The pace of coronavirus vaccinations now may determine whether or not we'll need a perpetual cycle of new shots to combat variants
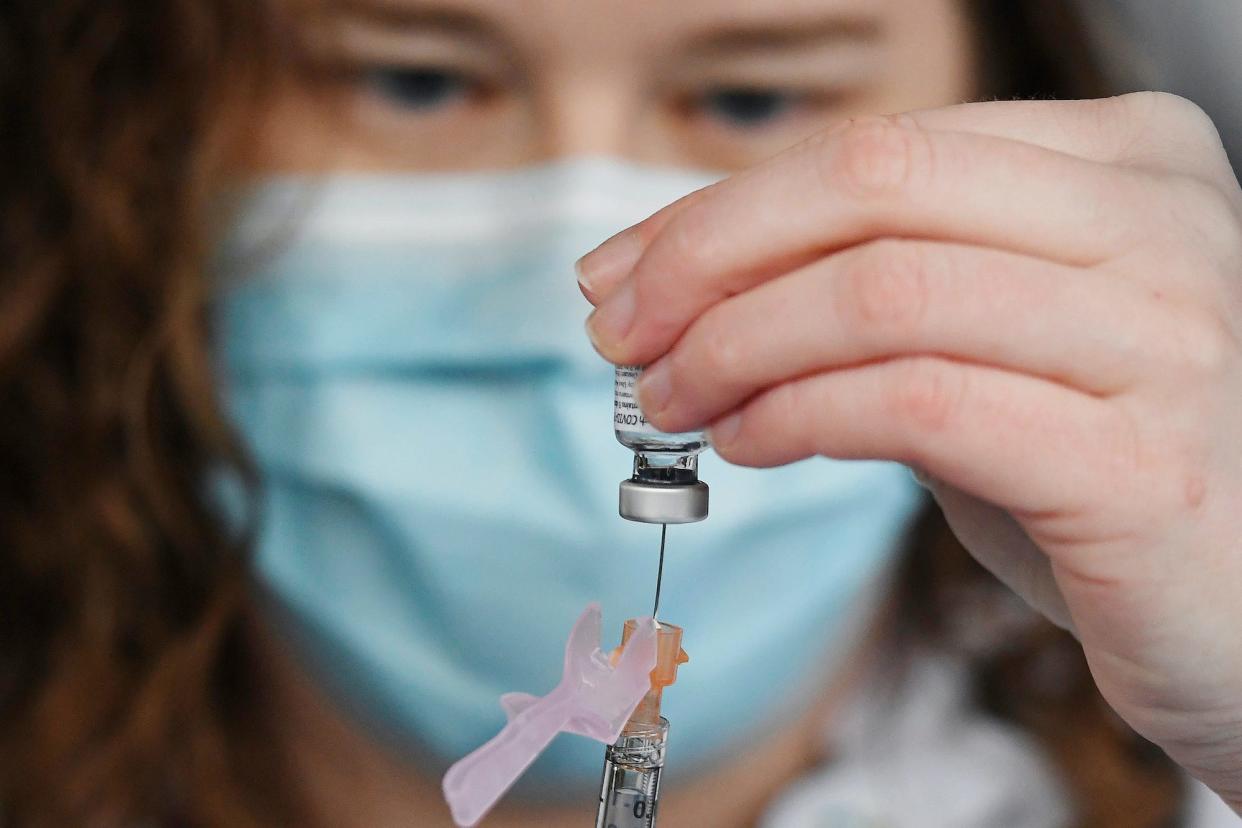
Scientists worry that vaccinations aren't proceeding fast enough to prevent new, perhaps deadlier coronavirus strains from emerging.
New variants that can evade existing vaccines could create a cycle in which people need to keep getting new coronavirus shots for years.
UK officials said Friday that the variant identified there could have a higher mortality rate than the original, though the evidence is "uncertain."
The global vaccine rollout is racing against the clock: New, more infectious variants of the coronavirus are spreading worldwide, and it's unclear how well existing vaccines work against these strains.
For now, vaccines seem effective against the strain identified in December in the UK, called B117. But preliminary research suggests vaccines may be less effective against B1351, the strain identified in South Africa.
"It is all the more reason why we should be vaccinating as many people as you possibly can," Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, said on Thursday. "Viruses don't mutate unless they replicate, and if you can suppress that by a very good vaccine campaign, then you could actually avoid this deleterious effect that you might get from the mutations."
But the process of getting shots into arms is off to a slow start in many countries. The US has administered more coronavirus vaccines than any other nation, but it has only given out roughly 19 million doses as of Friday.
Scientists worry that the current pace of vaccinations may allow time for too many new strains to emerge. That could lead to a scenario in which scientists must update vaccines regularly.
Michael Worobey, a viral evolutionary biologist at the University of Arizona, recently told the BBC that the emergence of new coronavirus strains could be "a glimpse into the future where we are going to be in an arms race with this virus, just like we are with flu."
It's also possible that a deadlier strain will turn up before most people are vaccinated. In that case, coronavirus shots may be routinely required for young people, similar to polio or measles vaccines.
The coronavirus could eventually resemble the common cold

The coronavirus' future depends heavily on our ability to control transmission quickly. The more people develop immunity - whether through natural infection or vaccines - the faster the virus will reach an endemic state, meaning it would circulate perpetually but no longer hit pandemic-level peaks.
In a recent study, researchers at Emory University and Pennsylvania State University suggested that the coronavirus could eventually resemble a common cold that infects people during childhood.
Under that study's most likely scenario, kids would get their first COVID-19 infection, on average, between ages 3 and 5. Almost every kid would get infected by age 15. Since pediatric infections are generally mild, there would be no need to vaccinate children beforehand. Infants might also have a certain degree of immunity at birth.
"For the first six months or so of life, or maybe longer if you're nursing, kids have maternal antibodies from their mother, both from the umbilical cord and from breast milk, so there's a chunk of time in the first year or so of life when kids aren't going to get a primary infection," Jennie Lavine, the study's lead author, told Insider.
The researchers estimated that reinfections would be even milder - and might even boost immunity against related coronavirus strains.
If vaccinations proceed quickly, the New York Times reported, the virus could reach this endemic state in as little as six months to a year. Fauci recently estimated that life could return to normal in the fall if 70% to 85% of Americans were vaccinated by the end of summer.
But based on observed patterns of other human coronaviruses, the researchers' model suggested that the new coronavirus would most likely become endemic within five to 10 years. Without speedy vaccinations, in other words, outbreaks could persist for some time.
Updating vaccines for new variants
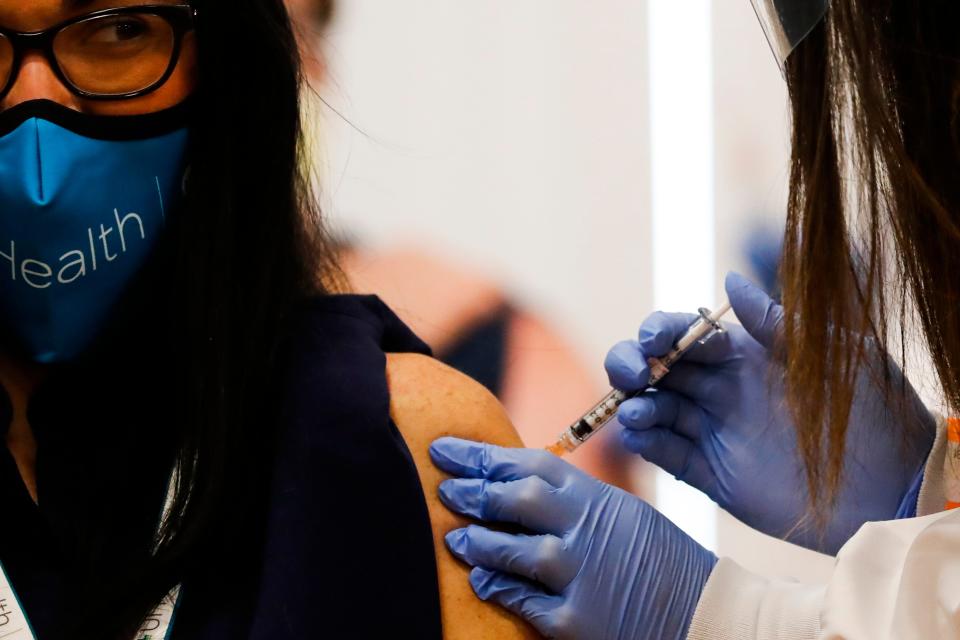
Vaccines trigger the production of virus-specific antibodies, so that if people get exposed to the virus after being vaccinated, those same antibodies will recognize the virus and destroy it before it has a chance to replicate widely.
In an ideal scenario, coronavirus vaccines would protect against all strains of the virus for several years.
But scientists worry that new coronavirus variants may be different enough from the original that they could evade the antibodies developed in response to vaccines. If that happens, scientists might need to constantly tweak vaccines' genetic instructions to vanquish new strains. The process isn't necessarily difficult, but it would mean people would need follow-up shots.
"If we ever have to modify the vaccine, that is not something that is a very onerous thing," Fauci said Thursday. "We can do that, given the platforms we have."
But a scenario in which new strains require people to get revaccinated regularly - as is already the case with flu shots - becomes increasingly likely the longer it takes to get the current shots into arms.
It's also possible, though, that other layers of immunity may protect people from emerging strains. White blood cells known as T cells and B cells also remember foreign invaders, often for longer periods of time than antibodies. A recent study suggested that recovered coronavirus patients had robust T-cell and B-cell immunity for at least eight months. A study of SARS, which is caused by a genetically similar coronavirus, showed that recovered patients had T-cell immunity 17 years after their infection.
A deadlier strain could make coronavirus shots routine

By vaccinating people quickly, public-health officials hope to avoid the worst-case scenario: the emergence of a deadlier coronavirus strain.
"Things that we need to keep looking for that would prevent this from becoming a very mild, endemic thing that doesn't require vaccination would be if somehow the virus changed such that infections in childhood became more severe," Lavine said.
In that case, she added, all young people would need to get shots before they acquired their first coronavirus infection.
There's already some evidence that the UK coronavirus strain could be deadlier than original. The UK's chief scientific adviser, Patrick Vallance, said Friday that the new variant could have an up to 30% higher mortality rate among some age groups, though the evidence remained "uncertain."
The good news, however, is that existing coronavirus shots seem to work against it.
"From what we've seen so far, the variants being described do not alter the ability of neutralizing antibodies elicited by vaccination to neutralize the virus," Moderna's chief medical officer, Tal Zaks, said at the JP Morgan Healthcare Conference earlier this month.
But that makes the task of vaccinating people all the more urgent.
"Everyone will probably get infected sometime," Lavine said "Let's make it an infection after the vaccination so that you don't get really sick from it."
Read the original article on Business Insider

