Panic, then neglect: Prior pandemics gave us lessons to fight the coronavirus. But funding dried up.
WASHINGTON – One virus came from an unusual kind of cat and killed hundreds of people. Another was blamed on pigs and killed 18,000 people worldwide, two-thirds of them in the USA. A third came from camels, killed hundreds and remains more lethal than the others.
Each of these respiratory viruses, which sparked worldwide panics during the past 20 years, offers lessons in how to battle the new coronavirus that has sickened more than 1.2 million people around the world.
Public health agencies in the USA are hampered in putting those lessons into action because they haven't spent enough time and money preparing between crises. Public health funding at every level of government has spiked feverishly during outbreaks, only to stagnate or fall after the outbreak dissipated.
“Every time we have an infectious disease emergency, you see a lot of interest in funding and robust response, and then that disappears when these events recede from the headlines. We have this cycle of panic and neglect, panic and neglect,” said Amesh Adalja, a senior scholar at Johns Hopkins University’s Center for Health Security.

No two pandemics are alike
Health experts joke that if you’ve seen one pandemic, you’ve seen one pandemic. That’s because transmission rates and the severity of illness vary from virus to virus.
Severe Acute Respiratory Syndrome, which swept the world from China in 2003, infected 8,096 people and killed 774. But it didn’t spread easily among people. Limiting interactions with civet cats in China restricted the outbreak. The Centers for Disease Control and Prevention still doesn't allow those animals to be brought into the USA.
Swine flu, the nickname for a strain of H1N1, sickened 61 million Americans and killed 12,469 after erupting in North America in early 2009. A vaccine was widely distributed by that November, after the pandemic peaked. The remedy is incorporated in the annual flu vaccine.
Middle East Respiratory Syndrome is more lethal than the others – some estimates say it killed a third of those infected. That has limited its spread because people die before they can sicken others. After emerging in Saudi Arabia in 2012, the virus that originated with camels has largely remained in that region. There have been 2,494 lab-confirmed cases and 858 deaths.
In comparison, the new coronavirus pandemic infected more than 823,000 people worldwide and killed more than 40,000 by Tuesday, according to figures compiled by Johns Hopkins University.
"This is a virus that can spread easily, can spread surreptitiously and can cause severe disease, for which we have neither a vaccine nor demonstrably effective treatment," said Harvey Fineberg, former provost of Harvard University and former president of the Institute of Medicine (now called the National Academy of Medicine). "This mix is a real new danger."
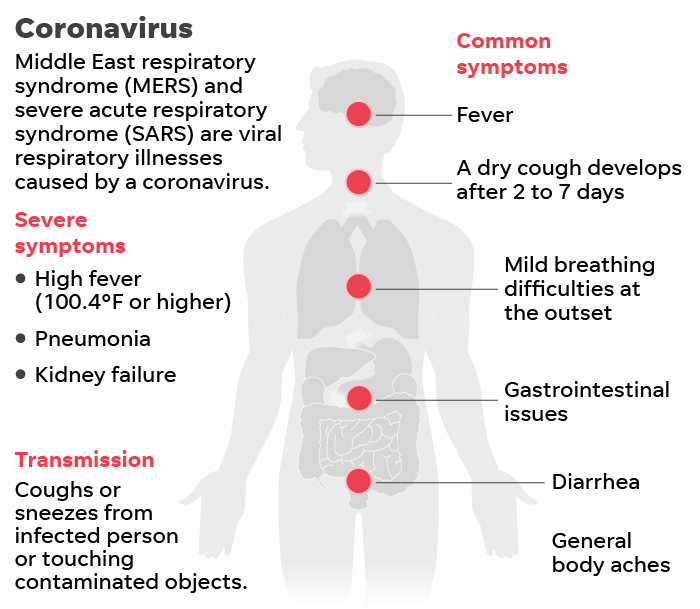
Coronavirus was identified quickly – but it took time to raise the alarm
Ann Marie Kimball, a professor emeritus in epidemiology at the University of Washington who worked on the SARS outbreak, said technology improvements allowed researchers to identify the new coronavirus in about a week rather than the month it took for SARS.
Chinese authorities isolated the virus Jan. 7 and shared the genetic sequence Jan. 12, so countries could develop tests.
“The transparency recommendation internationally in the scientific community has definitely got legs,” Kimball said, and there has been “terrific progress” in Chinese science and technology.
As an unfamiliar pneumonia spread, political leaders in China, then in the USA were initially reluctant to acknowledge the severity of the outbreak, she said. “This seems to be a knee-jerk first thing for leaders, to say, ‘Oh, this can’t be as bad as you’re telling me it is,’ ” Kimball said.
The Chinese government notified the World Health Organization on Dec. 31 about a pneumonia outbreak with an unknown cause in the city of Wuhan. There were 44 cases by Jan. 3. The virus spread to Thailand, Japan and South Korea by Jan. 20.
The first case may have been as early as Nov. 17, although it wasn’t recognized at the time, according to Chinese reports. U.S. officials said China should have notified the rest of the world as the number of cases grew in mid-December.
“I don't know if you'd say China is to blame,” President Donald Trump said. “Certainly, we didn't get an early run on it. It would have been helpful if we knew about it earlier.”
How SARS, MERS and H1N1 shaped coronavirus response
Though China didn't alert the World Health Organization until Dec. 31, it did track a handful of cases in mid-December under guidelines WHO adopted after the SARS and MERS outbreaks in 2005.
Those regulations were tested for the first time in 2009 during the H1N1 pandemic. In 2014, Fineberg reviewed how they worked in The New England Journal of Medicine and found lessons that apply to the coronavirus pandemic.
He found “outstanding performance” in identifying the pathogen and developing diagnostics. He also discovered vulnerabilities in national and local public health capacities, difficulties in decision-making and concerns about international cooperation.
“The world is ill-prepared to respond to a severe influenza pandemic or to any similarly global, sustained and threatening public-health emergency," Fineberg concluded.
Fineberg told USA TODAY the Chinese "did not do well" in the earliest days of the new coronavirus because they tried to suppress information and chastised doctors who reported it. One of those doctors contracted the illness and died.
Then China mobilized, quickly developed a test and locked down Wuhan to hinder further spread of the virus.
"We see the pluses and minuses in that response," said Fineberg, who was named this month to chair a standing committee on infectious diseases under the National Academies of Sciences, Engineering and Medicine. It has convened experts on the response to COVID-19 for the White House Office of Science and Technology Policy.
Other countries have demonstrated how to contain and treat coronavirus.
"Singapore is a very interesting lesson," Fineberg said. "They have been able to manage and keep it at a very low level."
That country suffered greatly from the SARS outbreak. This time, it aggressively tested and isolated those infected with or exposed to the virus that causes COVID-19. Authorities measured the temperature of anyone entering a public building. The result: 1,189 confirmed cases and six deaths as of Saturday, according to Johns Hopkins.
South Korea deployed widespread testing and treated patients with symptoms separately from others in standard clinical settings.
"The worst thing you could do is bring infected people or those who have a higher risk of infection into proximity with a lot of people suffering other illnesses," Fineberg said.
South Korea has had 10,156 cases and 177 deaths as of Tuesday, according to Johns Hopkins.

Public health funding tends to follow a crisis
Public health funding to respond to emergencies – whether at the global, national, state or county level – has spiked during outbreaks. Afterward, it has returned to the baseline or dropped.
“If you’re not having a crisis, and you have to make hard decisions about where you’re going to fund, you tend not to fund the things that may happen – you tend to fund the things that are happening,” said Craig Fugate, a former head of the Federal Emergency Management Agency.
“Over time," he said, "we have cut back and cut back and cut back our public health services, particularly at state and local levels.”
The response to the Ebola outbreak in 2015 in West Africa followed a typical pattern. U.S. funding for global health security from the Centers for Disease Control and Prevention, the Agency for International Development and the Pentagon generally ranged from $390 million in 2006 to $486 million in 2020, according to the Kaiser Family Foundation.
During the height of the Ebola outbreak, the three funds combined for more than $1.3 billion.
“When health crises strike – measles, MERS, Zika, dengue, Ebola, pandemic flu – and the American people grow alarmed, the U.S. government springs into action,” the Center for Strategic and International Studies reported in November. “But all too often, when the crisis fades and the fear subsides, urgency morphs into complacency. Investments dry up, attention shifts and a false sense of security takes hold.”
Federal public health grants to states for three key programs has declined from a peak in 2003, according to a Government Accountability Office report in May 2018.
Those programs strengthen state and local health departments, provide for surges in hospital capacity for infectious diseases and support labs. Funding peaked at a combined $1.4 billion in 2003. It declined until 2014 before recovering slightly by 2017, according to GAO.
From 2003 to 2020, hospital preparedness grants were cut nearly in half. Public health preparedness grants fell more than 20%, according to the Trust for America's Health.
“Congress should prioritize funding for health care preparedness even after this outbreak is under control,” Nadine Gracia, chief operating officer for the Trust for America’s Health and a former chief medical officer in the office of assistant secretary of Health and Human Services, told the House Homeland Security Committee on March 10.
The $2 trillion package to deal with COVID-19 passed last week includes $250 million in hospital preparedness grants and $100 billion for hospitals and the health care system. Those grants are supposed to cover losses or expenses related to the crisis.
In announcing the deal, Senate Majority Leader Mitch McConnell, R-Ky., called it a “war-time level of investment” that would “rush new resources onto the front lines of our nation’s health care fight."
Adalja, the Hopkins scholar, said respiratory viruses will remain a threat forever because they infect people so easily.
"We need to be very prepared for other respiratory virus threats, not just coronavirus, not just flu," he said.
"When a new respiratory virus appears and it shows an ability to be communicable in humans," he said, "we have to jump into action very quickly with diagnostic testing, vaccine development and antiviral development."

States are short on equipment to fight the coronavirus
The neglect portion of the public health funding cycle has become apparent as states and hospitals scramble for equipment such as masks and ventilators.
New Jersey has spent $1.8 million per month responding to the coronavirus, Christopher Neuwirth, an assistant commissioner for the New Jersey Department of Health, told a House Homeland Security Committee on March 10.
Before the surge of federal assistance approved last week, the state received a total of $1.75 million from the CDC for acute care facilities, emergency medical services and health departments, he said.
“Recognizing that medical supplies are facing a historic shortage and that health care supply chains are nearly frozen for respirators, disinfectants and other personal protective equipment, we urge you to consider additional funding to New Jersey and the distribution of items from the strategic national stockpile,” Neuwirth said.
New York Gov. Andrew Cuomo estimated the state needs 30,000 ventilators to care for the expected surge in patients. The federal government had provided 4,000 as of last weekend.
Cuomo said New York competes against other states to buy ventilators, so the price for each one has risen from $20,000 to $50,000.
"We need to give our ... health care professionals the supplies they need, and we need to do it now," Cuomo said Monday. "We're building a stockpile. The word 'stockpile' by definition means not for immediate use. It means you are preparing for a battle to come."
'On-the-job emergency training': Hospitals may run low on staff to run ventilators for coronavirus patients
Shortages aren't a surprise. Kim Saruwatari, the public health director in Riverside County, California, told a state legislative hearing a year ago that the county was prepared to respond to short-term emergencies, not a pandemic.
“When you consider our global society and the ability of diseases to spread worldwide in a matter of days, preparedness is critically important,” Saruwatari said.
“Funding shortages have caused staff reductions in many areas," she said, which is especially challenging during a natural disaster or pandemic.
Riverside County, about 50 miles east of downtown Los Angeles, has 2.4 million residents. Its public health budget is $100 million a year, Saruwatari said. The $12 million contribution from the county general fund has been flat for years amid competing priorities.
“Do they have the capability to respond to a large-scale, long-term public health emergency?" she asked. "No, not with our current infrastructure.”
Will we learn from the coronavirus pandemic?
Some officials expect a government commission, similar to the one after the Sept. 11 terror attacks, will be set up to review the nation's response to COVID-19.
“We need a somewhat brutal assessment of what worked, what didn’t work and what we can do differently,” said Fugate, the former FEMA chief.
Providing enough funding will always be difficult, Fugate said, but there could be changes in regulations and legislation.
For example, Fugate said the Stafford Act, which is typically used to provide federal relief during natural disasters, could be changed to explicitly deal with pandemics. Trump declared a national emergency for coronavirus under the Stafford Act, but as he noted, the law had never been used before for a public health crisis.
Another option would be to produce some medical or emergency equipment domestically, focusing on tools that are used rarely but critical in a crisis. Given that a significant percentage of protective masks are produced in China, Kimball said, the U.S. government should have ramped up domestic production for health care workers and the general public.
“You could have pulled that trigger two or three weeks ago," Kimball, the University of Washington professor, said while under lockdown.
If the country can’t stockpile crucial equipment such as ventilators, Fugate suggested a mechanism could be created to sound the alarm when a threat emerges. The federal government could invoke the Defense Production Act, which Fugate called a “sledgehammer,” to direct industries to manufacture critical equipment.
Trump invoked the act Friday to direct carmaker General Motors to produce ventilators. The company had already assigned hundreds of workers to the task as governors and hospitals sought the equipment.
“We’ve got to get past this idea that we’ll have too much,” Fugate said. “I think we’re going to run out of stuff faster than they realize.”
This article originally appeared on USA TODAY: Coronavirus: How SARS, MERS, H1NI gave lessons on funding, treatment

