The truth about do not resuscitate orders
The deadly coronavirus is sweeping the country, putting thousands of people into hospital and killing more than 7,000.
But some groups including the disabled, frail, elderly and those with chronic long-term conditions have been left scared that if they become ill they could be denied treatment; doctors may impose what are known as do not attempt resuscitation orders (DNARs), which means if their heart stops doctors and nurses will not give them artificial respiration.
Scandal and furore over the use and misuse of DNARs is nothing new. The debate re-emerged after a clumsy and inconsiderate attempt by one south Wales GP surgery to write to at-risk patients asking them to sign a form by post.
In the days that followed, doctors attempting to explain DNARs on social media were compared to the Nazi “Angel of Death”, Josef Mengele — abhorrent and distasteful, to say the very least.
This week, the NHS’s chief nurse has written to hospitals warning them not to impose blanket do not resuscitate orders.
That we are in this situation is a travesty, and blame rests both on the medical profession and the rest of us for avoiding an honest, open debate about death and dying that has been sorely needed for too long.
Too many doctors, trained to cure sickness, have been reluctant to have conversations earlier with patients they cannot save. Equally, many families baulk at having these conversations with relatives before they reach the hospital bed.
Blame also rests on some media outlets that have fuelled the irrational fear of DNARs among members of the public with sensationalist reporting of what exactly is involved and what the rules are.
It is time for some facts.
First, we must all accept that death is inevitable. We want to be comfortable, without pain and at ease. To slip away as our heart stops beating — it will be among the last of our organs to shut down.
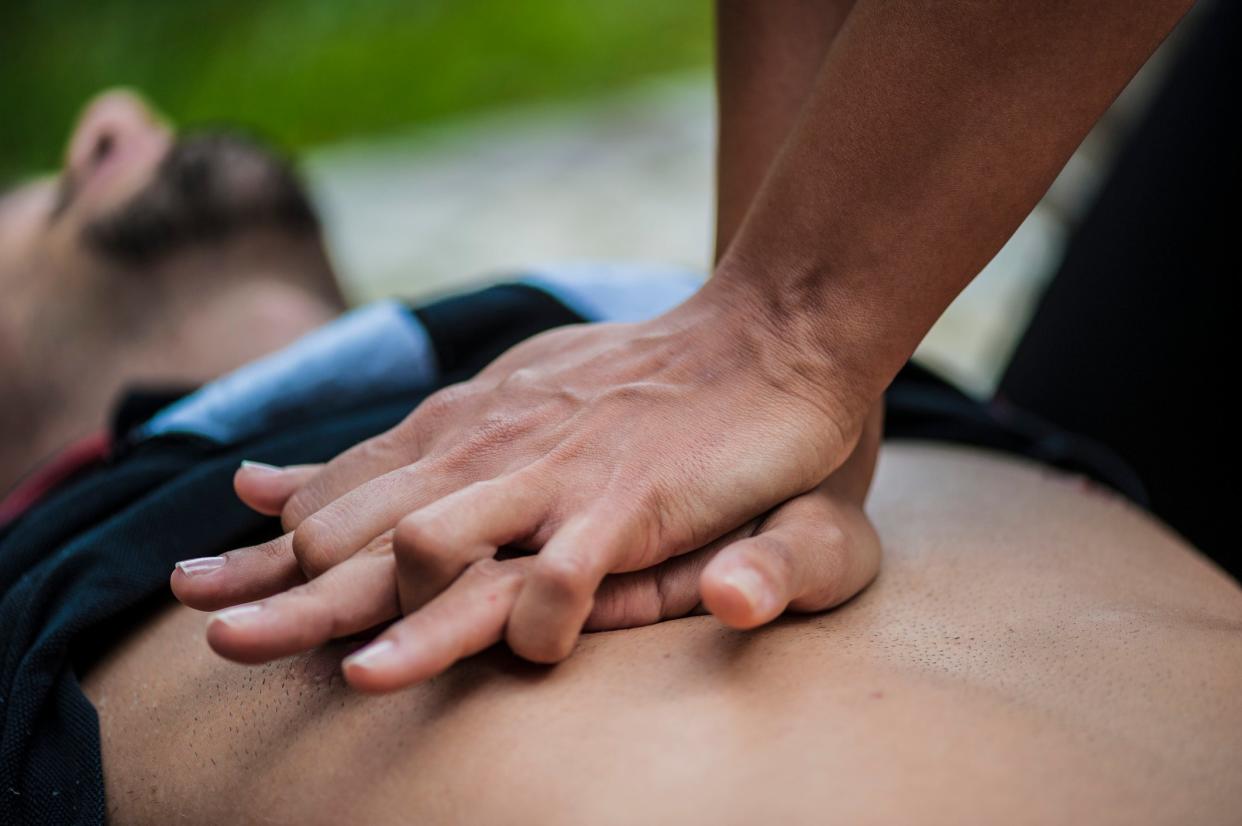
Receiving chest compressions is not the miracle cure for death that it has often been portrayed as. Fewer than half of people who receive CPR will be successfully resuscitated, and of those only around 20 per cent will actually leave hospital alive.
If you’re frail and elderly, CPR will more than likely break your ribs. You may end up enduring awful pain and discomfort in the days that follow.
Do not resuscitate orders exist to avoid this unnecessary brutality and to deliver the end that we would all hope for. DNARs do not mean patients are denied other treatment or food and water. When you’re dying the body does not need food or water, but this is a poorly explained fact that has contributed to much public anger in the past.
Doctors cannot just impose a DNAR without discussing it with the patient or their family. To do so could be unlawful, yet sadly it continues to happen and every incident fuels further mistrust.
In 2014, the law changed after a court battle brought by the family of Janet Tracey who died at Cambridge University Hospitals Trust in 2011. A DNAR was placed on Ms Tracey’s records without her knowledge or consent.
The court made clear that failure to discuss the DNAR with a patient was a breach of their human rights and that there should be a presumption in favour of involving the patient unless there were convincing reasons not to.
Patients being upset about these conversations is not a sufficient reason for doctors to avoid having them.
But while a patient must be involved, this is not a matter of consent. A doctor cannot be forced to carry out CPR if they think it will be futile.
These conversations are difficult at the best of times. Many nurses and doctors do it well, with compassion, on a daily basis and such conversations are a gift to families and patients. It allows them to say goodbye. Imposing a DNAR and not telling the family or patient, as in Ms Tracey’s case, denied the family the ability to have those important final conversations.
During the coronavirus outbreak, the NHS is under pressure like it has never experienced. Decisions will need to be made about who gets treatment, but this is nothing new. Doctors are forced to decide every day how far to go to try and save patients.
Access to intensive care is not an automatic right and for some people this is simply not a viable option regardless of coronavirus.
Blanket attempts at DNARs reveal the failure of some clinicians to start these necessary conversations sooner. Any patient or family who is concerned should discuss their wishes in advance and, if necessary, create an advanced directive stating what care they do not want to receive.
One consistent gap in end-of-life care in the NHS is the absence of a national policy on when and how decisions on resuscitation should be made.
Coronavirus has put into sharp relief, again, the need for a national public debate that both educates and informs clinicians and members of the public about each other’s equally valid perspectives on end-of-life care.
Read more
Tracking the coronavirus outbreak around the world in maps and charts
When can we really expect coronavirus to end?
Everything you need to know on supermarket delivery slots
The dirty truth about washing your hands
Listen to the latest episode of The Independent Coronavirus Podcast

