The side effects you need to know about before switching to the coil

Choosing the right contraception can be a daunting task, but if you - like many other women - are considering the coil, one of the first things you need to be clear about are the possible side effects.
Dr Sonal Shal, an NHS GP, spoke with Cosmopolitan UK about what to expect from the new contraception, and when you should seek help if you're worried about the effects it's having on your body:
What is the coil?
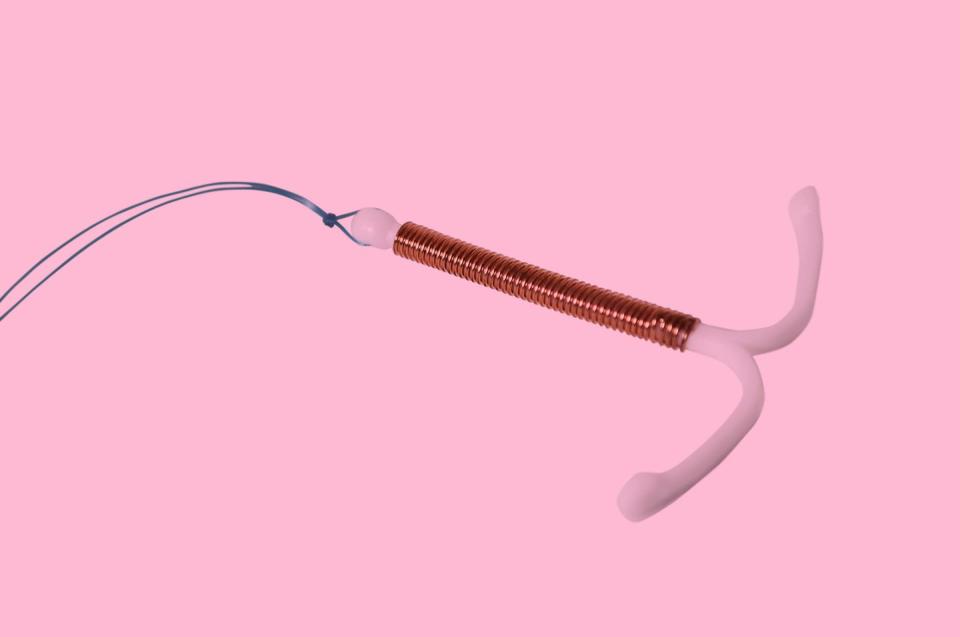
The coil is a form of contraception used by thousands of women all over the world. It's a small, T-shaped plastic and copper device (hence it's also known as the copper coil) that's put into your womb by a doctor or nurse.
When inserted correctly, it is more than 99% effective, making it one of the more reliable contraceptive options.
Before you have a coil inserted a doctor will take a thorough medical and sexual history to ensure that it is the safest option for you. They may also take some swabs to look for infection, or check to ensure there is no risk of pregnancy. It is important to mention if you have had any unprotected sex or at risk of sexually transmitted infections.
What are the different types of coil?
There are two types of intrauterine (meaning inside the uterus) coil; a copper coil, also known as the intrauterine device (IUD) and a hormonal coil, also known as the intrauterine system (IUS) . They both have slightly different mechanisms of action and therefore slightly different side-effect profiles.
The hormonal coil (usually Mirena or Jaydess) is also used as first line treatment for pain.
What are the side effects of the coil?
The most common side effect from both coils is changes to bleeding patterns.
Dr Sonal explains: "In the 3-6 months following coil insertion, women may experience irregular, prolonged or frequent periods, but this usually improves with time.
"For many women their periods can stop all together, and this is particularly true for women using the hormonal coil - which is often recommended to women who have naturally heavy or painful periods."
Other side effects can include:
Abdominal cramping
Weight gain
Vaginal discharge
Headaches
Breast tenderness
Acne.
However, as with any form of contraception, these can vary for each individual.
"All women are different and it is difficult to determine who will experience problems and who won’t, explains Dr Sonal - however, she adds: "In the wide majority, these symptoms will settle in the first few months after insertion."
And, while the Pill can increase your chances of developing breast cancer, Dr Sonal says: "There is no link between breast cancer and use of the hormonal coil."
Risks of the coil
When inserted properly by a nurse or doctor, the risks of the IUS or IUD are extremely minimal; but, of course, there are things to be aware of.
"In the rare instance that you do fall pregnant with the coil inside then you are at increase risk of an ectopic pregnancy (pregnancy occurring outside the womb) and this requires immediate attention," Dr Sonal says. "So any woman with the coil who develops sudden onset, severe lower abdominal pain, with or without bleeding should ask to speak to a doctor."
Following insertion, you'll be taught how to check that your coil is still in place. Dr Sonal says: "In around 1 in 20, the coil may spontaneously expel it self and this is most common in the first year of use, particularly within 3 months of insertion. So it is important that you follow your doctor's advice and learn to check the coil strings regularly, particularly after your period.
"If you can't feel your strings, then avoid any unprotected sex and see your doctor."
There's also a very tiny chance that insertion could go wrong. "Another rare complication is perforation of the uterus (making a hole in the uterus) at the time of coil insertion. However, doctors inserting the coil must have strict training and in experienced hands this is very unlikely." You can minimise these risks by ensuring you're fitted by a doctor you trust, or going to an NHS sexual health clinic for your appointment.
Oh, and you'll be glad to know that there's no existing evidence to support the idea that libido is affected with the use of the coil, so sex should feel entirely normal.
When you should see a doctor about the coil
If you're worried about any of the above, it's best to book an appointment with your GP to check things over.
Dr Sonal says:"Women should medical assistance at any time if they develop symptoms of pelvic infection (pelvic pain, smelly vaginal discharge, or pain) or any new abnormal bleeding.
"If there are any ongoing concerns, please contact your doctor or talk to a specialist doctor or nurse in a sexual health clinic. They can discuss with you whether the symptoms you are experiencing are because of the contraception.
"If it is thought they are, they can easily remove the coil and most symptoms will fully resolve."
If you've done your research beforehand and feel that the coil is the right contraception for you, chances are you'll feel totally happy with your decision.
For more information, visit the NHS website.
Follow Abbi on Instagram.
('You Might Also Like',)

