Visiting loved ones in hospital will have to wait till next year, doctors warn
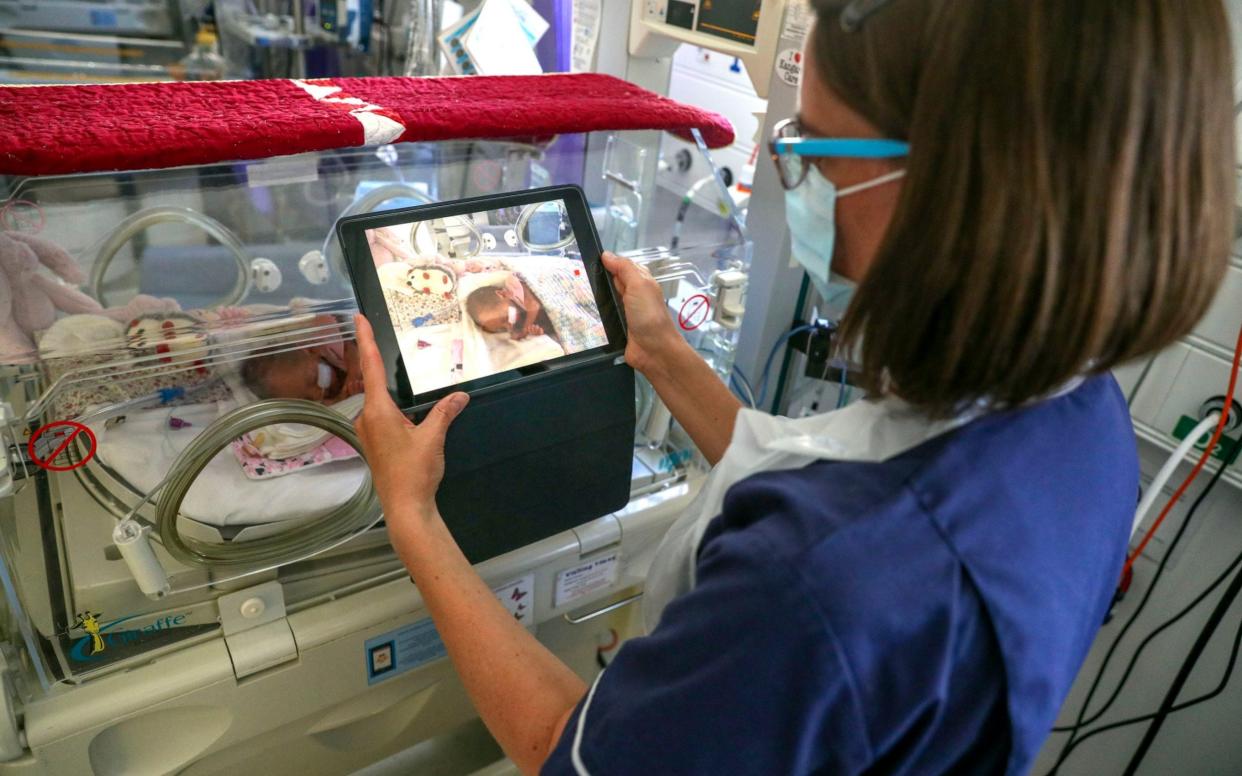
People will not be able to visit loved ones in hospital or attend routine outpatient clinics until “well into next year” despite falling numbers of coronavirus cases, senior doctors have warned.
The number of people admitted to hospital with Covid-19 has fallen significantly since January, with the impact of the lock down and vaccination roll-out now being translated into fewer patients admitted onto wards and intensive care units.
Latest Government figures show that the total number of patients in hospital suffering from Covid has more than halved, going from 38,839 on January 19 to 14,808 on Thursday, February 24.
The figures also show a significant drop in the number of Covid patients admitted to hospital on a daily basis, falling from the second wave peak of 4,576 on January 12 to 1,111 on February 23. The number of patients on mechanical ventilation has almost halved, from a second wave peak of 4,076, on January 22, to 1,971 on Friday.
But the Royal College of Physicians (RCP) has warned that this easing of pressure on the NHS will not see a return to normality for many months to come.
Professor Andrew Goddard, president of the RCP, told The Sunday Telegraph: “It will be a while before hospitals look like they did before the pandemic. Until we know if vaccination stops transmission of the virus and most of the population has been vaccinated, we will still have to restrict visitors and retain social distancing, doing as much as we can virtually, for at least the rest of the year and beyond.”
He added: “The days of simply walking into a busy hospital outpatient waiting room won't be back for a long time. Hospitals are safe places, but if we are to ensure they remain safe strict infection prevention and control will continue to be necessary.”

Professor David Oliver, a consultant in south east England with 31 years experience, said “The overall number of people in hospital with Covid has fallen quite dramatically and wards that were converted to all Covid are now being repurposed to non-Covid. But there’s no way that out-patient numbers will return to the volumes of before for quite a while and we will need to continue with remote consultations. And general family visits will only be phased back in very gradually.”
The RCP says that although Covid admissions are falling and hospitals are no longer being overwhelmed as they were at the height of the UK’s second wave, they continue to feel the pressure of the pandemic.
Figures for bed occupancy in England - including Covid and non-Covid patients - are currently as high as they were in December and January, at around 111,000. That is more than the 71,000 Covid and non-Covid beds occupied at the peak of the first wave, last April.
Between last April and December hospitals dealt with 18 million fewer out patients than normal and around 2.7m fewer elective operations.
“We’re still in quite a bad place, but it feels much better than it did a month ago because the pandemic is waning and the impact of the vaccine is being felt among older groups,” said Professor Goddard.
Consultants have warned that it will take many months to deal with the backlog of elective and planned surgery postponed as a result of the pandemic. Adding to the problem of the sheer volume of patients on waiting lists for routine surgery, is the fact that many hospital staff have been left physically and emotionally drained by dealing with Covid and that ICUs, needed for some post-surgical recovery, are still operating at capacity.
Professor Oliver said: “There's going to be a lot of catch-up needed in planned surgery work, but you’ve got a lot of staff who are exhausted. With many younger doctors especially pretty traumatised by what they’ve been through, getting Covid themselves or seeing colleagues die, and feeling betrayed by things like the lack of proper PPE.”
The age of patients being admitted to hospital with Covid has fallen, as the programme to vaccinate those aged in their 80s and over, which began in mid-January, begins to have an effect on infection rates.
Fatality rates for the over 80s have dropped by two thirds in the past six weeks, but have not yet fallen for the over 70s and below because the vaccination roll out has yet to cover as many in the lower age groups or reach levels of full protection.
As a result those currently being admitted to intensive care units with severe Covid are increasingly in their 70s and under.
"Hospitalisation for over 80s is falling at a faster rate than for under 70s because of the impact of vaccination,” said Professor Goddard, adding: “ICU admissions are increasingly younger people who have not yet been reached by the vaccination roll out."

