center. On Wednesday, DeWine said he had grown “impatient” with the rollout and challenged hospitals to administer the vaccine within 24 hours of receiving it, calling it a “moral imperative” to get the vaccine out as quickly as possible.
Oklahoma
Oklahoma City: The state has reported more than 1,000 new COVID-19 cases, as hospitalizations from the disease caused by the novel coronavirus remained near their all-time high. Oklahoma recorded 1,083 new confirmed cases of the virus Friday and another 38 fatalities, state health officials said Saturday. The Oklahoma State Department of Health has delayed reporting case counts over the holiday weekend. The actual number of cases is believed to be far higher because many people haven’t been tested, and some who get sick don’t show symptoms. There were 1,910 people hospitalized with the virus in Oklahoma on New Year’s Day, according to the department. The state’s record was set last Monday, when there were 1,927 people with the virus in Oklahoma hospitals. Over the past week, more than 18% of coronavirus tests in Oklahoma have come back positive, according to data from Johns Hopkins University.
Oregon
Portland: A health care worker was hospitalized after having a severe allergic reaction to the Moderna COVID-19 vaccine, according to the Oregon Health Authority. The worker, an employee at Wallowa Memorial Hospital, experienced anaphylaxis after receiving a first dose of the vaccine last week, officials said late Thursday. The health authority said vaccines for COVID-19 can cause mild to moderate side effects in some people, including pain and swelling on the arm and sometimes fever, chills, tiredness and headache. “The Centers for Disease Control and Prevention has reported that in rare cases, some people have experienced severe allergic reactions after getting a COVID-19 vaccine,” health officials said in a press release. “An allergic reaction is considered severe when a person needs to be treated with epinephrine or EpiPen, or if they must go to the hospital.” Health officials will continue to track adverse reactions to the COVID-19 vaccines.
Pennsylvania
Philadelphia: Scores of costumed performers took to the streets of their south Philadelphia stomping grounds for a New Year’s celebration of Mummers tradition, far from the customary parade route and despite official cancellation of the annual event and a ban on large gatherings due to the coronavirus pandemic. Participants in brightly colored costumes, some with faces painted, paraded down 2nd Street in South Philadelphia on Friday following trucks that blared string band or popular music. Some wore masks, but many did not. Mayor Jim Kenney announced in July that the city would not grant permits to planned outdoor events with more than 50 people, effectively canceling the large annual parade and other events as officials struggled to keep a lid on the spread of the virus. Some Mummers leaders and organizations also asked members to stay home. City spokeswoman Lauren Cox said there were no major issues Friday but said seeing pictures of many participants without masks was “very concerning given the seriousness of this current wave of the pandemic.” She urged voluntary quarantines and testing for anyone who had been in large crowds.
Rhode Island
Providence: The first person to get vaccinated against the coronavirus in the state got his second shot Saturday. Dr. Christian Arbelaez, an emergency room physician at Rhode Island Hospital in Providence, received his second dose without the fanfare that surrounded him nearly three weeks prior, the Providence Journal reports. The moment came as his workplace continues to treat a post-Thanksgiving wave of patients and is bracing for another wave after Christmas and New Year’s Day. “It’s this perfect storm – can we take care of everyone?” Arbelaez said. “Do we have capacity? Do we have front-line workers well enough? Those are all the things that worry me.” More than 20,500 people have received their first shots in Rhode Island, according to state health officials.
South Carolina
Columbia: Nearly 700 nonprofits are receiving state grants totaling $25 million to help offset costs during the coronavirus pandemic. The state Department of Administration announced Wednesday that 686 nonprofits would receive grants ranging from $2,500 to $50,000. Among the groups that got the money are arts organizations, churches and food banks. The grants can be used to cover expenses such as staffing and operating costs as well as personal protective equipment and revenue loss. The state had to turn down another several million dollars’ worth of requests, as a total of 1,590 nonprofits applied for $76 million in aid. The volume of requests led to a two-week delay in notifying winners. That delay had put more stress on businesses already strained by the pandemic, Frank Knapp, president of the state’s Small Business Chamber of Commerce, told The Post and Courier. The monies were allocated by the Legislature in September to spend federal COVID-19 aid for South Carolina. The state is also issuing $40 million to small businesses affected by the pandemic.
South Dakota
Sioux Falls: A federal judge says a state court can’t use the COVID-19 pandemic as an excuse to delay a Codington County trial. U.S. District Judge Charles B. Kornmann also criticized South Dakota’s response to the pandemic, saying it has done “little, if anything,” to mitigate the spread of COVID-19. Kornmann ordered that unless the Codington County state court resolves Matthew Kurtenbach’s May 2019 case by Jan. 15, Kurtenbach will win a federal petition he filed claiming wrongful imprisonment and a violation of his right to a speedy trial. “South Dakota cannot ‘take advantage’ of its own failures to follow scientific facts and safeguards in entering blanket denials of the rights of speedy trials,” the judge wrote. Kurtenbach petitioned the court at least 25 times for a right to a speedy trial. At one point, Kornmann directly criticized Gov. Kristi Noem’s actions during the pandemic. “The Governor has steadfastly refused to impose a statewide mask mandate. She has often questioned publicly the scientific fact that mask wearing prevents the virus from spreading,” the judge wrote.
Tennessee

Memphis: The Shelby County Health Department will begin vaccinating workers and residents at congregate care facilities, including nursing homes and assisted living facilities, this week, the department said Saturday. The health department started vaccinating first responders with the Moderna vaccine Dec. 28 and is continuing to vaccinate law enforcement officers, firefighters and paramedics, said spokesperson Joan Carr. Doug McGowen, chief operating officer for the City of Memphis, said there are 50,000 health care workers and 6,000 first responders in the Shelby County community, and “it’s going to take a while” to get all of those individuals vaccinated. Some people in priority group 1a2, which includes funeral home workers and people who are 75 or older, have also been vaccinated by the health department. As of Saturday afternoon, all the available weekend appointments for vaccinations at the department’s two drive-thru centers had been filled. The health department has also started vaccinating staff at mass COVID-19 testing sites.
Texas
Dallas: Coronavirus hospitalizations fell slightly Saturday but remained near their record high, as health officials said there were about 600 intensive care beds available across the state of nearly 29 million people. Texas reported 12,319 COVID-19 patients in hospitals Saturday, ending five consecutive days of record-breaking hospitalizations. But even with the decrease of more than 160 patients from Friday, the virus continued to strain medical resources. Intensive care units in several parts of Texas were full or nearly full, with 626 ICU beds available statewide Saturday, according to the Texas Department of State Health Services. The department reported 96 new fatalities, as well as 3,995 newly confirmed cases of COVID-19 and 487 probable cases. The actual number of cases is believed to be far higher because many people haven’t been tested, and some who get sick don’t show symptoms. Over the prior seven days, nearly 1 in 5 coronavirus tests in Texas came back positive, according to data from Johns Hopkins University.
Utah
Salt Lake City: Less than a quarter of the 127,375 doses of COVID-19 vaccine reportedly received in the state have been used to vaccinate health care providers and long-term care facility residents and staff as of the end of the year, Deseret News reports. “The initial rollout of the vaccine has been slow, slower than anticipated, slower than we wanted,” said Rich Lakin, immunization program director with the Utah Department of Health. “We hope to be at a much faster pace in the next 15 days.” Utah is already starting to speed up the process, health department spokesperson Tom Hudachko said Thursday. More than 6,000 doses were reportedly administered in the state Thursday, double the daily increases earlier in the week. What’s making the difference, Hudachko said, is that local health departments, including tribal clinics, and long-term care facilities are able to give doses much faster than hospitals. In Davis County, a mass drive-thru clinic at the Legacy Events Center is able to vaccinate 28 health care workers at a time with appointments, he said. At long-term care facilities, CVS and Walgreens and other contractors are quickly inoculating both residents and staff.
Vermont
Stamford: The town has voted to overturn in its community Gov. Phil Scott’s emergency orders issued with the intention of protecting the state during the COVID-19 pandemic. The select board of the town of about 800 people along the Massachusetts border voted 3-2 Tuesday to “terminate” the governor’s restrictions. The three board members in favor of the idea cite a section of Vermont law that they believe allows them to reject the governor’s order. Select board member Daniel Potvin said during the meeting that quarantine requirements, restrictions on large family or public gatherings, and face mask requirements “violate the constitution” in part because they were imposed without normal due process of law. He asserted it was important to stand up against such measures because it could lead to more loss of personal freedoms later on. Scott hasn’t enforced the orders heavy-handedly, he said, “but that could change.” Potvin said Friday the town is expecting some type of legal action from the state of Vermont, but “until it’s cleared up, the governor’s orders are still in effect.”
Virginia
Richmond: State Sen. Ben Chafin has died after contracting the coronavirus, Senate Republicans said Friday. Chafin represented southwest Virginia and was from Russell County. A Republican, he was first elected to the House of Delegates in 2013 and then moved to the state Senate in 2014. He was 60. Lawmakers from around the state mourned Chafin’s death late Friday. “I knew Ben as a lawmaker, an attorney, a banker, and a farmer raising beef cattle in Moccasin Valley, working the land just as generations of his family had done before him,” Gov. Ralph Northam said. “He loved the outdoors, and he loved serving people even more.” Senate Republicans said in a statement: “He served to ensure that his region and community, and the people he loved, would never be forgotten.” Chafin is the first Virginia lawmaker to die from the virus.
Washington
Vancouver: Quartz Mountain Distillers was surprised last week by a $14,060 fine from the U.S. Food and Drug Administration for producing hand sanitizer, but the company found out the next evening that the fee is not being enforced. Owner Randy Kyle said the distillery began making hand sanitizer in April. The family owners gave almost all of it away to help local health care workers remain safe, the Columbian reports. All distillers that made hand sanitizer during the COVID-19 pandemic were facing the fine. The Department of Health & Human Services on Thursday announced it was directing the FDA not to enforce the fine after the FDA received heavy backlash on social media. “Small businesses who stepped up to fight COVID-19 should be applauded by their government not taxed for doing so,” the Department of Health & Human Services said on Twitter. Kyle said he was unaware of any fine from the beginning of the pandemic. If the company were forced to pay it, he would have to closed down. “I’d just have to lock the door and walk away,” he said.
West Virginia
Charleston: The state has reported a weekly record in the number of positive coronavirus cases entering the new year. West Virginia had at least 6,915 confirmed virus cases for the six-day period last week, excluding Sunday, according to health statistics. Officials have cautioned that figures could be skewed due to a lag in reporting cases over the Christmas holiday period. Sunday’s cases won’t be reported until Monday. Still, the state had its three highest daily figures last week since the start of the pandemic: at least 1,385 positive cases Tuesday, 1,618 Wednesday and 1,516 Thursday. Last week’s cases marked the ninth weekly record in the past 13 weeks. The previous record of 6,871 positive cases was set two weeks ago. There also were a record 810 people hospitalized for the virus Friday. As of Saturday there were a record 27,418 active cases of the virus statewide, up 57% in the past month.
Wisconsin
Grafton: What was initially thought to be a major human error of someone damaging 57 vials of the coronavirus vaccine at the Aurora Medical Center Grafton has since grown into a federal investigation. A pharmacist at the facility intentionally removed 57 vials of the Moderna coronavirus vaccine from the refrigerator and left them out overnight knowing that the vaccines would be “useless” to those who received them. On Dec. 26, Aurora gave 57 people the vaccine from the tampered vials. After further review, the vials were discarded, and an investigation began. On Wednesday, Aurora notified Grafton police, and it became public that the vials were left out intentionally. The pharmacist was arrested Thursday. The FBI and the U.S. Food and Drug Administration were also investigating, police said. Jeff Bahr, president of Aurora Health Care Medical Group, called the pharmacist a “bad actor.” According to Grafton police, the now-former pharmacist intentionally took the vials out of the refrigerator and left them out overnight knowing it would render the vaccines “useless” and make people who received them believe they were vaccinated when they were not.
Wyoming
Cheyenne: Bars and restaurants across the state will be allowed to return to normal operating hours beginning next Saturday as COVID-19 hospitalizations decline in the state. Gov. Mark Gordon made the announcement last Saturday, praising businesses for adapting to health orders and thanking “the people of Wyoming who recognized the strain on their hospitals and health care workers and acted accordingly,” The Wyoming Tribune Eagle reports. “These have not been easy times for anyone,” he said. “We are not out of the woods yet, but continued personal safety measures while the vaccine is being distributed will enable our state’s schools and businesses to continue to remain open.” The updated health orders allow bars and restaurants to resume on-site consumption from 10 p.m. to 5 a.m., and they allow gyms to increase the number of participants in group fitness classes from 10 to 25. Counties can still opt out of the requirements if local conditions move to safer levels in accordance with White House metrics.
From USA TODAY Network and wire reports
This article originally appeared on USA TODAY: Oxygen supplies, wasted vaccines: News from around our 50 states

