Sarasota Memorial used good judgment and proper procedures in fighting COVID
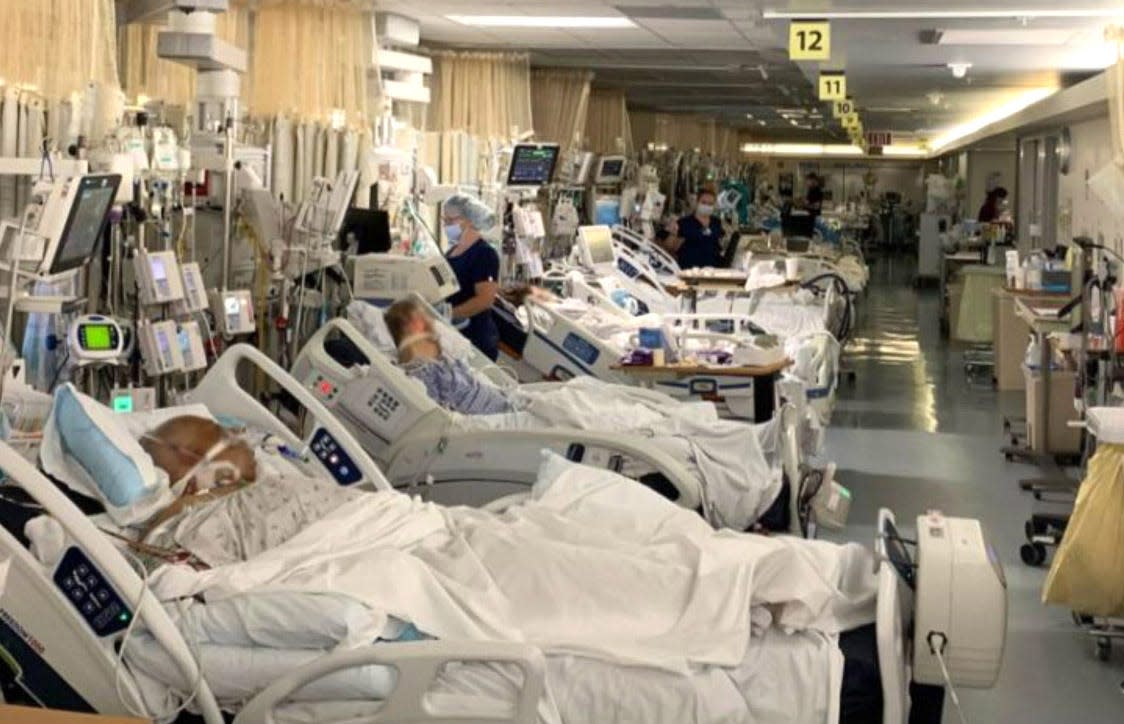
As health care professionals and drug developers, we would like to reinforce the points that were made in a March 26 letter to the editor titled "Extremists make hospital their new target.”
The four of us have more than 100 years of combined drug development experience, and we have worked for major pharmaceutical corporations and biotech companies. Collectively, we have developed and brought many drugs to the marketplace. In addition, we thoroughly understand the regulatory process for traditional drug development as well as the Emergency Use Authorization process granted by the Food and Drug Administration to quickly bring COVID vaccines, diagnostics and treatments to the public during the pandemic.
A gradual process
The biology of the virus that causes COVID was not very well understood when it first hit the shores of our country in early 2020, and medical experts gained new insights on a daily basis regarding the pattern of the disease spectrum it caused – as well as proper ways to treat it.

Initial papers published in early 2020 from France and China appeared to show that hydroxychloroquine could inhibit the growth of COVID in test tubes and block the virus from entering cells, thus causing its more rapid disappearance from the nose and throat in patients. However, these were small, preliminary studies that were not rigorous or well-controlled, and they had numerous other methodologic limitations. Indeed, many additional early trials were plagued by similar issues.

Subsequently, more than 50 larger, more rigorous clinical studies were conducted which showed no clinical efficacy of hydroxychloroquine in either early- or late-stage disease – and the Centers for Disease Control and Prevention and Food and Drug Administration cautioned against hydroxychloroquine's use given the lack of benefit and potential toxicity.
In fact, as early as June 15, 2020, the Food and Drug Administration stated hydroxychloroquine showed no benefit for decreasing mortality or speeding clinical recovery.

Similarly, early studies of ivermectin – a drug used in veterinary and human medicine to prevent and treat parasitic worm infections – also showed a decreased ability of the virus to replicate in laboratory settings, and early, small studies in humans showed some potential benefits. However, when larger, definitive and well-controlled studies were conducted, they did not show evidence of clinical efficacy.

In addition, studies have shown that in order to achieve the concentrations in patients necessary to produce the effects observed in test tubes, much higher doses of ivermectin (one hundredfold greater) than the doses approved for human use would be required. At these doses, there would be a potential for serious side effects; for example, there might be issues involving central nervous system toxicity – such as tremors, balance issues and seizures.
An exceptional job
The health care professionals at Sarasota Memorial Hospital did an exceptional job treating patients infected with SARS-CoV-2, and the hospital scored in the top 5% of all hospitals in America with respect to positive clinical outcomes across all degrees of COVID severity.
Clinicians need to practice evidence-based medicine. To achieve the best outcomes, treatment protocols developed by infectious disease and intensive care physicians need to be followed in accordance with therapeutics authorized by the Food and Drug Administration and treatment algorithms recommended by the Centers for Disease Control and Prevention.

This is exactly what was done at Sarasota Memorial, and with much better than average overall patient outcomes.
Philip Chaikin, Debra Kimless, Thomas Newman and Randy Sleet are all retired or semi-retired physicians/scientists who live in the Suncoast region. None of the four authors has an affiliation with Sarasota Memorial Hospital.
This article originally appeared on Sarasota Herald-Tribune: Sarasota Memorial used good judgment and science to fight COVID

