'This is a bad practice': Doctors question FDA protocol for plasma treatment of coronavirus patients
WASHINGTON — Jimmy Glenn, a one-time boxing instructor, opened his Times Square bar in 1971. The grandson of Southern sharecroppers, Glenn would keep his bar open through years of crime and grime, urban flight and terror fears. He kept it open right until mid-March, when New York Gov. Andrew Cuomo announced that all eating and drinking establishments in the state had to close because of the coronavirus pandemic.
Glenn had actually stopped coming to the bar a week before the order, his son Adam Glenn told Yahoo News. His father remained “isolated at home,” with no visitors but Adam.
But somehow the pathogen found the 89-year-old. Adam Glenn says his father became sick with COVID-19, the disease caused by the coronavirus, in the first week of April. He was hospitalized at NYU Langone Medical Center in Manhattan on April 12.
Adam Glenn became his father’s most ferocious advocate, pushing for every conceivable treatment. “I had to learn it to get what I wanted for my dad,” Glenn recalled. Among the treatments he received was hydroxychloroquine, the much-disputed malaria drug touted by President Trump but warned against by the medical establishment. It didn’t work. Neither did anything else, and so in early May, Adam Glenn pushed NYU Langone doctors for a treatment that had worked during the 1918 influenza pandemic and many times after that: convalescent plasma.

Recovering from an infectious disease usually leaves a patient with plenty of armaments, known as antibodies, against the infection. Those antibodies can be collected in the form of convalescent plasma and transferred to someone still battling the same infection, potentially providing the crucial boost the recipient needs to recover.
What those patients may not realize is that the medical establishment remains uncertain about a coronavirus treatment that has been available to Americans for more than a month. In its understandable rush to make convalescent plasma available, the FDA did not mandate that blood banks test the blood they collect for the very coronavirus antibodies that make the treatment promising. Of the three levels of testing donated blood for antibodies, only the least rigorous — and hence the least exact — is mandated.
That has put the medical establishment in an uncomfortable position, with many touting the treatment but some also warning against it. The epidemiologist S.P. Kalantri, of the Mahatma Gandhi Institute of Medical Sciences, recently denounced stories of convalescent plasma’s success as “just small anecdotes at best” and “not science.”
Medical ethicist Steven Joffe of the University of Pennsylvania sounded a similar warning. “I hope convalescent plasma proves effective,” Dr. Joffe wrote on Twitter. He explained that convalescent plasma could lead to the production of another treatment, called monoclonal antibodies (antibodies not taken from other people but produced in a laboratory).
To be sure, the FDA is relying on sound, decades-old science in advocating for the use of antibodies as a treatment. And the agency is, at the same time, supporting the kind of randomized clinical trials that will in the not-too-distant future yield definitive answers about how convalescent plasma should be used. That will take time, however.

NYU Langone, where Glenn was hospitalized, is enrolled in a protocol crafted by the FDA and executed by the Mayo Clinic, the renowned medical center headquartered in Rochester, Minn. Doctors who register with the Mayo Clinic have to declare that they are investigating the use of convalescent plasma. Doing so then allows them to use convalescent plasma on severely ill patients like Glenn.
There is nothing inherently unusual about the Mayo Clinic’s “expanded access” protocol, which is predicated on concepts of medical uncertainty and expediency. The FDA acknowledges that convalescent plasma is still “investigational” in nature, meaning its benefits have not been certified. That may not be an issue for severely ill patients like Glenn, who will try anything to save their lives. That is why “expanded access” protocols like this one are sometimes called “compassionate use.”
Doctors at NYU Langone, however, were reluctant to use convalescent plasma on Glenn. They were doing their own clinic trials, separate from the Mayo Clinic, intended to figure out just how convalescent plasma can be used to treat patients. But that study would take time, and time was something Jimmy Glenn did not have. And so Adam Glenn pushed for NYU Langone to give his father convalescent plasma through the Mayo Clinic protocol.
"I went through a very long battle with the hospital,” Adam Glenn recalls. Doctors at NYU Langone were hesitant to use the Mayo Clinic protocol, but Glenn kept pushing, and they finally relented.
In early May, Jimmy Glenn was administered one dose of convalescent plasma. It may have been too late for any treatment, given the various attacks COVID-19 launches on the respiratory, circulatory and other systems. Jimmy Glenn died on May 7.
While convalescent plasma did not save Glenn, it did not kill him either. Blood transfusion is safe and commonplace, never more so than when administered by a large, well-regarded hospital like NYU Langone. Adam Glenn believes his father was simply too ravaged by the disease to benefit from convalescent plasma.
Glenn’s plight does, however, highlight an uncomfortable truth about convalescent plasma: Promising as the treatment may be, it has been administered in what some say is a counterproductive manner. And while convalescent plasma has doubtlessly helped many people, its benefits have been blunted by what critics say is a haphazard federal response.
“We have no efficacy data at this time,” acknowledged a spokesperson for the Mayo Clinic, which received $26 million from the federal government to administer the expanded access program.

About 13,500 people have already received convalescent plasma through the Mayo Clinic, which requires doctors to register before connecting them to blood banks that have collected blood from recovered coronavirus patients. That blood should theoretically contain antibodies that could help another person fight off the disease by conferring what is known as passive immunity. And much of it doubtlessly does. But studies show that the antibody levels can vary wildly, which means that patients and their families are taking far more of a gamble than they realize.
“It’s a 4-month-old disease,” says Dr. Benhur Lee, a microbiologist at Mt. Sinai Health System in New York. “I think we just need more data.”
Gathering data takes time. And the coronavirus has already killed 330,000 people around the world, including more than 90,000 in the United States. That has led to approvals of “off-label” uses of drugs like hydroxychloroquine, ordinarily used to treat malaria, and remdesivir, which can be used against an array of viruses. The hope is that something will work before thousands more die.
That, at least, is the thinking behind the Mayo Clinic program. “I have never seen a blood product up and going as quickly as this one has,” says Cliff Neumark, a vice president at Vitalant, one of the blood banks that is participating in the Mayo Clinic plasma protocol.
The approach is a “leap of faith,” agrees Dr. Katharine Bar, who is running two convalescent plasma studies at the University of Pennsylvania. At the same time, she judged the FDA protocol as ultimately “appropriate,’ given the profoundly imperfect choices available.
The story of convalescent plasma is one of a federal medical establishment wanting badly to compensate for its slow response to the coronavirus.
In January, the Centers for Disease Control and Prevention rejected an offer of coronavirus diagnostic tests from the World Health Organization. Instead, CDC virologists thought they could produce their own diagnostic test. Mistakes hampered that effort and the diagnostic test did not become widely available until March. That means precious weeks during which the nation could have been fighting the pandemic were squandered.
Wanting to avoid a similar scenario when it came to convalescent plasma the FDA put a premium on speed, announcing its new convalescent plasma program on April 3. The following day, President Trump endorsed the treatment at a White House press briefing. “We have a great deal of enthusiasm for that,” he said, adding that convalescent plasma “shows a great promise” and “provides hope.”
On this point, Trump was aligned with both the scientific community and the media, which touted convalescent plasma with varying degrees of nuance. “America Needs Plasma From COVID-19 Survivors Now,” went the headline of an Atlantic article. The article explained why convalescent plasma may work and why it may not. Other media coverage offered a similar cautious optimism on convalescent plasma.
Months later, the uncertainty remains. “We don’t have any data to say that this approach will work or not,” lamented one pathologist who is running a convalescent plasma trial of his own in a Southern California hospital. Speaking under the condition that his name and affiliation remain undisclosed, the pathologist said that there was “tremendous pressure” on the FDA to jury-rig what looked like an investigational trial so that blood plasma could be provided to “very sick patients for compassionate use,” the way off-label drugs are.

A person can donate blood for the Mayo Clinic expanded access program if he or she received a positive diagnostic test for the coronavirus, then waited 14 days after symptoms of the disease disappeared. Around this time, the body should be producing high levels of antibodies, although there has been some suggestion that two weeks is too soon to donate blood for coronavirus convalescent plasma). But because that blood won’t receive a general antibody test — let alone a specific test for coronavirus-neutralizing antibodies — doctors won’t know the exact quality of the product they are administering (the donated blood is carefully screened for common diseases, making it highly unlikely it would sicken the recipient.)
“This is a bad practice,” says Dr. Alan Wu, a leading laboratory scientist at the University of California at San Francisco, speaking specifically of how a major New York blood bank was transfusing patients with blood that could entirely lack coronavirus-fighting properties. That blood bank has since begun testing for antibodies.
Many major blood banks, such as the Red Cross, are now conducting antibody tests on blood before sending it to hospitals enrolled in the Mayo program. But some are not, and none are required to according to the FDA, which is overseeing the entire effort.
In response to questions from Yahoo News, FDA spokesperson Michael Felberbaum explained that the agency’s protocol was guided by a desire to save lives, and a belief that convalescent plasma could do so. “Given the current urgent need, and because antibody testing might not be available, we are not recommending that antibody testing be performed before investigational convalescent plasma is administered to a patient,” Felberbaum told Yahoo News.
Another problem is that the accuracy of such tests has been questioned, and the FDA has allowed pharmaceutical companies to market tests that it has not independently validated. “We still do not have well-validated serologic assays,” the Southern California pathologist told Yahoo News (serology is the study of blood products, while “assay” is the scientific term for a medical test).
What’s more, most blood experts believe that the blood should receive an additional test, for neutralizing antibodies specifically capable of stopping the coronavirus. This is the third, and highest, level of scrutiny. Those more specific tests are “the gold standard,” says Dr. Lee of Mt. Sinai. But they are even more difficult to obtain than the less specific test that tells a patient whether he or she has any antibodies at all.
There is little outside incentive for blood banks to go through this additional testing, since general antibody and more specific neutralizing antibody tests will claim valuable resources and time and, in any case, the federal government is not requiring those extra layers of scrutiny.
And the more blood the blood banks shuttle to doctors treating coronavirus patients, the greater the eventual reimbursement they receive from the federal government. A spokesperson for the Department of Health and Human Services who could speak only on the condition of anonymity confirmed that reimbursement comes from Biomedical Advanced Research and Development Authority, or BARDA, a federal agency under HHS purview. BARDA’s administrator, Dr. Rick Bright, was recently demoted for refusing to endorse hydroxychloroquine, the malaria drug President Trump has continued to promote for treatment of the coronavirus.
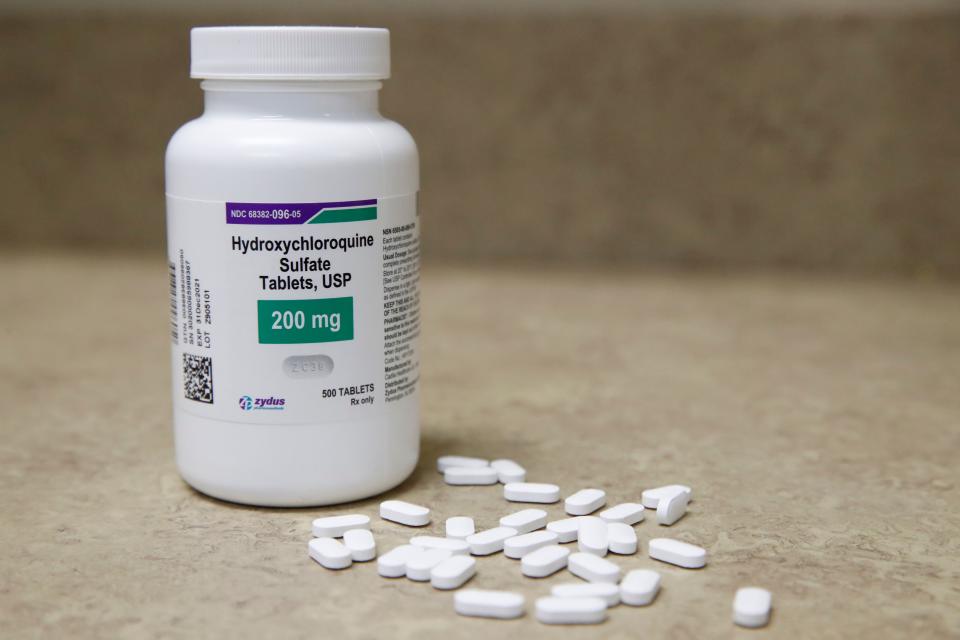
Transfusing blood does not carry anywhere near the same level of risk as using hydroxychloroquine, which is why blood banks have embraced the expanded access program, despite ongoing concerns about its efficacy.
“There are many unanswered questions regarding levels of antibody and types of antibody in the product, and what levels and types of antibody are most effective,” said Dr. Rita Reik, chief medical officer of OneBlood, one of the largest blood banks in the United States. She also holds the same title at America’s Blood Centers, a trade group that represents 600 blood centers across the United States, including those owned by Vitalant and the New York Blood Center.
Dr. Reik says participation in the Mayo Clinic program “will result in the collection of data that can be used to determine its actual efficacy.” Such data is more easily collected through randomized trials than compassionate use protocols. That tension between efficacy and speed is one medical ethicists and public health officials constantly labor to address.

What scant data is available show both promise and peril, with many questions remaining unanswered. Dr. Larry Dumont, the lead researcher for blood bank Vitalant, says that his preliminary investigations on blood samples indicate that about six of the blood products now being offered as convalescent plasma lack the Immunoglobulin M and Immunoglobulin G antibodies — known as IgM and IgG, respectively— that suggest the blood has value in fighting disease.
Yet unless they can act as neutralizing antibodies for that specific pathogen — in this case, the coronavirus— they are effectively useless. Little data exists on the levels of the ever-important neutralizing antibodies produced after a bout of coronavirus. That is largely a function of the speed with which the coronavirus has swept across the globe, accelerating but also complicating research and treatment.
“In an ideal world, it would be great to have a high throughput, sensitive and specific neutralizing antibody assay that could be applied to every donation in real time,” Dr. Dumont told Yahoo News. “Unfortunately, we are limited by biology and technology for the neutralizing-antibody test,” which he called “labor-intensive” and “time-consuming.”
Still, he justifies offering patients convalescent sera, despite its yet-undetermined value. “We have people in intensive care units,” Dr. Dumont said. “Convalescent sera might help them.”
After queries from Yahoo News, the New York Blood Center said it would begin doing the same thing. But thousands of people have donated blood of unknown antibody content. Nor is it clear whether small blood banks will also begin testing for antibodies absent a federal requirement to do so.
And though the risks of blood transfusion are low, they are not nonexistent. “Transfusion is not as safe as people think,” Johns Hopkins anesthesiologist Steven Frank said in 2012, upon the publication of a study highlighting those risks, which include potentially fatal infections like sepsis. Two years later, a University of Michigan study confirmed that when blood transfusions took place in hospitals, the risk of infection increased.

Above all, what researchers and doctors lack is sound data on how to administer convalescent plasma. One study cited by the FDA involved testing only five patients at the Shenzhen Third People's Hospital in Shenzhen, China. Those patients all improved after being treated with convalescent plasma, which had been tested for coronavirus-specific neutralizing antibodies. Doing such tests is the surest means of making convalescent plasma more than an exercise in flying blind.
There is no expectation that the FDA will mandate such tests, as they are not yet widely available. After all, even the more general antibody test is not a requirement of the FDA protocol. (Dr. Dumont of the blood bank Vitalant says that tests for binding antibodies, which are different from neutralizing antibodies, can serve as a reliable “surrogate.”)
Without accurate knowledge of what convalescent plasma contains, it will be impossible to say whether convalescent plasma is an effective treatment. One study published late last month, tested 175 recovering coronavirus patients in China for neutralizing antibodies. The results showed a staggering range: 14 percent showed high neutralizing antibodies, but 30 percent showed low and 6 percent had no coronavirus neutralizing antibodies whatsoever. There were also the 39 percent with “medium-high” neutralizing antibodies and 17 percent with “medium-low” neutralizing antibodies.
The concern that those who have recovered from coronavirus lack the necessary antibodies is more than theoretical. Molly DeMellier, a resident of Queens who recovered from the coronavirus, signed up for a convalescent plasma study at Mt. Sinai after a listener to her dating podcast told her about it. “I think I applied the day I started feeling better,” she told Yahoo News. Like many other coronavirus survivors, she wanted to help “in some small way.”

Mt. Sinai requires antibody tests on blood samples in advance of patients making full donations. A week after she went to Manhattan to take that first step, she received a phone call explaining the sample she provided “didn’t have enough antibodies to donate.” She was advised to try later, because the body may develop more antibodies as time goes on.
Some university laboratories have abstained from the Mayo Clinic protocol, electing to take a more measured approach. Dr. Jonathan Esensten, a colleague of Dr. Wu at UCSF, is running his own convalescent plasma trial.
“The risk is, if you’re not testing, you might be releasing convalescent plasma with low levels of antibodies,” Esensten told Yahoo News.
He added that some of the blood samples he has studied do not have sufficient antibodies to help patients, confirming what Dr. Dumont and others have found.
“If it’s not helping people,” Esensten said, “we need to stop.”
_____
Click here for the latest coronavirus news and updates. According to experts, people over 60 and those who are immunocompromised continue to be the most at risk. If you have questions, please refer to the CDC’s and WHO’s resource guides.
Read more:



