As Tennessee sees lack of maternal care, it's increasingly 'dangerous to be pregnant' in rural areas

PARIS, Tenn. — Lacy Crawford is on her fourth pregnancy. Two were miscarriages, and this one already has her doctors worried about another medical emergency.
Problem is, the nearest obstetrician is in Jackson — more than an hour away by car.
The hospital in her northwest Tennessee town of Paris, population 10,316, closed its birthing center this month. The loss means Crawford is scrambling, mid-pregnancy, to find new health care providers. A center in Murray, Kentucky, is closer, but patients on TennCare would not be able to use it.
As a nurse who has worked in a birthing center, Crawford knows how quickly this scenario can go terrifyingly wrong.
"I've seen emergency cesarean sections that showed up and the baby was out in 10 minutes," Crawford said. "So it's scary to see that an hour's drive could make a difference in the lives of me and my baby if an emergency was to happen."
'Maternity care deserts'
It’s an increasingly common obstacle in small towns: Hospitals cannot afford to keep expensive delivery centers open. More and more, communities are simply without vital obstetricians and gynecologists, often referred to as OB/GYNs. These “maternity care deserts” affect more than 2.2 million U.S. women, according to a 2022 report by the March of Dimes.
Nearly one-third of Tennessee counties lack quality care for expectant mothers, according to the March of Dimes report. What's more, the report found that 27% of Tennessee women live more than a half-hour from a birthing center. That’s roughly three times the national average.
No wonder Tennessee had the nation’s third-highest rate of maternal deaths between 2018 and 2021, according to the health analysis organization.
John Tucker, CEO of the Henry County Medical Center, blames low reimbursement rates for TennCare, which covered about 70% of deliveries at hospitals. Tennessee officials also refuse to expand eligibility for Medicaid as envisioned by the 2010 Affordable Care Act. As a result, Tucker added, the region has experienced a decline in birth rates since 2020.
“There's nothing we'd like to do more than restart our OB program because I think it's one of those core services," Tucker said. "But there literally wasn't a way for us to stay (financially solvent) if we continued."
What is Tennessee's maternal mortality?
The Tennessee Department of Health is expected soon to release an annual report on maternal mortality, showing an increasing number of women enduring delivery complications that sometimes lead to death.
Fewer birthing centers mean complications are likely to continue to worsen, said Nikki Zite, a professor and vice chair of education and advocacy in the Department of OB/GYN at the University of Tennessee Graduate School of Medicine.
“We expect maternal morbidity and mortality to be significantly higher with both the Dobbs decision (the Supreme Court ruling overturning Roe v. Wade) and a lack of access to abortion and hospital closures,” said Zite, who is a physician. “We will also see an impact on the neonatal side with more birth complications for newborns.”
Crawford, the pregnant nurse, said she worries about that, too.
She still needs to make at least 10 more trips to the OB/GYN before her delivery for routine checkups. When the due date approaches, she and her husband will simply have to drive to the hospital.
Expanding care in rural areas: Southern rural hospitals face uncertain post-pandemic future
She has a toddler at home and can't afford to pack her up and stay at a hotel closer to the hospital in Jackson.
"We've had a couple of appointments in Jackson, and I'm confident in the care they provide," she said. "But the fact is that care is at least an hour away."
Birthing centers not financially viable
Henry County Medical Center announced in May that it would close the birthing center in September, noting that it would now only provide gynecological services.
During a recent visit to the center, staff members remained optimistic that the hospital could find a way to reopen. They're even keeping much of the medical equipment used in the center. But the financial prospects don't look good.

Tucker said about 70% of patients who delivered at the hospital were on TennCare, the state's Medicaid provider. Most of those patients were enrolled in a Blue Cross Blue Shield coverage program called "BlueCare." Tucker said BlueCare pays about $1,700 for the mother's stay and $335 or $458 for each baby, no matter how long they remain in the hospital.
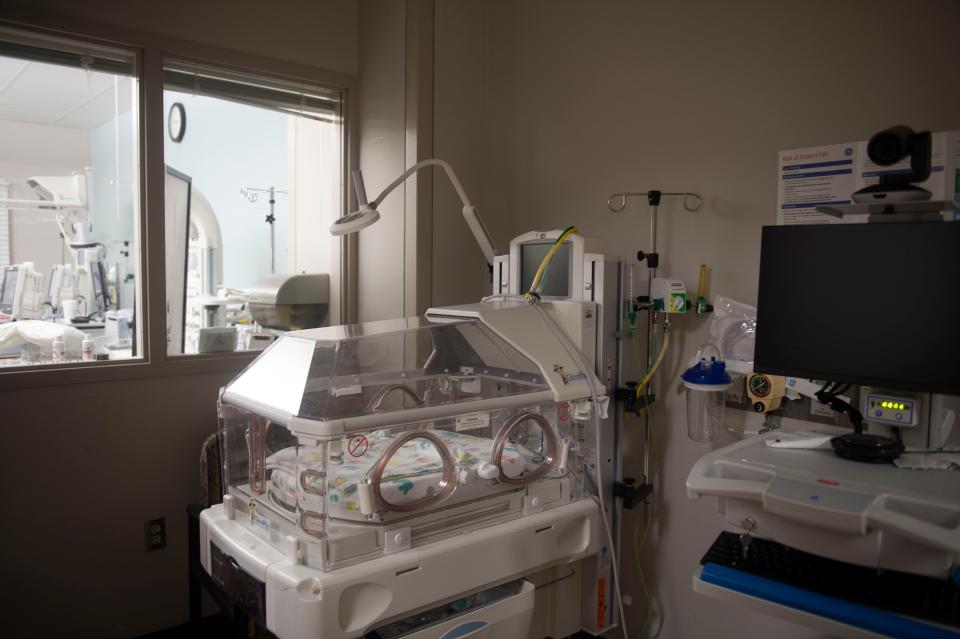
"If a baby is in the neonatal nursery for two days, three days or 10 days, we get paid $400 to take care of that baby," he said. "You can't stay at a Super 8 for two nights for $458, let alone a neonatologist-attended nursery."
While most babies only stay in the hospital for one or two days, every two newborns are attended to by a nurse. The unit also must pay for an on-staff neonatal physician to care for the babies, Tucker said. That doesn't include the cost of equipment upkeep and operating a 24/7 surgery center — which includes a pharmacy, respiratory therapy, staffing and so on.
In total, Tucker said the center was losing about $4.5 million a year before the closure.
Alison Sexter, a spokesperson for the BlueCare program, said hospital representatives asked for a 500% increase in rates in the spring, a figure BlueCare called "untenable." The insurer also offered to increase payments for all hospital services, Sexton said. Sexton also blamed the hospital's declining number of patients.
"Again, HCMC faces several challenges, some of which are not necessarily isolated to the facility but plague many rural hospitals across the country," Sexter added in an email, noting that there are "more than 25 providers" accepting TennCare within 50 miles of the hospital.
Indeed, the hospital has seen a drop in the number of deliveries since the COVID-19 pandemic, officials said. But, even so, the health center has delivered between 500 and 600 babies a year, said Dr. Pamala Evans, an OB/GYN there.
The Henry County Medical Center delivered twice the number of babies last year than it did in 2018, when McKenzie Regional Hospital closed about 20 miles away, Evans said.
More potential for maternal, birthing complications
To better understand the hole such closures create, consider what already doesn't exist around the Paris community.
To the south, Carroll County already operates without obstetrical services. Same for Benton County, located east of Paris and Stewart County, directly to the northeast.
All of the nearest hospitals that accept TennCare are about an hour away.
"Even if we fly someone from our hospital, it's 30 minutes to the closest hospital by helicopter ride," Evans said. "So, if you're hemorrhaging or if you're in pre-term labor, it's just not going to happen."
Women living in rural areas are 9% more likely to suffer complications from their pregnancies because of this lack of access, according to the March of Dimes study.
"A person's ability to have a healthy pregnancy and healthy birth should not be dictated by where they live and their ability to access consistent, quality care," March of Dimes CEO Elizabeth Cherot wrote in a statement last month. "But these reports show that, today, these factors make it dangerous to be pregnant and give birth for millions of women in the United States."
A worsening problem
The March of Dimes noted in data released last month that the problem is worsening across the country.
It found there has been a 4% drop in the number of U.S. birthing hospitals since 2018 and more than 5.6 million women live in areas with no or inadequate care. That means 70 additional counties have been classified as maternity care deserts since that time, the report found.
It also discovered that U.S. states with the highest rates of care shortages are largely rural.
The American Hospital Association reported recently that 74% of such closures in rural communities are in states that did not expand Medicaid or had only recently done so. Other problems include difficulty in recruiting staff to such rural locations and high rates of burnout.
Zite, the Knoxville OB/GYN, blames a lack of Medicaid expansion and the challenges of recruiting young doctors to rural communities, where there are already few doctors.
"The younger generation of OB/GYNs are looking for better work-life balance," Zite said.
"Committing to a practice without a shared call pool of at least three to five other people is not something most new grads are looking for. So, when you only have one or two docs in a community, recruiting is very hard."
Frank Gluck is the health care reporter for The Tennessean. He can be reached at fgluck@tennessean.com. Follow him on Twitter at @FrankGluck.
Want to read more stories like this? A subscription to one of our Tennessee publications gets you unlimited access to all the latest political news, plus newsletters, a personalized mobile experience, and the ability to tap into stories, photos and videos from throughout the USA TODAY Network's daily sites.
This article originally appeared on Nashville Tennessean: Lack of Tennessee pregnancy care makes it 'dangerous' in rural areas

