Pfizer's and Moderna's vaccines likely work for all existing coronavirus strains. Don't worry about mutations for now, scientists say.
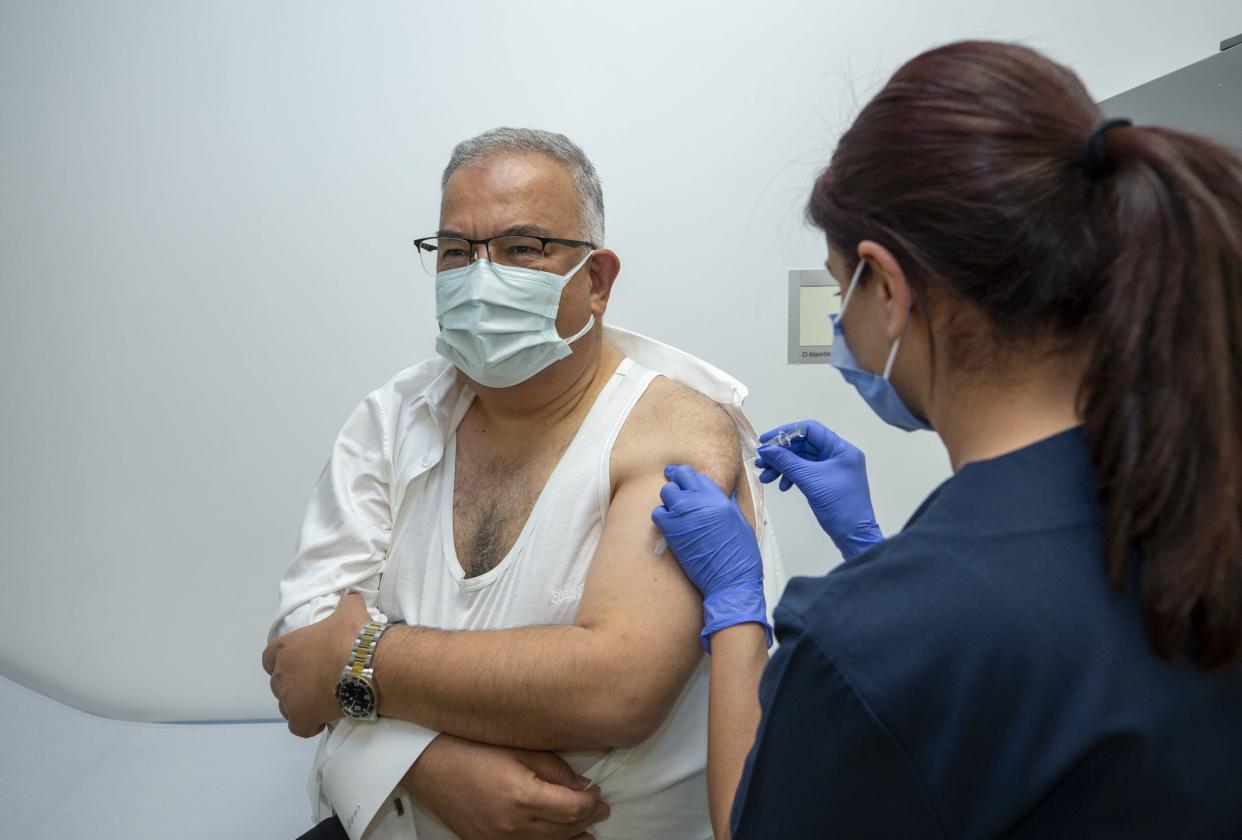
The coronavirus vaccine candidates from Pfizer and Moderna both prevented COVID-19 in clinical trials.
Research suggests the coronavirus is genetically stable, which means it mutates very slowly.
So the leading vaccines should work well long-term against all strains of the virus.
By contrast, viruses like the flu accumulate genetic errors more quickly, which is why a new vaccine is needed each year.
Don't worry about mutated strains of the coronavirus, experts say — the leading vaccine candidates should protect you against every version of the virus they've seen.
Moderna and Pfizer each announced this month that their coronavirus vaccines prevent COVID-19 — the former's is 94.5% effective, while the latter's is 95%. Both companies hope to get approval from the FDA in the coming weeks.
Genetic evidence about the virus so far suggests that these vaccine candidates — and others in the race — are unlikely to need much tweaking in the future. That's because the coronavirus, SARS-CoV-2, mutates slowly — its genome remains relatively stable over time.
So any vaccine developed to target the original virus should work in the long-run against different versions that arise as it subtly evolves over time.
"All SARS-CoV-2 to date are very genetically similar," Lucy van Dorp, a researcher at University College London's Genetics Institute, told Business Insider. "While most vaccines were designed with the original Wuhan reference genome as a target, I would be surprised if there would be big differences in efficacy against the major SARS-CoV-2 lineages at this stage."
The coronavirus mutates far more slowly than the flu

All viruses accumulate genetic errors over time as they replicate. Some of these mutations can affect how well they infect hosts or how virulent they are. But the speed at which a virus mutates matters.
The flu virus, for instance, mutates relatively quickly, which is why scientists create a new vaccine each year to keep up. But according to Emma Hodcroft, a geneticist at the University of Basel in Switzerland, there are only 20 to 25 differences between all existing versions of the coronavirus — across a genetic sequence of 30,000 building blocks.
"People are getting the same virus now that we saw in the spring," Hodcroft previously told Business Insider.
Van Dorp estimated that the coronavirus accumulates about two mutations per month.
"This rate is about half that estimated for influenza," she said, adding, "given the slow rate of evolution, it is hoped that vaccines won't need to be regularly redesigned."
Trevor Bedford, an infectious-disease expert at the Fred Hutch research center in Seattle, estimated that "it will take the virus a few years to mutate enough to significantly hinder a vaccine."
One reason for the virus' slow mutation rate, van Dorp explained, is that SARS-CoV-2 has a protein that proofreads its genetic code as it replicates and corrects errors.
So in looking at its behavior, she added, "no single mutation seems to have had a very marked impact."
People might need booster shots, though
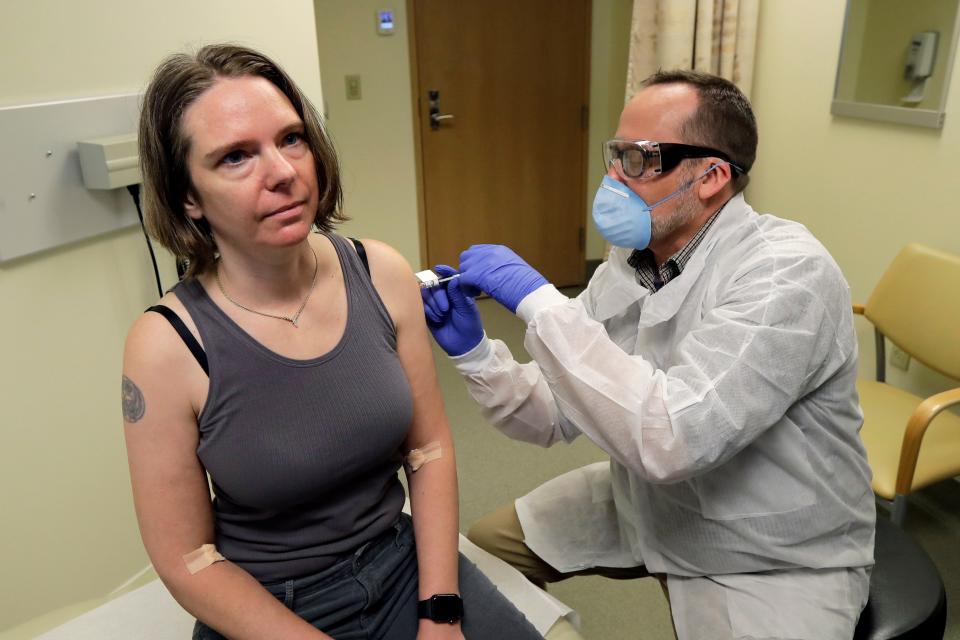
Scientists haven't been able to study the coronavirus long enough to determine how long immunity might last.
Some evidence suggests people could get reinfected. But that's not because of new, distinct strains, which are the primary reason we need a new flu shot each year. Rather, research has found that that coronavirus antibodies may dissipate after weeks or months.
"If immunity does turn out to be fleeting, we'll need a plan of a vaccination plus a booster, or revaccination at periodic intervals," Marm Kilpatrick, a disease ecologist, previously told Business Insider.
But antibodies are just one layer of the immune system; T cells can outlast antibodies and also help find and destroy the virus. Plus, even if people do become susceptible to reinfection after some period of time, that's not a deal-breaker — it's what booster shots are for.
"This happens for a lot of vaccines," Florian Krammer, a vaccinologist at the Icahn School of Medicine at Mount Sinai, previously told Business Insider. "It's not a problem. You can get revaccinated."
'Escape mutants'
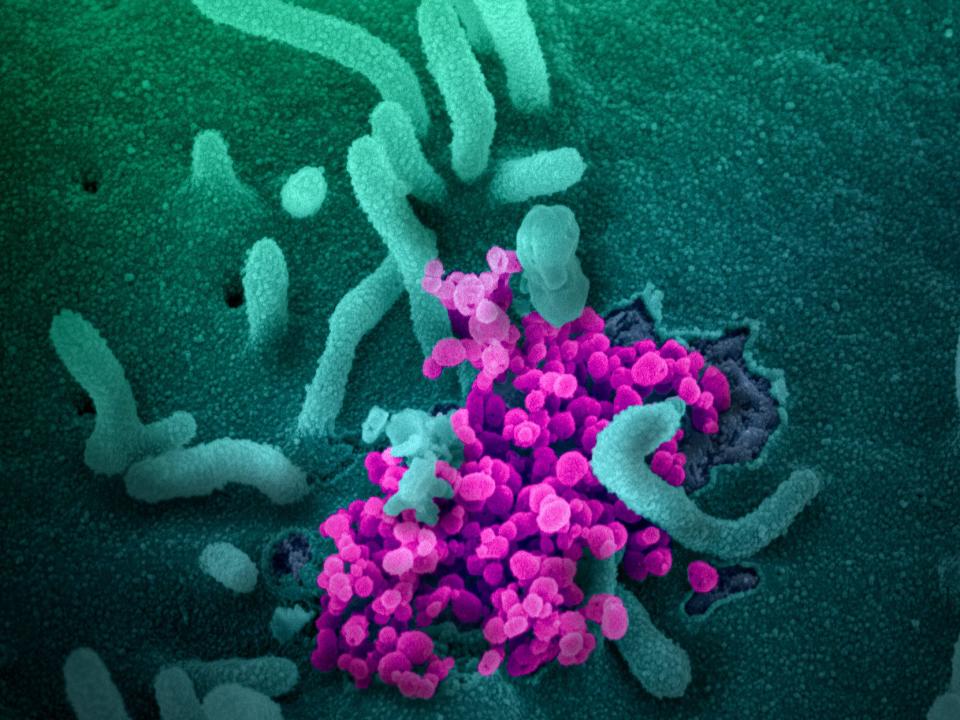
As vaccine roll-outs approach, researchers like van Dorp are keeping an eye out for mutant coronavirus strains that evolve to escape the antibodies our immune systems generate. Such strains could undermine a vaccine's effectiveness.
"These are referred to as escape mutants," van Dorp said.
In particular, scientists are monitoring changes in the part of the coronavirus' genome that codes for the shape of its spike protein. The spike is what the virus uses to invade our cells, and it's also how most vaccines and antibodies target the virus. So a possible tweak there could make it easier for the virus to infect our bodies and harder for our immune systems to destroy it.
According to van Dorp, there are some virus variants with partial resistance to antibodies circulating already, but at a very low frequency.
"These have already been flagged and are being monitored closely," she said.
Genetic monitoring also revealed that one version of SARS-CoV-2 became more prevalent worldwide than the original virus that emerged in China: a strain with a mutation that affects the shape of the spike protein. But there is not yet any definitive evidence that this mutation is the reason that lineage of virus came to dominate — it could simply be luck and circumstance. Plus, there's no reason to think a vaccine wouldn't be effective on that strain.
Bedford predicts that we'll see occasional mutations that enable SARS-CoV-2 "to partially escape from vaccines or existing herd immunity."
But again, he said, "this process will most likely take years rather than months."
Read the original article on Business Insider

